Mindfulness and the Brain: What Does Neuroscience Say?
 We have all heard the term “mindfulness” but what does it really mean in terms of the brain and in terms of neuroscience?
We have all heard the term “mindfulness” but what does it really mean in terms of the brain and in terms of neuroscience?
Being present in the moment is very empowering. It means focusing your awareness on the here and now. It’s about embracing each moment of the day and not worrying about what tomorrow may bring.
Living in the present moment can be transformative, but what does it do to the brain?
The human brain contains hundreds of trillions of synapses that help the brain cells communicate with each other. The brain contains anywhere from 80 to 100 billion neurons, which help form these connections.
Despite all of this, scientists still don’t have a full understanding of what actually happens in the brain when we practice mindfulness or meditate.
Our knowledge of the brain is really the tip of the iceberg because there is still so much more we need to learn.
In this article, we will take a look at the field of mindfulness research, examine certain studies, and look at how mindfulness affects and changes the brain.
Researchers are even looking into how mindfulness can help with things like ADHD and autism, which is very exciting.
Before you read on, we thought you might like to download our three Mindfulness Exercises for free. These science-based, comprehensive exercises will not only help you cultivate a sense of inner peace throughout your daily life but will also give you the tools to enhance the mindfulness of your clients, students, or employees.
This Article Contains:
- A Look at the Field of Mindfulness Research
- 7 Studies You Need to Know About
- 9 Benefits Research has Shown
- The Neuroscience of Mindfulness: A Look Inside
- How Mindfulness Affects and Changes The Brain
- Mindfulness Versus Medication: What Can We Prove?
- The Research On Autism and Mindfulness
- Can Mindfulness Help ADHD?
- A Take-Home Message
- References
A Look at the Field of Mindfulness Research
There are many studies, which have been done on mindfulness. Some of the most widely recognized include Mindfulness-Based Stress Reduction (MBSR) and Mindfulness-Based Cognitive Therapy (MBCT).
- Jon Kabat-Zinn and his colleagues at the University of Massachusetts Medical Center developed the Mindfulness-Based Stress Reduction program.
- The Mindfulness-Based Cognitive Therapy program was developed by Segal, Williams and, Teasdale.
Mindfulness-based stress reduction (MBSR) is a mindfulness-based program designed to assist people with pain and a range of conditions and life issues. These issues may also be issues that are difficult to treat in a hospital setting.
The MBSR course has been proven to help alleviate stress, anxiety, depression and chronic pain. It combines meditation techniques with cognitive behavioral skills and mindful movement and is taught in a way that is practical and relevant for everyday living.
The MBSR course is a wonderful example of how being mindful can help with many things beyond merely relaxing the mind and body and being present in the moment.
The goal of mindfulness-based cognitive therapy (MBCT) is to help people change thoughts that are unproductive. This might include patterns of thought that aren’t serving you well, or other types of behaviors and emotional responses.
MBCT uses psychological techniques that help patients better understand the correlation between various modes of the mind and mood disorders. When you recognize the connection, you can then work toward an appropriate answer.
You can use the strong connection between the mind and pain to change the way that you think. The therapy is also thought to be helpful in the recovery from the stress and depression associated with pain.
MBCT draws on the structure of MBSR integrating some approaches from Cognitive Behavioral Therapy and it is typically taught in an eight-week format for up to twelve participants.
An MCBT program typically contains:
- The cultivation of awareness through a mindfulness practice.
- A framework characterized by non-striving, acceptance, and a genuine interest in experience, which is incorporated into the teaching process.
- A process of linking the learning to an understanding of working with the idea of vulnerability.
Personal experiential learning is integrated into a wider framework of understanding. This understanding relates both to the nature of general human vulnerability and suffering and to the particular nature of vulnerability and to depressive relapse.
Typically the MBCT sessions are facilitated through dialogue, reflection, group exercises and teaching.
Although the term mindfulness-based cognitive therapy may be somewhat imposing, its meaning is very straightforward.
- M stands for Mindfulness, or bringing your awareness to the present moment without judgment or expectation.
- B stands for Based, as in derived from or connected to.
- C stands for Cognitive, which refers to the thinking, planning, and measuring parts of the brain.
- T stands for Therapy or the treatment of illnesses and disease.
Cognitive behavioral therapy or CBT is one of the most highly recommended and well-respected talk therapies of the 21st century.
CBT is defined as an active, directive, time-limited, structured approach that is used to treat a variety of mental problems like anxiety, phobias, depression, stress, and even pain. It is a client-driven therapy where you choose your own goals.
CBT focuses on the here and now much like MBCT.
In the academic community, there are also many good mindfulness researchers to be aware of including Judson Brewer, MD, Ph.D., David Creswell, Ph.D., Larissa Duncan, Ph.D. and Elissa Epel, Ph.D.
Judson Brewer MD, Ph.D. – Psychiatrist and Chief, Division of Mindfulness
Judson Brewer is a psychiatrist and an associate professor at the Departments of Medicine and Psychiatry as well as a research director at the Center for Mindfulness, UMASS Medical School.
Brewer is known for his work with mindfulness and addictions. In his work with neuroimaging technologies, he is developing mindfulness techniques that help people stop smoking, overcome food cravings as well as examining how mindfulness affects the brain.
Brewer is also looking into the future and researching the effects of mindfulness delivered digitally.
According to Brewer, this is the future of mindfulness and it’s important to study it. Brewer’s team is also developing an app, “Unwinding Anxiety,” which they plan to study in future clinical trials.
David Creswell, Ph.D. – Associate professor of psychology, Carnegie Mellon University
David Creswell, an associate professor of psychology, is researching stress and resiliency. His work is examining what really makes people resilient when they come upon stressful situations in life. His work combines health psychology and neuroscience.
Creswell has also begun clinical trials examining how Mindfulness-Based Stress Reduction may help improve social relationships as well as promote healthy aging for older adults.
Larissa Duncan, Ph.D.
Larissa Duncan is currently the Elizabeth C. Davies Chair in Child & Family Well-Being. She is also an associate professor of human development and family studies at the School of Human Ecology and the Center for Healthy Minds at the University of Wisconsin–Madison.
Duncan is currently working on finding ways to explore mindful parenting and helping to bring mindfulness training to pregnant women, as well as children, adolescents, and family members.
Duncan is looking toward the future and studying how Mindfulness-Based Childbirth and Parenting might affect a mothers’ mental health, stress physiology, and well-being.
As part of this research, she is also examining infants’ behavioral and neurological development.
Elissa Epel, Ph.D.
Elissa Epel is a Professor at the Department of Psychiatry at the University of California, San Francisco School of Medicine.
Epel is known for her work which links severe stress with shortened telomeres, which are cellular structures that play a key role in both disease and aging. Epel’s mindfulness research has also focused on examining the benefits of meditation as a tool for people who are under severe stress or experiencing ongoing stress.
Epel’s work is focused on helping those who have no previous meditation experience.
For the future, Epel is looking at how a practice like meditation might affect people who have suffered adversity in childhood. According to Epel, these types of individuals tend to have certain patterns of thought that are ideal targets for meditation training.
7 Studies You Need to Know About
Lutz, Dunne & Davidson (2008) examined how mindfulness impacts the amygdala, which is a region of the brain that is primarily associated with emotional processes.
In the study, it was determined that this area of the brain tended to be less active and have less gray matter density following mindfulness sessions.
The hippocampus also plays a role in mindfulness. The hippocampus, the region of the brain associated with memory, helps regulate the amygdala. Following mindfulness training, this part of the brain was also found to be more active according to Goldin & Gross (2010).
Mindfulness can help us nurture healthier relationships as well, according to a study done at the University of North Carolina at Chapel Hill (Carson, J. et al. (2004).
The study demonstrated a correlation between the practice of mindfulness and improved relationships. The couples in the study reported more closeness and more relationship satisfaction amongst other things.
Other studies examined the prefrontal cortex, the part of the brain associated with both impulse control and maturity. This part of the brain tended to become more active following mindfulness training. (Chiesa & Serretti, 2010).
In a study published in NeuroReport in 2005, results showed thicker cortical regions related to attention and sensory processing in long-term meditation practitioners, when compared with those who did not meditate.
These findings also suggest that simple meditation practice may offset cortical thinning brought about by aging. (Lazar et al. 2005)
A study of the 8-week MBSR course for nurses showed that their mindfulness practice facilitated empathetic attitudes while decreasing their tendency to take on other people’s negative emotions. (Beddoe & Murphy, 2004)
9 Benefits Research has Shown
Results of research indicate that mindfulness can help you in more ways than you think, especially in the workplace.
Christopher Liddy, an organizational behavior doctoral candidate at Case Western Reserve’s Weatherhead School of Management conducted research with Darren Good, an assistant professor at Pepperdine University.
The research examined over 4,000 scientific papers on varying degrees of mindfulness. The researchers looked at the impact of mindfulness in terms of how people think, feel and perform at work as well as how they relate.
The results of the study, Contemplating Mindfulness at Work, were then published in the Journal of Management.
The study suggests that:
- Mindfulness positively impacts human functioning.
- Mindfulness can help improve the quality of attention.
- Mindfulness, even though it is an internal quality, can impact interpersonal behavior.
- Mindfulness can help provide greater empathy and compassion.
In the research it was discovered that mindfulness cannot only positively impact attention, it can also help improve cognition, emotions, physiology and even behavior.
The researchers also found that mindfulness can help keep attention stable and help one remain focused on the present. Those who completed mindfulness training were better able to remain vigilant and focused, especially on visual and listening tasks.
Mindfulness has also been shown to help improve 3 unique qualities of attention, stability, control, and efficacy.
In terms of relationships, mindfulness can also give us a boost, helping to provide us with greater empathy and compassion.
According to Sara Davin, PsyD, MPH, mindfulness is not only a powerful tool for patients but also for doctors and medical care providers.
According to the Cleveland Clinic, there is ample evidence in support of the many benefits of mindfulness.
Some of these benefits include:
- Optimization of mental health.
- Positive impact on the brain and immune system.
- Help with chronic pain.
- Help overcome insomnia.
- Help with caregiver burnout healthcare providers may face.
In a review of more than 20 randomized controlled trials in 2011, it was shown that mindfulness can help improve overall mental health.
Mindfulness can also help reduce the risk of relapse from depression, while also helping with anxiety disorders like PTSD.
Mindfulness not only helps boost the immune system, but it can also help improve our neural processing in as little as a 10 to 15-minute session.
Mindfulness can also help with chronic pain. With chronic pain being an epidemic, it’s important to find alternative tools that are drug-free.
Mindfulness is one of those tools. In the study, those who meditated showed a decrease in pain and pain-related limitations. The benefits were comparable with cognitive behavioral therapy.
Insomnia and poor sleeping patterns can also lead to many other health problems. In randomized controlled trials, it was shown that mindfulness could help reduce insomnia, according to the Insomnia Severity Index.
Mindfulness can also be very beneficial to healthcare providers as well. Burnout is a big problem in the healthcare industry, and trials indicate that mindfulness can help boost resilience and create positive changes while reducing stress, anxiety, and burnout amongst healthcare workers.
The Neuroscience of Mindfulness: A Look Inside

Neuroplasticity allows the brain to reorganize itself. It does this by forming new neural connections throughout our life.
Evidence shows us that mindfulness can help increase our resilience, which allows us to cope better and roll with the punches.
By applying neuroplasticity, you can essentially “re-wire” and “hardwire” the brain helping you achieve greater levels of peace, health, happiness, and joy.
Sara Lazar, a neuroscientist at Harvard Medical School, actually uses MRI technology to look at the brain. In her research, she looks at the detailed structures of the brain to see what might be going on during certain tasks like meditation or yoga.
Lazar herself used to be a skeptic until she attended some yoga classes.
After attending a few classes, she literally felt the difference. She felt calmer, happier, and much more compassionate. As a result of this experience, she decided to refocus her research on the particular changes that occur in the brain’s physical structure as a result of meditation practice.
In Lazar’s first study she looked at individuals with extensive meditation experience. The study involved focused attention on those internal experiences.
The data showed that meditation might serve to slow down or even prevent age-related thinning of the frontal cortex. This area of the brain otherwise contributes to the formation of memories.
We assume that we become forgetful as we age. However, Lazar and her team discovered that those who meditated in their 40’s and 50’s had the same amount of grey matter as those in their 20’s and 30’s.
In Lazar’s second study, she used people who had never meditated before. These people attended a Mindfulness-based stress reduction training program, where they took a weekly class.
They also participated in various mindfulness exercises, including sitting meditation, mindful yoga and a body scan practice. Sessions lasted for 30 -40 minutes every day.
In this study, Lazar tested the recipients for the positive effects that mindfulness meditation would have on psychological well-being.
Lazar was also interested in helping people alleviate symptoms of chronic pain, insomnia, depression, and anxiety, amongst other things.
After 8 weeks, brain volume had increased in 4 regions of the brain. The most relevant of these regions included:
- The Hippocampus
- The Temporoparietal junction
Areas of the brain that decreased from the study included the amygdala.
The hippocampus is a structure of the brain shaped like a seahorse. It is responsible for the regulation of emotions, spatial orientation, learning and the storage of memories.
The temporoparietal junction is the area of the brain where the parietal lobes meet the temporal area. This area of the brain is responsible for empathy and compassion.
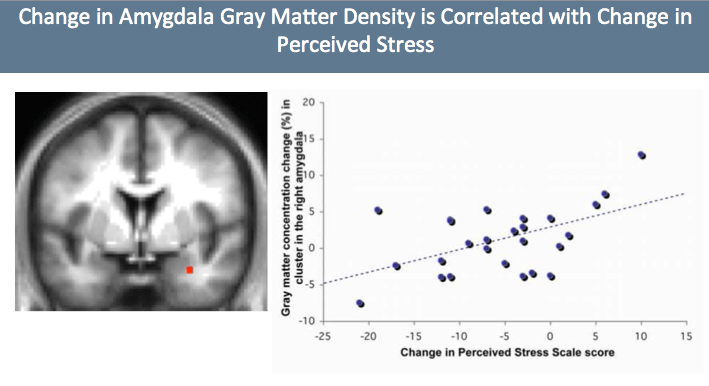
The study results also showed that the amygdala decreased, which meant the fight-or-flight response, the reaction to threats, also decreased.
The smaller the amygdala becomes, the better people react to stress. The decrease in the brain’s grey matter correlates with the changes in the levels of stress as well, according to the study.
All of this research is promising because it means that the change in people’s reactions occurs within themselves, and not in the environment itself.
In the end, mindfulness can help you change how you react to stressful situations, helping you feel calmer and much more in control.
How Mindfulness Affects and Changes The Brain
Over the past 10 years, studies in neuroimaging have investigated certain changes in brain morphology as it pertains to mindfulness meditation.
One meta-analysis taken from 21 neuroimaging studies examined the brains of 300 experienced practitioners of meditation. The study revealed that 8 unique regions of the brain were consistently changed in those who were experienced in meditation.
These 8 regions of the brain included:
- Rostrolateral prefrontal cortex
- Sensory cortices
- Insular cortex
- Hippocampus
- Anterior cingulate cortex
- Mid-cingulate cortex
- Superior longitudinal fasciculus
- Corpus callosum
The exact ways in which these different brain regions changed did vary from study to study since different studies use different neuroimaging measurements. However, consistent changes were seen across the board including:
- Changes in brain density
- Changes in thickness of brain tissue
- An increase in the number of neurons, fibers, and glia in a given region
- Changes in cortical surface area
- Changes in white matter fiber density
In looking at this research, we can certainly see a positive trend, with those who meditate and practice mindfulness.
What do all of these unique regions of the brain really do?
The rostrolateral prefrontal cortex is a region of the brain that is linked with a greater awareness of the thinking process (meta-awareness), the processing of complex, abstract information and introspection.
The sensory cortices and insular cortex are the parts of the brain that are the main cortical hubs when it comes to tactile information, like touch, pain, body awareness, and conscious proprioception.
The hippocampus is a pair of subcortical structures that are involved with the formation of memory as well as facilitating emotional responses.
The anterior cingulate cortex and mid-cingulate cortex are those areas in the brain connected with self-control, the regulation of emotions, as well as attention.
The superior longitudinal fasciculus and corpus callosum are what is called white matter tracts. These areas communicate between and within the hemispheres of the brain.
Researchers suggest that the effect of meditation on these brain structures appears to be medium in magnitude. This outcome is comparable to the effects of other interventions such as psychological interventions, education, and behavioral interventions.
Because this study involved so many different regions of the brain, researchers suggest that the effects of meditation might involve multiple aspects of brain functioning on a large scale, which is very promising.
As a result of this work, Tang, Holzel, and Posner suggest that engaging in mindfulness practice is indeed promising in terms of the treatment of clinical disorders, helping to encourage a healthy mind and enhanced well-being.
Research with mindfulness and meditation is really still in its infancy. Even with that, a number of studies have investigated changes in brain activation both at rest and during very specific tasks that are associated with the practice of mindfulness meditation.
Mindfulness Versus Medication: What Can We Prove?

In one recent trial, Mindfulness-based cognitive therapy (MBCT) was compared with anti-depressant medication.
The results of the study showed that with participants who had an unstable remission that 73% of them had a reduction in the risk of relapse in both the MBCT and the antidepressant group compared with a placebo.
There were no differences between the MBCT group and the depressant group. These results are encouraging because it suggests that MBCT is a reasonable alternative therapy to standard medication.
Those who used MBCT worked to develop capacities and coping strategies so they could then view their thoughts differently, seeing them in a bigger, wider way.
As a result, they developed more self-compassion, which helps to mediate the efficacy of MBCT.
Mathew Brensilver, Ph.D., also has an opinion on the effectiveness of mindfulness versus psychiatric medication like antidepressants.
According to Brensilver’s research, antidepressant use has expanded significantly over the years.
In 2000, only 6.5% of the population used antidepressants. Compare that to 2010, and you’ll see that the number has increased to 10.4%.
Both medication and meditation and mindfulness have similar goals – to reduce the amount of distress.
There are different schools of thought when comparing these two interventions. For some, going on antidepressants allows them to feel much more stabilized, which then allows them to focus better on a practice like mindfulness.
It has also been shown that combining medication and psychotherapy often results in better outcomes than one of those alone.
The same thing might be said for combining mindfulness and meditation with antidepressants, resulting in a better outcome.
According to Brensilver, psychiatric medication is not generally designed to help someone thrive and flourish.
Brensilver suggests that mindfulness offers something “distinctive and precious.”
Mindfulness, in his opinion, cannot only help alleviate distress, but it can also lead one into a state of mind where they are flourishing, which can help them develop deep completeness of the moment.
How mindfulness changes the emotional life of our brains
The Research On Autism and Mindfulness
The use of mindfulness interventions for those with autism is a fairly new thing. Research has shown that mindfulness is a beneficial practice that can lead to less parenting stress, less anxiety, lower levels of depression and improvements in sleep and life-satisfaction. (Conner & White 2014)
There has been some research done with something called Mindful Parenting that proves to be hopeful.
Mindful parenting involves applying the skills of mindfulness into the child-parent interaction. This includes listening with full attention, having a non-judgmental acceptance of the self and the child as well as self-regulation in the parenting relationship.
One reason mindfulness may be effective for those with autism has to do with the part of the brain known as the amygdala.
From the perspective of the brain the stress response invokes two unique systems:
- A “hot” system, which is largely automatic involving sensory and emotional processing (the amygdala).
- And a “cold” system that involves cognitive processing (the prefrontal cortex and anterior cingulate cortex).
During acute or chronic stress, the hot system tends to be overly responsive when compared to the cold system. To lower levels of stress, it’s important to find a balance between these systems.
This can be done by increasing cognitive control and regulation and lowering sensory and emotional processing.
Mindfulness meditation appears to help some people strike that precious balance. Focusing on and observing what one is sensing and feeling, in terms of the hot system, allows them to respond in a much calmer manner.
According to Singh et al. (2011), mindfulness may also help those with Asperger syndrome, which is a form of Autism.
Evolving research has found that the behavioral manifestations of Asperger syndrome can differ significantly between different people, and particularly between men and women (Simone, 2010). Likewise, the challenges those with the condition face will differ, so interventions and support must be tailored to an individual’s needs.
Studies have found that mindfulness-based interventions can help minimize several struggles that those with Asperger syndrome may experience related to behaviors and mood regulation.
Often, those with Asperger syndrome exhibit differences in the way they regulate emotions compared to neuro-typical populations (Samson, Huber, & Gross, 2012), using strategies such as physical stimulation (i.e., stimming) and time spent engaging with preferred activities.
While aggressive behavior is not always a feature of the syndrome (and it is not known how the prevalence of aggression in Asperger populations compares to neuro-typical populations), it may manifest as one of many possible emotional responses to a challenging, stressful, or overwhelming environment.
Therefore, one study by Singh et al. (2011) employed a multiple baseline design across subjects in which three adolescents with Asperger syndrome utilized a mindfulness-based technique known as Meditation on the Soles of the Feet as a strategy for reducing aggression at home and in school.
Subjects were taught to shift the focus of their attention away from negative things that may have previously triggered aggressive behavior to something neutral, like the soles of their feet.
Prior to the mindfulness instruction, the adolescents displayed moderate rates of aggression.
During the mindfulness practice, the mean rate of aggression on a weekly basis decreased. The study lasted between 17-24 weeks. The aggression levels decreased from 2.7, 2.5 and 3.2 to 0.9, 1.1, and 0.9, respectively.
No aggressive instances were observed during the last three weeks of the mindfulness practice.
No episodes of physical aggression occurred during a 4-year follow up, which was even more promising, and suggested that mindfulness may help young adults with Asperger syndrome to regulate emotions in more productive ways.
Another study, pointing to the finding that 50-70% of adults on the autism spectrum experience anxiety or depression, employed an MBSR intervention involving thirteen 90-minute sessions (Sizoo & Kuiper, 2017). In the sessions, participants practiced various mindfulness techniques, including meditations and body scans, and explored strategies to embed mindfulness practice into their daily lives.
The study found that after the 13-week program (and at the 3-month follow-up), participants reported a more positive global mood and substantially reduced anxiety. These effects were found to be of similar magnitude to those stemming from a CBT intervention.
Therefore, research suggests that mindfulness may support those living with Asperger syndrome to effectively manage moods and employ healthier strategies for managing anger and frustration.
Can Mindfulness Help ADHD?

In one randomized controlled trial researchers compared the affectedness of mindfulness instruction to the effectiveness of methylphenidate amongst children with ADHD. The study is currently focused on measures of attention and hyperactivity as well as impulsivity.
While medication is typically the first sought after treatment for ADHD, its effects are often short-term. Medication also has side effects and the adherence is often low.
Training in mindfulness is emerging as a good choice for young people with ADHD.
The outcomes of the study will be presented at conferences and in scientific and peer-reviewed journals. The results will help not only families of those with ADHD but also general practitioners and mental health providers.
This study will also help inform health insurance companies as to which treatment is more cost-effective in the long term. Data collection for this study is ongoing, but it offers hope to those who are seeking alternative treatments for ADHD.
A Take-Home Message
The brain is made up of billions of neurons. These neurons need to communicate with one another and with other parts of the body. All of these systems work together in a cohesive fashion.
The brain is plastic, meaning it has plasticity, the ability to learn and grow and change over time. Meditation affects the brain’s functionality, its structure, and its thought patterns.
The more you meditate and practice mindfulness, the more the brain’s synapses strengthen, which can help improve your life.
Every time you indulge in those negative thoughts and feelings, you are strengthening their effect on you.
However, every time you engage in positive thoughts and behaviors and let go of the negative ones, you are retraining your brain to think a little differently.
As Aristotle once said:
“We are what we repeatedly do.”
We think what we repeatedly think as well. Thanks to the study of neuroscience, the scientific community has become much more aware of how the brain works.
Joining together neuroscience and mindfulness, you can begin to bridge the gap and connect all of the dots between how the brain really works and how those daily practices can impact your life.
By practicing mindfulness and meditation, you can then begin to more fully understand how your emotions, thoughts, and feelings impact your life.
If you want to to take one small step in support of a happier, healthier, and calmer way of life, mindfulness and meditation is a great place to start.
We hope you enjoyed reading this article. Don’t forget to download our three Mindfulness Exercises for free.
- Autism and the Neuroscience of Mindfulness. (n.d.). Retrieved March 12, 2019, from https://theautismblog.seattlechildrens.org/autism-and-the-neuroscience-of-mindfulness/
- Beddoe, A & Murphy, S. 2004. Does Mindfulness Decrease Stress and Foster Empathy Amoings Nursing Student? Journal of Nursing Education, 43(7), 305-312.
- Brensilver, M. (2016, August 03). Mindfulness and Psychiatric Medication. Retrieved March 12, 2019, from https://www.mindfulschools.org/research-and-neuroscience/mindfulness-psychiatric-medication/
- Bushak, L. (2016, March 10). What’s The Difference Between Mindfulness And Meditation? Retrieved March 12, 2019, from https://www.medicaldaily.com/mindfulness-meditation-differences-377346
- Carson, J. et al. (2004). Mindfulness-Based Relationship Enhancement. Behavior Therapy, 35, 471-494.
- Chiesa, A., & Serretti, A. (2010). A systematic review of neurobiological and clinical features of mindfulness meditations. Psychological Medicine, 40(08), 1239–1252.
- Cho, J. (2016, July 14). 6 Scientifically Proven Benefits Of Mindfulness And Meditation. Retrieved March 12, 2019, from https://www.forbes.com/sites/jeenacho/2016/07/14/10-scientifically-proven-benefits-of-mindfulness-and-meditation/#2d3a006063ce
- Conner, C. M., & White, S. W. (2014). Stress in mothers of children with autism: Trait mindfulness as a protective factor. Research in Autism Spectrum Disorders, 8(6), 617-624.
- Crane, R.S., Brewer, J. A., Feldman, C., Kabat-Zinn, J., Santorelli, S., Williams, J. M. G., Kuyken, W., (2017) “What Defines Mindfulness-Based Programs? The Warp and the Weft.” Psychol Medicine 47: 990-999.
- D. J. Good, C. J. Lyddy, T. M. Glomb, J. E. Bono, K. W. Brown, M. K. Duffy, R. A. Baer, J. A. Brewer, S. W. Lazar. Contemplating Mindfulness at Work: An Integrative Review. Journal of Management, 2015; 42 (1): 114-142.
- Fox, K. C., Nijeboer, S., Dixon, M. L., Floman, J. L., Ellamil, M., Rumak, S. P., . . . Christoff, K. (2014, June). Is meditation associated with altered brain structure? A systematic review and meta-analysis of morphometric neuroimaging in meditation practitioners. Retrieved March 12, 2019, from https://www.ncbi.nlm.nih.gov/pubmed/24705269
- Goldin, P. R., & Gross, J. J. (2010). Effects of mindfulness-based stress reduction (MBSR) on emotion regulation in social anxiety disorder. Emotion, 10(1), 83.
- Hoge, E. A., Bui, E., Marques, L., Metcalf, C. A., Morris, L. K., Robinaugh, D. J., . . . Simon, N. M. (2013, August). Randomized controlled trial of mindfulness meditation for generalized anxiety disorder: Effects on anxiety and stress reactivity. Retrieved March 12, 2019, from https://www.ncbi.nlm.nih.gov/pubmed/23541163
- Hölzel, B. K., Carmody, J., Evans, K. C., Hoge, E. A., Dusek, J. A., Morgan, L., … Lazar, S. W. (2010). Stress reduction correlates with structural changes in the amygdala. Social Cognitive and Affective Neuroscience, 5(1), 11–17.
- Hölzel, B. K., Carmody, J., Vangel, M., Congleton, C., Yerramsetti, S. M., Gard, T., & Lazar, S. W. (2011). Mindfulness practice leads to increases in regional brain gray matter density. Psychiatry Research: Neuroimaging, 191(1), 36–43.
- Lazar, S. et al. (20 NeuroReport, 16(17), 1893-1897.05). Meditation experience is associated with increased cortical thickness.
- Lazar, S. (n.d.). Welcome to the Lazar Lab. Retrieved from https://scholar.harvard.edu/sara_lazar
- Lu, S. (2015, March). Mindfulness holds promise for treating depression. Retrieved March 12, 2019, from https://www.apa.org/monitor/2015/03/cover-mindfulness
- Luke, A., & Gibson, B. (2014, November 24). Mindfulness Meditation Reduces Implicit Age and Race Bias: The Role of Reduced Automaticity of Responding. Retrieved March 12, 2019, from https://journals.sagepub.com/doi/abs/10.1177/1948550614559651
- Lutz, A., Slagter, H. A., Dunne, J. D., & Davidson, R. J. (2008). Attention regulation and monitoring in meditation. Trends in Cognitive Sciences, 12(4), 163–169.
- McGreevey, & McGreevey, S. (2011, April 22). ‘Turn down the volume’. Retrieved March 12, 2019, from https://news.harvard.edu/gazette/story/2011/04/turn-down-the-volume/
- Meppelink, R., de Bruin, E. I., & Bögels, S. M. (2016). Meditation or Medication? Mindfulness training versus medication in the treatment of childhood ADHD: a randomized controlled trial. BMC Psychiatry, 16, 267.
- Neuroplasticity: The Neuroscience of Mindfulness Meditation. (n.d.). Retrieved March 12, 2019, from https://www.nyimc.org/event/the-neuroscience-of-mindfulness-and-meditation/
- Research on Mindfulness in Education. (n.d.). Retrieved March 12, 2019, from https://www.mindfulschools.org/about-mindfulness/research/
- Samson, A. C., Huber, O., & Gross, J. J. (2012). Emotion regulation in Asperger’s syndrome and high-functioning autism. Emotion, 12(4), 659-665.
- Simone, R. (2010). Aspergirls: Empowering females with Asperger syndrome. London, UK: Jessica Kingsley Publishers.
- Singh, N. N., Lancioni, G. E., Manikam, R., Winton, A. S. W., Singh, A. N. A., Singh, J., & Singh, A. D. A. (2011). A mindfulness-based strategy for self-management of aggressive behavior in adolescents with autism. Research in Autism Spectrum Disorders, 5(3), 1153–1158.
- Singh, N., Lancioni, G., Singh, A., Winton, A., & Singh, A. (2011, July). Adolescents with Asperger syndrome can use a mindfulness-based strategy to control their aggressive behavior. Retrieved March 12, 2019, from https://www.sciencedirect.com/science/article/pii/S1750946710001984
- Sizoo, B. B., & Kuiper, E. (2017). Cognitive behavioural therapy and mindfulness based stress reduction may be equally effective in reducing anxiety and depression in adults with autism spectrum disorders. Research in Developmental Disabilities, 64, 47-55.
- The Neuroscience of Mindfulness Meditation. (2017, February 24). Retrieved March 12, 2019, from https://chopra.com/articles/the-neuroscience-of-mindfulness-meditation
- Zapletal, K. (2017, June 26). Neuroscience of Mindfulness: What Happens to Your Brain When You Meditate. Retrieved March 12, 2019, from https://observer.com/2017/06/neuroscience-mindfulness-brain-when-you-meditate-development/
- Zapletal, K., & Zapletal, K. (2017, May 18). Neuroscience of Mindfulness: What Exactly Happens to Your Brain When You Meditate. Retrieved March 12, 2019, from https://mindfulentrepreneurship.com/neuroscience-of-mindfulness-what-exactly-happens-to-your-brain-when-you-meditate-7d1ca47d9fca
- http://www.jneuropsychiatry.org/peer-review/is-it-medication-versus-mindfulness-in-prevention-of-depression-relapse-neuropsychiatry.pdf
Let us know your thoughts
Read other articles by their category
- Body & Brain (49)
- Coaching & Application (57)
- Compassion (26)
- Counseling (51)
- Emotional Intelligence (24)
- Gratitude (18)
- Grief & Bereavement (21)
- Happiness & SWB (40)
- Meaning & Values (26)
- Meditation (20)
- Mindfulness (45)
- Motivation & Goals (45)
- Optimism & Mindset (34)
- Positive CBT (29)
- Positive Communication (20)
- Positive Education (47)
- Positive Emotions (32)
- Positive Leadership (18)
- Positive Parenting (4)
- Positive Psychology (33)
- Positive Workplace (37)
- Productivity (17)
- Relationships (46)
- Resilience & Coping (36)
- Self Awareness (21)
- Self Esteem (38)
- Strengths & Virtues (32)
- Stress & Burnout Prevention (34)
- Theory & Books (46)
- Therapy Exercises (37)
- Types of Therapy (64)





What our readers think
Thank you for sharing the best information this blog is more helpful for me.
What meditation research neglects, the affective neuroscience of proprioception and mindfulness, and implications regarding the self-mastery of positive affective states.
For affective and cognitive neuroscience, brain imaging (fmri) and ‘in vivo’ or direct stimulation of cellular arrays in the brain are the primary methods to understand how affect in instantiated in the brain, yet cannot account for how neuro-muscular or proprioceptive stimuli modulate affect. This has resulted in the general neglect of how these stimuli elicit and inhibit affective states. Below is a brief explanation and simple procedure that demonstrates the role of tension and relaxation in eliciting affect, and provides a much simpler and testable explanation of ‘unique’ affective states such as meditation, peak experience, and ‘flow’.
Proprioceptors (sensory receptors) are located in our muscles and joints and respond to changes in the relative activity of the covert musculature. They also induce changes in affective states in the brain. An example of this is how we experience pleasure. Unlike other functions in the brain, from perception to thinking, the neural source of our pleasures are localized in the brain as specialized groups of nerve cells or ‘nuclei’, or ‘hot spots’, located in the midbrain. These nuclei receive inputs from different sources in the nervous system, from proprioceptive stimuli (neuro-muscular activity) to interoceptive stimuli (satiation and deprivation) to cognitive stimuli (novel positive or negative means-end expectancies), and all modulate the activity of these nuclei which release or inhibit endogenous opioids that elicit the rainbow of pleasures which mark our day.
Just get relaxed using a relaxation protocol such as progressive muscle relaxation, eyes closed rest, or mindfulness, and then follow it by exclusively attending to or performing meaningful activity, or in other words, positive thinking, and avoiding all meaningless activity or ‘distraction’. Keep it up and you will not only stay relaxed, but continue so with a greater sense of wellbeing or pleasure. The attribution of affective value to meaningful behavior makes the latter seem ‘autotelic’, or reinforcing in itself and thus increasing self-control, and the resultant persistent attention to meaning crowds out the occasions we might have spent dwelling on other unmeaningful worries and concerns.
Hi Art,
Thank you for your thoughts here. We’re pleased that our post inspired such an in-depth response. Unfortunately, in the interest of keeping our comment section easy for our readers to navigate, we could not publish your full comment. But thank you, and we welcome more succinct contributions in the future.
– Nicole | Community Manager
I felt a little upset when I read the comments about young people with Aspergers. It seems to me that it was a little too generalised. Many teenagers with Aspergers don’t display any aggression whatsoever. I have a teenager with Aspergers and work with teenagers with Aspergers and very few display aggression. This for me re-inforced the stereotypes people have of Aspergers. Mindfulness is particularly helpful to help deal with anxiety. That would be absolutely true. I was disappointed to read this on PositivePsychology!
Hi Karen,
Thank you for your feedback. I agree with your thoughts here; not all who live with Aspergers experience difficulties with aggression, but the snapshot of research findings we present comes across as a generalization. I’ll pass this feedback on to our editing team.
– Nicole | Community Manager
Thanks Nicole, I really appreciate this. My son who is going to uni next year and lives with Aspergers gets quite upset when it comes across like this. He says thank you for responding too.
I believe that Mindfulness is something that can help people on many different levels. I do not believe that people who have been diagnosed with mental disorders should be treated as if they are all in a box. In order to breakthrough on mental awareness we must first acknowledge the symptoms and then understand how to treat them. First and foremost I believe that God designed us to be mindful. Some may be wired differently than others. If we take a step back and try to define what is normal we would see their is no such thing. Our differences is who makes us who we are. If we approach mental health with the mind frame of meeting the need of the person instead of labeling I believe we would have a better understanding of how to treat the problem. Being able to focus is usually one of the main problems. I am determined to change the way this is perceived and teach new ways of being able to reach everyone from the level they are on with mindfulness the way God intended. YOUR FULL MIND LIFE LLC, TONIKIA L. STEANS CREATOR
Dear Sir/Madam,
Good morning! I am a volunteering meditation practitioner live in the Uk. I am planning to write a book to publish on mindfulness and would like to know whether I am allowed to use your website materials if I quote them as reference for my book.
Kind Regards
Dr Kamal
Hi Kamal,
Of course — feel free to reference us in your book. Best of luck with it!
– Nicole | Community Manager
A wonderful article summarizing the CRITICAL DEVELOPMENTS, in this domain. A lot still needs to be explored. But, the BEST part is ” We are Progressing “.
I am a Science Teacher and something I know about the brain is that language comes from both hemispheres (which you may already be implying). The left side is more about rules, regulations, standards and handles analyzing situations when speaking of language. The right is responsible fore descriptive and creative language. Are you a leftie? The right hemisphere controls the left hand is less dominant than the left hemisphere. The corpus collosum connects the two. I bet strenghthening the neurons in the corpus collosum would help. I once did meditation that did just that. I will see if I can find it.
On Affective Neuroscience and Mindfulness: A different view on mindfulness
Presented here for your consideration is a new and quite radical explanation of mindfulness from the perspective of affective neuroscience, or more specifically, a neurologically grounded theory of incentive motivation. The explanation is simple, easily falsifiable, and its procedural entailment redefines the practice of mindfulness. Still, it may be wrong. Indeed, a bad theory must not overstay its welcome, and although I provide a granular explanation of my hypothesis in the treatise linked below, sometimes to see the light one must look at the sun.
In 1984, the psychologist David Holmes published in the ‘American Psychologist’ a review (linked below) of the cumulative research on meditation and concluded that meditative states were merely resting. The article was roundly criticized, as meditation was obviously much more than a simple state of rest. Well, the critics were half right, meditation is rest, but rest is NOT simple. Indeed, rest induces a pleasurable or affective state which can be modulated in turn by the moment to moment expectancies that not only tell you where you are, but where you are going. Indeed, contrary to what mindfulness suggests, being in the moment is impossible, for we must always decide upon the direction or meaning of our actions from moment to moment, and this always translates into effective and affective outcomes. These concepts can easily be anchored to the facts of behavior and translated into simple validating procedure, as I argue below.
In affective neuroscience, incentives embody affective states that reflect attentive arousal as mediated by dopamine systems, and pleasure, as mediated by opioid systems. The nerve cells or nuclei of both systems are proximally located in the mid-brain and can activate each other. For example, looking forward to a pleasure accentuates the pleasure, and a pleasurable experience perks up attentive arousal.
Dopamine release can occur as a phasic or intermittent response, as when our attention ebbs and flows as a function or our momentary fluctuating interest and boredom. It also occurs as a tonic or sustained response in order to maintain a baseline level of alertness that allows us to go about our lives. Similarly, opioid release occurs as a phasic response when we sample our daily pleasures, and it also may be a tonic response, but only when the covert musculature is in an inactive or relaxed state. When an individual is tense or anxious, tonic opioid activity is suppressed. This makes evolutionary sense, as resting conserves an animal’s caloric resources, and animals in the wild sustain their survivability through the dual incentive of alertness for predators while at a pleasurable state of rest. (as your lounging cat would attest, if it could speak)
From these facts, certain predictions about behavior may be made that conform with empiric reality. For example, peak or flow experiences that reflect heightened attentive arousal and pleasure only occur when an individual is both relaxed and is aroused by behavior that entails highly positive moment to moment meaningful outcomes (e.g. creativity, sporting events). Dopamine in turn stimulates opioid activity, and the enhanced dopamine/opioid interaction results in an ecstatic or peak experience.
This observation can also be practically confirmed (or falsified!). Simply elicit a continuous resting state through a mindfulness procedure and couple it with imminent behavior that has important or meaningful outcomes, and the more meaningful, the greater the affect. The underscores the fact that as a resting protocol, mindfulness will elicit affective states which will scale with the salience of momentary outcomes that in turn can be easily arranged. Mindfulness in other words is not a steady affective state, but a variable affective state, and can be a mystical or peak experience, or just a mildly pleasant way of chilling out. It all depends upon what you are looking forward to imminently do.
For a more detailed explanation see pp.47-52, 82-86 on the linked treatise on the psychology of resting states.
Holmes Article
https://www.scribd.com/document/291558160/Holmes-Meditation-and-Rest-The-American-Psychologist
The Psychology of Rest
https://docs.wixstatic.com/ugd/9bba72_a06875c1cef541c5a7e55bac9ef86711.pdf
Good article
Hello
I am from Norway (66 years old), and I have been stuttering since I was 6 years old. I have now read “The master and his emmissary”, written by Iain McGilchrist. It is a book about functions of right and left hemishpere. I feel my stuttering could have some connection with those two brain halves. I feel there is a battle between left and right when I am stuttering. Concentrating in a meditative way when speaking reduces the stuttering. Do you have any comments?
Compliments from
Tor Sørdal Bue