CBT Techniques: 25 Cognitive Behavioral Therapy Worksheets
 Even if you’re relatively unfamiliar with psychology, chances are you’ve heard of cognitive-behavioral therapy, commonly known as CBT.
Even if you’re relatively unfamiliar with psychology, chances are you’ve heard of cognitive-behavioral therapy, commonly known as CBT.
It’s an extremely common type of talk therapy practiced around the world.
If you’ve ever interacted with a mental health therapist, a counselor, or a psychiatry clinician in a professional setting, it’s likely you’ve participated in CBT.
If you’ve ever heard friends or loved ones talk about how a mental health professional helped them identify unhelpful thoughts and patterns and behavior and alter them to more effectively work towards their goals, you’ve heard about the impacts of CBT.
CBT is one of the most frequently used tools in the psychologist’s toolbox. Though it’s based on simple principles, it can have wildly positive outcomes when put into practice.
In this article, we’ll explore what CBT is, how it works, and how you can apply its principles to improve your own life or the lives of your clients.
Before you read on, we thought you might like to download our three Positive CBT Exercises for free. These science-based exercises will provide you with a comprehensive insight into Positive CBT and will give you the tools to apply it in your therapy or coaching.
This Article Contains:
- What is CBT?
- Cognitive Distortions
- 9 Essential CBT Techniques and Tools
- Cognitive Behavioral Therapy Worksheets (PDFs) To Print and Use
- Some More CBT Interventions and Exercises
- A CBT Manual and Workbook for Your Own Practice and for Your Client
- 5 Final Cognitive Behavioral Activities
- A Take-Home Message
- References
What is CBT?
“This simple idea is that our unique patterns of thinking, feeling, and behaving are significant factors in our experiences, both good and bad. Since these patterns have such a significant impact on our experiences, it follows that altering these patterns can change our experiences” (Martin, 2016).
Cognitive-behavioral therapy aims to change our thought patterns, our conscious and unconscious beliefs, our attitudes, and, ultimately, our behavior, in order to help us face difficulties and achieve our goals.
Psychiatrist Aaron Beck was the first to practice cognitive behavioral therapy. Like most mental health professionals at the time, Beck was a psychoanalysis practitioner.
While practicing psychoanalysis, Beck noticed the prevalence of internal dialogue in his clients and realized how strong the link between thoughts and feelings can be. He altered the therapy he practiced in order to help his clients identify, understand, and deal with the automatic, emotion-filled thoughts that regularly arose in his clients.
Beck found that a combination of cognitive therapy and behavioral techniques produced the best results for his clients. In describing and honing this new therapy, Beck laid the foundations of the most popular and influential form of therapy of the last 50 years.
This form of therapy is not designed for lifelong participation and aims to help clients meet their goals in the near future. Most CBT treatment regimens last from five to ten months, with clients participating in one 50- to 60-minute session per week.
CBT is a hands-on approach that requires both the therapist and the client to be invested in the process and willing to actively participate. The therapist and client work together as a team to identify the problems the client is facing, come up with strategies for addressing them, and creating positive solutions (Martin, 2016).
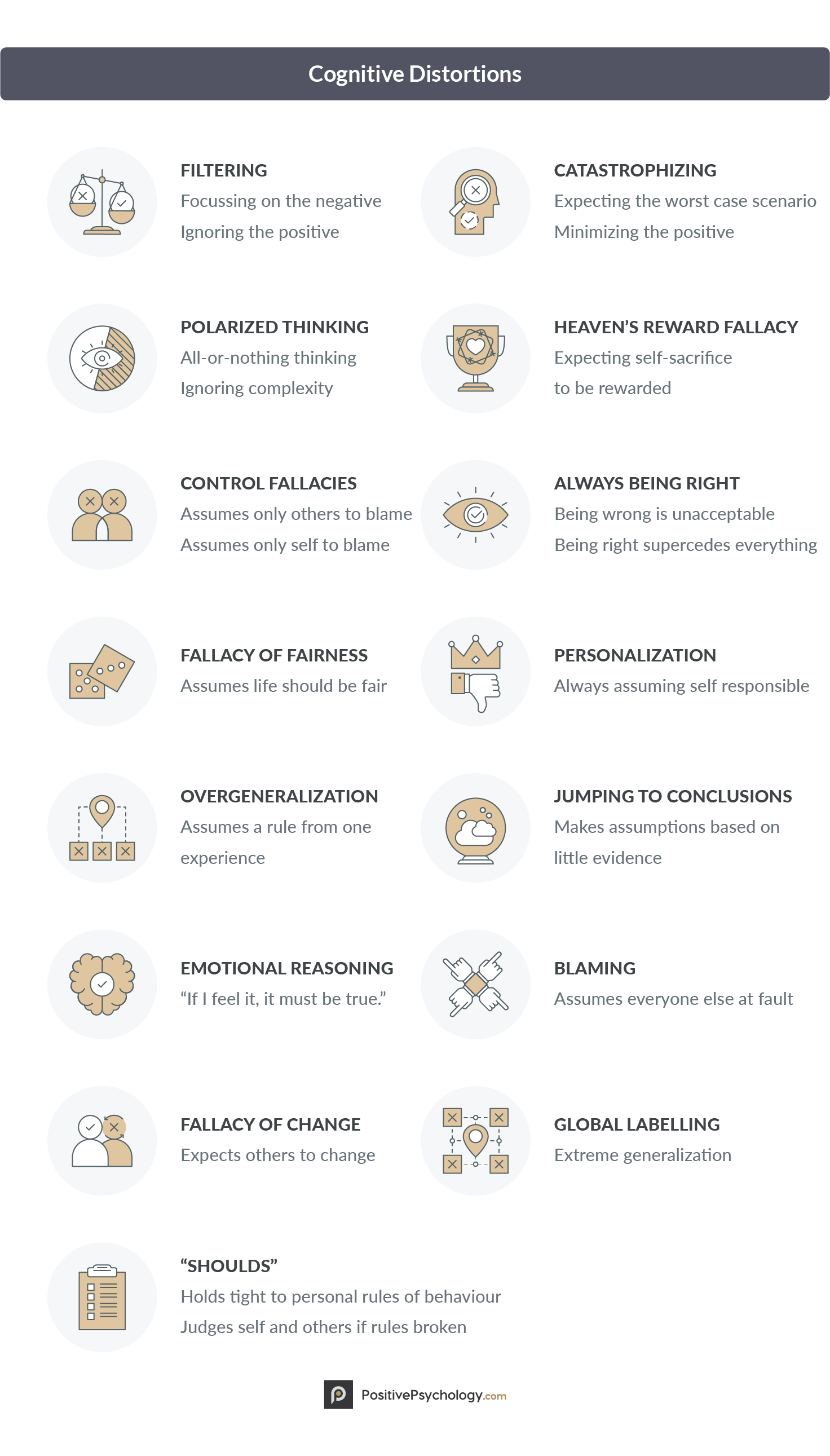
Cognitive Distortions
Many of the most popular and effective cognitive-behavioral therapy techniques are applied to what psychologists call “cognitive distortions,” inaccurate thoughts that reinforce negative thought patterns or emotions (Grohol, 2016).
There are 15 main cognitive distortions that can plague even the most balanced thinkers.
1. Filtering
Filtering refers to the way a person can ignore all of the positive and good things in life to focus solely on the negative. It’s the trap of dwelling on a single negative aspect of a situation, even when surrounded by an abundance of good things.
2. Polarized thinking / Black-and-white thinking
This cognitive distortion is all-or-nothing thinking, with no room for complexity or nuance—everything’s either black or white, never shades of gray.
If you don’t perform perfectly in some area, then you may see yourself as a total failure instead of simply recognizing that you may be unskilled in one area.
3. Overgeneralization
Overgeneralization is taking a single incident or point in time and using it as the sole piece of evidence for a broad conclusion.
For example, someone who overgeneralizes could bomb an important job interview and instead of brushing it off as one bad experience and trying again, they conclude that they are terrible at interviewing and will never get a job offer.
4. Jumping to conclusions
Similar to overgeneralization, this distortion involves faulty reasoning in how one makes conclusions. Unlike overgeneralizing one incident, jumping to conclusions refers to the tendency to be sure of something without any evidence at all.
For example, we might be convinced that someone dislikes us without having any real evidence, or we might believe that our fears will come true before we have a chance to really find out.
5. Catastrophizing / Magnifying or Minimizing
This distortion involves expecting that the worst will happen or has happened, based on an incident that is nowhere near as catastrophic as it is made out to be. For example, you may make a small mistake at work and be convinced that it will ruin the project you are working on, that your boss will be furious, and that you’ll lose your job.
Alternatively, one might minimize the importance of positive things, such as an accomplishment at work or a desirable personal characteristic.
6. Personalization
This is a distortion where an individual believes that everything they do has an impact on external events or other people, no matter how irrational that may be. A person with this distortion will feel that he or she has an exaggerated role in the bad things that happen around them.
For instance, a person may believe that arriving a few minutes late to a meeting led to it being derailed and that everything would have been fine if they were on time.
7. Control fallacies
This distortion involves feeling like everything that happens to you is either a result of purely external forces or entirely due to your own actions. Sometimes what happens to us is due to forces we can’t control, and sometimes what it’s due to our own actions, but the distortion is assuming that it is always one or the other.
We might assume that difficult coworkers are to blame for our own less-than-stellar work, or alternatively assume that every mistake another person makes is because of something we did.
8. Fallacy of fairness
We are often concerned about fairness, but this concern can be taken to extremes. As we all know, life is not always fair. The person who goes through life looking for fairness in all their experiences will end up resentful and unhappy.
Sometimes things will go our way, and sometimes they will not, regardless of how fair it may seem.
9. Blaming
When things don’t go our way, there are many ways we can explain or assign responsibility for the outcome. One method of assigning responsibility is blaming others for what goes wrong.
Sometimes we may blame others for making us feel or act a certain way, but this is a cognitive distortion. Only you are responsible for the way you feel or act.
10. “Shoulds”
“Shoulds” refer to the implicit or explicit rules we have about how we and others should behave. When others break our rules, we are upset. When we break our own rules, we feel guilty. For example, we may have an unofficial rule that customer service representatives should always be accommodating to the customer.
When we interact with a customer service representative that is not immediately accommodating, we might get angry. If we have an implicit rule that we are irresponsible if we spend money on unnecessary things, we may feel exceedingly guilty when we spend even a small amount of money on something we don’t need.
11. Emotional reasoning
This distortion involves thinking that if we feel a certain way, it must be true. For example, if we feel unattractive or uninteresting in the current moment, we think we are unattractive or uninteresting. This cognitive distortion boils down to:
“I feel it, therefore it must be true.”
Clearly, our emotions are not always indicative of the objective truth, but it can be difficult to look past how we feel.
12. Fallacy of change
The fallacy of change lies in expecting other people to change as it suits us. This ties into the feeling that our happiness depends on other people, and their unwillingness or inability to change, even if we demand it, keeps us from being happy.
This is a damaging way to think because no one is responsible for our own happiness except ourselves.
13. Global labeling / mislabeling
This cognitive distortion is an extreme form of generalizing, in which we generalize one or two instances or qualities into a global judgment. For example, if we fail at a specific task, we may conclude that we are a total failure in not only that area but all areas.
Alternatively, when a stranger says something a bit rude, we may conclude that he or she is an unfriendly person in general. Mislabeling is specific to using exaggerated and emotionally loaded language, such as saying a woman has abandoned her children when she leaves her children with a babysitter to enjoy a night out.
14. Always being right
While we all enjoy being right, this distortion makes us think we must be right, that being wrong is unacceptable.
We may believe that being right is more important than the feelings of others, being able to admit when we’ve made a mistake or being fair and objective.
15. Heaven’s Reward Fallacy
This distortion involves expecting that any sacrifice or self-denial will pay off. We may consider this karma, and expect that karma will always immediately reward us for our good deeds. This results in feelings of bitterness when we do not receive our reward (Grohol, 2016).
Many tools and techniques found in cognitive behavioral therapy are intended to address or reverse these cognitive distortions.
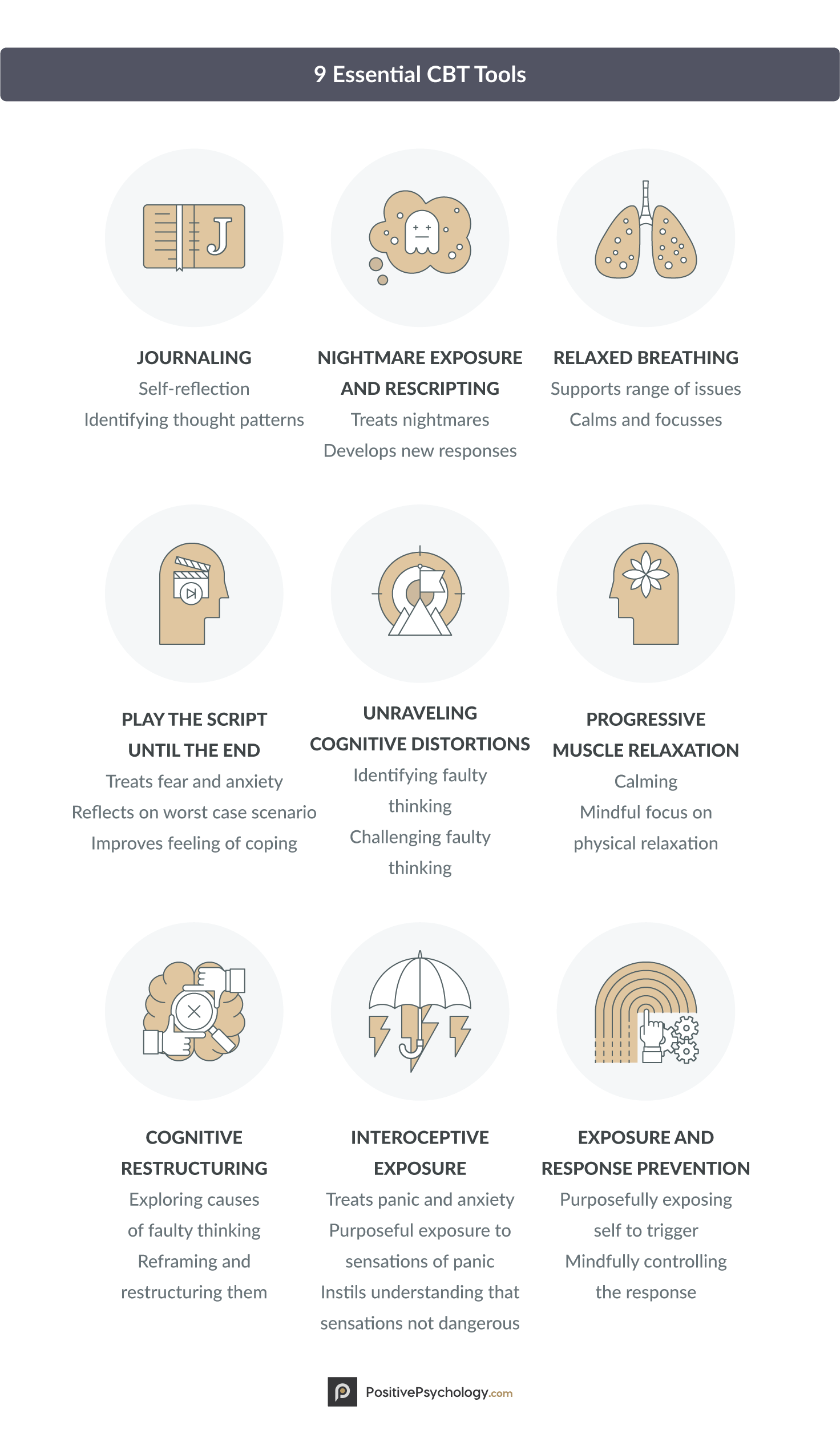
9 Essential CBT Techniques and Tools
There are many tools and techniques used in cognitive behavioral therapy, many of which can be used in both a therapy context and in everyday life. The nine techniques and tools listed below are some of the most common and effective CBT practices.
1. Journaling
This technique is a way to gather about one’s moods and thoughts. A CBT journal can include the time of the mood or thought, the source of it, the extent or intensity, and how we reacted, among other factors.
This technique can help us to identify our thought patterns and emotional tendencies, describe them, and change, adapt, or cope with them (Utley & Garza, 2011).
Follow the link to find out more about using a thought diary for journaling.
2. Unraveling cognitive distortions
This is a primary goal of CBT and can be practiced with or without the help of a therapist. In order to unravel cognitive distortions, you must first become aware of the distortions from which you commonly suffer (Hamamci, 2002).
Part of this involves identifying and challenging harmful automatic thoughts, which frequently fall into one of the 15 categories listed earlier.
3. Cognitive restructuring
Once you identify the distortions you hold, you can begin to explore how those distortions took root and why you came to believe them. When you discover a belief that is destructive or harmful, you can begin to challenge it (Larsson, Hooper, Osborne, Bennett, & McHugh, 2015).
For example, if you believe that you must have a high-paying job to be a respectable person, but you’re then laid off from your high-paying job, you will begin to feel bad about yourself.
Instead of accepting this faulty belief that leads you to think negative thoughts about yourself, with cognitive restructuring you could take an opportunity to think about what really makes a person “respectable,” a belief you may not have explicitly considered before.
4. Exposure and response prevention
This technique is specifically effective for those who suffer from obsessive-compulsive disorder (OCD; Abramowitz, 1996). You can practice this technique by exposing yourself to whatever it is that normally elicits a compulsive behavior, but doing your best to refrain from the behavior.
You can combine journaling with this technique, or use journaling to understand how this technique makes you feel.
5. Interoceptive exposure
Interoceptive Exposure is intended to treat panic and anxiety. It involves exposure to feared bodily sensations in order to elicit the response (Arntz, 2002). Doing so activates any unhelpful beliefs associated with the sensations, maintains the sensations without distraction or avoidance, and allows new learning about the sensations to take place.
It is intended to help the sufferer see that symptoms of panic are not dangerous, although they may be uncomfortable.
6. Nightmare exposure and rescripting
Nightmare exposure and rescripting are intended specifically for those suffering from nightmares. This technique is similar to interoceptive exposure, in that the nightmare is elicited, which brings up the relevant emotion (Pruiksma, Cranston, Rhudy, Micol, & Davis, 2018).
Once the emotion has arisen, the client and therapist work together to identify the desired emotion and develop a new image to accompany the desired emotion.
7. Play the script until the end
This technique is especially useful for those suffering from fear and anxiety. In this technique, the individual who is vulnerable to crippling fear or anxiety conducts a sort of thought experiment in which they imagine the outcome of the worst-case scenario.
Letting this scenario play out can help the individual to recognize that even if everything he or she fears comes to pass, the outcome will still be manageable (Chankapa, 2018).
8. Progressive muscle relaxation
This is a familiar technique to those who practice mindfulness. Similar to the body scan, progressive muscle relaxation instructs you to relax one muscle group at a time until your whole body is in a state of relaxation (McCallie, Blum, & Hood, 2006).
You can use audio guidance, a YouTube video, or simply your own mind to practice this technique, and it can be especially helpful for calming nerves and soothing a busy and unfocused mind.
9. Relaxed breathing
This is another technique that will be familiar to practitioners of mindfulness. There are many ways to relax and bring regularity to your breath, including guided and unguided imagery, audio recordings, YouTube videos, and scripts. Bringing regularity and calm to your breath will allow you to approach your problems from a place of balance, facilitating more effective and rational decisions (Megan, 2016).
These techniques can help those suffering from a range of mental illnesses and afflictions, including anxiety, depression, OCD, and panic disorder, and they can be practiced with or without the guidance of a therapist. To try some of these techniques without the help of a therapist, see the next section for worksheets and handouts to assist with your practice.
How does cognitive behavioral therapy work – Psych Hub
Cognitive-Behavioral Therapy Worksheets (PDFs) To Print and Use

1. Coping styles worksheet
This PDF Coping Styles Formulation Worksheet instructs you or your client to first list any current perceived problems or difficulties – “The Problem”. You or your client will work backward to list risk factors above (i.e., why you are more likely to experience these problems than someone else) and triggers or events (i.e., the stimulus or source of these problems).
Once you have defined the problems and understand why you are struggling with them, you then list coping strategies. These are not solutions to your problems, but ways to deal with the effects of those problems that can have a temporary impact. Next, you list the effectiveness of the coping strategies, such as how they make you feel in the short- and long-term, and the advantages and disadvantages of each strategy.
Finally, you move on to listing alternative actions. If your coping strategies are not totally effective against the problems and difficulties that are happening, you are instructed to list other strategies that may work better.
This worksheet gets you (or your client) thinking about what you are doing now and whether it is the best way forward.
2. ABC functional analysis
One popular technique in CBT is ABC functional analysis. Functional analysis helps you (or the client) learn about yourself, specifically, what leads to specific behaviors and what consequences result from those behaviors.
In the middle of the worksheet is a box labeled “Behaviors.” In this box, you write down any potentially problematic behaviors you want to analyze.
On the left side of the worksheet is a box labeled “Antecedents,” in which you or the client write down the factors that preceded a particular behavior. These are factors that led up to the behavior under consideration, either directly or indirectly.
On the right side is the final box, labeled “Consequences.” This is where you write down what happened as a result of the behavior under consideration. “Consequences” may sound inherently negative, but that’s not necessarily the case; some positive consequences can arise from many types of behaviors, even if the same behavior also leads to negative consequences.
This ABC Functional Analysis Worksheet can help you or your client to find out whether particular behaviors are adaptive and helpful in striving toward your goals, or destructive and self-defeating.
3. Case formulation worksheet
In CBT, there are 4 “P’s” in Case Formulation:
- Predisposing factors;
- Precipitating factors;
- Perpetuating factors; and
- Protective factors
They help us understand what might be leading a perceived problem to arise, and what might prevent them from being tackled effectively.
In this worksheet, a therapist will work with their client through 4 steps.
First, they identify predisposing factors, which are those external or internal and can add to the likelihood of someone developing a perceived problem (“The Problem”). Examples might include genetics, life events, or their temperament.
Together, they collaborate to identify precipitating factors, which provide insight into precise events or triggers that lead to “The Problem” presenting itself. Then they consider perpetuating factors, to discover what reinforcers may be maintaining the current problem.
Last, they identify protective factors, to understand the client’s strengths, social supports, and adaptive behavioral patterns.
Download this Case Formulation Worksheet as a PDF here.
4. Extended case formulation worksheet
This worksheet builds on the last. It helps you or your client address the “Four P Factors” described just above—predisposing, precipitating, perpetuating, and protective factors. This formulation process can help you or your client connect the dots between core beliefs, thought patterns, and present behavior.
This worksheet presents six boxes on the left of the page (Part A), which should be completed before moving on to the right-hand side of the worksheet (Part B).
- The first box is labeled “The Problem,” and corresponds with the perceived difficulty that your client is experiencing. In this box, you are instructed to write down the events or stimuli that are linked to a certain behavior.
- The next box is labeled “Early Experiences” and corresponds to the predisposing factor. This is where you list the experiences that you had early in life that may have contributed to the behavior.
- The third box is “Core Beliefs,” which is also related to the predisposing factor. This is where you write down some relevant core beliefs you have regarding this behavior. These are beliefs that may not be explicit, but that you believe deep down, such as “I’m bad” or “I’m not good enough.”
- The fourth box is “Conditional assumptions/rules/attitudes,” which is where you list the rules that you adhere to, whether consciously or subconsciously. These implicit or explicit rules can perpetuate the behavior, even if it is not helpful or adaptive. Rules are if-then statements that provide a judgment based on a set of circumstances. For instance, you may have the rule “If I do not do something perfectly, I’m a complete failure.”
- The fifth box is labeled “Maladaptive Coping Strategies” This is where you write down how well these rules are working for you (or not). Are they helping you to be the best you can be? Are they helping you to effectively strive towards your goals?
- Finally, the last box us titled “Positives.” This is where you list the factors that can help you deal with the problematic behavior or thought, and perhaps help you break the perpetuating cycle. These can be things that help you cope once the thought or behavior arises or things that can disrupt the pattern once it is in motion.
On the right, there is a flow chart that you can fill out based on how these behaviors and feelings are perpetuated. You are instructed to think of a situation that produces a negative automatic thought and record the emotion and behavior that this thought provokes, as well as the bodily sensations that can result. Filling out this flow chart can help you see what drives your behavior or thought and what results from it.
Download our PDF Extended Case Formulation Worksheet.
5. Dysfunctional thought record
This worksheet is especially helpful for people who struggle with negative thoughts and need to figure out when and why those thoughts are most likely to pop up. Learning more about what provokes certain automatic thoughts makes them easier to address and reverse.
The worksheet is divided into seven columns:
- On the far left, there is space to write down the date and time a dysfunctional thought arose.
- The second column is where the situation is listed. The user is instructed to describe the event that led up to the dysfunctional thought in detail.
- The third column is for the automatic thought. This is where the dysfunctional automatic thought is recorded, along with a rating of belief in the thought on a scale from 0% to 100%.
- The next column is where the emotion or emotions elicited by this thought are listed, also with a rating of intensity on a scale from 0% to 100%.
- Use this fifth column to note the dysfunctional thought that will be addressed. Example maladaptive thoughts include distortions such as over-inflating the negative while dismissing the positive of a situation, or overgeneralizing.
- The second-to-last column is for the user to write down alternative thoughts that are more positive and functional to replace the negative one.
- Finally, the last column is for the user to write down the outcome of this exercise. Were you able to confront the dysfunctional thought? Did you write down a convincing alternative thought? Did your belief in the thought and/or the intensity of your emotion(s) decrease?
Download this Dysfunctional Thought Record as a PDF.
6. Fact-checking
One of my favorite CBT tools is this Fact Checking Thoughts Worksheet because it can be extremely helpful in recognizing that your thoughts are not necessarily true.
At the top of this worksheet is an important lesson:
Thoughts are not facts.
Of course, it can be hard to accept this, especially when we are in the throes of a dysfunctional thought or intense emotion. Filling out this worksheet can help you come to this realization.
The worksheet includes 16 statements that the user must decide are either fact or opinion. These statements include:
- I’m a bad person.
- I failed the test.
- I’m selfish.
- I didn’t lend my friend money when they asked.
This is not a trick—there is a right answer for each of these statements. (In case you’re wondering, the correct answers for the statements above are as follows: opinion, fact, opinion, fact.)
This simple exercise can help the user to see that while we have lots of emotionally charged thoughts, they are not all objective truths. Recognizing the difference between fact and opinion can assist us in challenging the dysfunctional or harmful opinions we have about ourselves and others.
7. Cognitive restructuring
This worksheet employs the use of Socratic questioning, a technique that can help the user to challenge irrational or illogical thoughts.
The first page of the worksheet has a thought bubble for “What I’m Thinking”. You or your client can use this space to write down a specific thought, usually, one you suspect is destructive or irrational.
Next, you write down the facts supporting and contradicting this thought as a reality. What facts about this thought being accurate? What facts call it into question? Once you have identified the evidence, you can use the last box to make a judgment on this thought, specifically whether it is based on evidence or simply your opinion.
The next page is a mind map of Socratic Questions which can be used to further challenge the thought. You may wish to re-write “What I’m Thinking” in the center so it is easier to challenge the thought against these questions.
- One question asks whether this thought is truly a black-and-white situation, or whether reality leaves room for shades of gray. This is where you think about (and write down) whether you are using all-or-nothing thinking, for example, or making things unreasonably simple when they are complex.
- Another asks whether you could be misinterpreting the evidence or making any unverified assumptions. As with all the other bubbles, writing it down will make this exercise more effective.
- A third bubble instructs you to think about whether other people might have different interpretations of the same situation, and what those interpretations might be.
- Next, ask yourself whether you are looking at all the relevant evidence or just the evidence that backs up the belief you already hold. Try to be as objective as possible.
- It also helps to ask yourself whether your thought may an over-inflation of a truth. Some negative thoughts are based in truth but extend past their logical boundaries.
- You’re also instructed to consider whether you are entertaining this negative thought out of habit or because the facts truly support it.
- Then, think about how this thought came to you. Was it passed on from someone else? If so, is that person a reliable source of truth?
- Finally, you complete the worksheet by identifying how likely the scenario your thought brings up actually is, and whether it is the worst-case scenario.
These Socratic questions encourage a deep dive into the thoughts that plague you and offer opportunities to analyze and evaluate those thoughts. If you are having thoughts that do not come from a place of truth, this Cognitive Restructuring Worksheet can be an excellent tool for identifying and defusing them.
How is positive cognitive-behavioral therapy (CBT) different from traditional CBT?
Although both forms of CBT have the same goal of bringing about positive changes in a client’s life, the pathways used in traditional and positive CBT to actualize this goal differ considerably. Traditional CBT, as initially formulated by Beck (1967), focuses primarily on the following:
- Analyzing problems
- Lessening what causes suffering
- Working on clients’ weaknesses
- Getting away from problems
Instead, positive CBT, as formulated by Bannink (2012), focuses mainly on the following:
- Finding solutions
- Enhancing what causes flourishing
- Working with client’s strengths
- Getting closer to the preferred future
In other words, Positive CBT shifts the focus on what’s right with the person (rather than what’s wrong with them) and on what’s working (rather than what’s not working) to foster a more optimistic process that empowers clients to flourish and thrive.
In an initial study comparing the effects of traditional and Positive CBT in the treatment of depression, positive CBT resulted in a more substantial reduction of depression symptoms, a more significant increase in happiness, and it was associated with less dropout (Geschwind et al., 2019).

Some More CBT Interventions and Exercises
Haven’t had enough CBT tools and techniques yet? Read on for additional useful and effective exercises.
1. Behavioral experiments
These are related to thought experiments, in that you engage in a “what if” consideration. Behavioral experiments differ from thought experiments in that you actually test out these “what ifs” outside of your thoughts (Boyes, 2012).
In order to test a thought, you can experiment with the outcomes that different thoughts produce. For example, you can test the thoughts:
“If I criticize myself, I will be motivated to work harder” versus “If I am kind to myself, I will be motivated to work harder.”
First, you would try criticizing yourself when you need the motivation to work harder and record the results. Then you would try being kind to yourself and recording the results. Next, you would compare the results to see which thought was closer to the truth.
These Behavioral Experiments to Test Beliefs can help you learn how to achieve your therapeutic goals and how to be your best self.
2. Thought records
Thought records are useful in testing the validity of your thoughts (Boyes, 2012). They involve gathering and evaluating evidence for and against a particular thought, allowing for an evidence-based conclusion on whether the thought is valid or not.
For example, you may have the belief “My friend thinks I’m a bad friend.” You would think of all the evidence for this belief, such as “She didn’t answer the phone the last time I called,” or “She canceled our plans at the last minute,” and evidence against this belief, like “She called me back after not answering the phone,” and “She invited me to her barbecue next week. If she thought I was a bad friend, she probably wouldn’t have invited me.”
Once you have evidence for and against, the goal is to come up with more balanced thoughts, such as, “My friend is busy and has other friends, so she can’t always answer the phone when I call. If I am understanding of this, I will truly be a good friend.”
Thought records apply the use of logic to ward off unreasonable negative thoughts and replace them with more balanced, rational thoughts (Boyes, 2012).
Here’s a helpful Thought Record Worksheet to download.
3. Pleasant activity scheduling
This technique can be especially helpful for dealing with depression (Boyes, 2012). It involves scheduling activities in the near future that you can look forward to.
For example, you may write down one activity per day that you will engage in over the next week. This can be as simple as watching a movie you are excited to see or calling a friend to chat. It can be anything that is pleasant for you, as long as it is not unhealthy (i.e., eating a whole cake in one sitting or smoking).
You can also try scheduling an activity for each day that provides you with a sense of mastery or accomplishment (Boyes, 2012). It’s great to do something pleasant, but doing something small that can make you feel accomplished may have more long-lasting and far-reaching effects.
This simple technique can introduce more positivity into your life, and our Pleasant Activity Scheduling Worksheet is designed to help.
4. Imagery-based exposure
This exercise involves thinking about a recent memory that produced strong negative emotions and analyzing the situation.
For example, if you recently had a fight with your significant other and they said something hurtful, you can bring that situation to mind and try to remember it in detail. Next, you would try to label the emotions and thoughts you experienced during the situation and identify the urges you felt (e.g., to run away, to yell at your significant other, or to cry).
Visualizing this negative situation, especially for a prolonged period of time, can help you to take away its ability to trigger you and reduce avoidance coping (Boyes, 2012). When you expose yourself to all of the feelings and urges you felt in the situation and survive experiencing the memory, it takes some of its power away.
This Imagery Based Exposure Worksheet is a useful resource for this exercise.
5. Graded exposure worksheet
This technique may sound complicated, but it’s relatively simple.
Making a situation exposure hierarchy involves means listing situations that you would normally avoid (Boyes, 2012). For example, someone with severe social anxiety may typically avoid making a phone call or asking someone on a date.
Next, you rate each item on how distressed you think you would be, on a scale from 0 to 10, if you engaged in it. For the person suffering from severe social anxiety, asking someone on a date may be rated a 10 on the scale, while making a phone call might be rated closer to a 3 or 4.
Once you have rated the situations, you rank them according to their distress rating. This will help you recognize the biggest difficulties you face, which can help you decide which items to address and in what order. It’s often advised to start with the least distressing items and work your way up to the most distressing items.
Download our Graded Exposure Worksheet here.
A CBT Manual and Workbook for Your Own Practice and for Your Client

Some of these books are for the therapist only, and some are to be navigated as a team or with guidance from the therapist.
There are many manuals out there for helping therapists apply cognitive behavioral therapy in their work, but these are some of the most popular:
- A Therapist’s Guide to Brief Cognitive Behavioral Therapy by Jeffrey A. Cully and Andra L. Teten (PDF here);
- Individual Therapy Manual for Cognitive-Behavioral Treatment of Depression by Ricardo F. Munoz and Jeanne Miranda (PDF here);
- Provider’s Guidebook: “Activities and Your Mood” by Community Partners in Care (PDF here);
- Treatment Manual for Cognitive Behavioral Therapy for Depression by Jeannette Rosselló, Guillermo Bernal, and the Institute for Psychological Research (PDF here).
Here are some of the most popular workbooks and manuals for clients to use alone or with a therapist:
- The CBT Toolbox: A Workbook for Clients and Clinicians by Jeff Riggenbach (Amazon);
- Client’s Guidebook: “Activities and Your Mood” by Community Partners in Care (PDF here);
- The Cognitive Behavioral Workbook for Anxiety: A Step-by-Step Program by William J. Knaus and Jon Carlson (Amazon);
- The Cognitive Behavioral Workbook for Depression: A Step-by-Step Program by William J. Knaus and Albert Ellis (Amazon);
- Cognitive-Behavioral Therapy Skills Workbook by Barry Gregory (Amazon);
- A Course in CBT Techniques: A Free Online CBT Workbook by Albert Bonfil and Suraji Wagage (online here).
There are many other manuals and workbooks available that can help get you started with CBT, but the tools above are a good start. Peruse our article: 30 Best CBT Books to Master Cognitive Behavioral Therapy for an excellent list of these books.
5 Final Cognitive Behavioral Activities
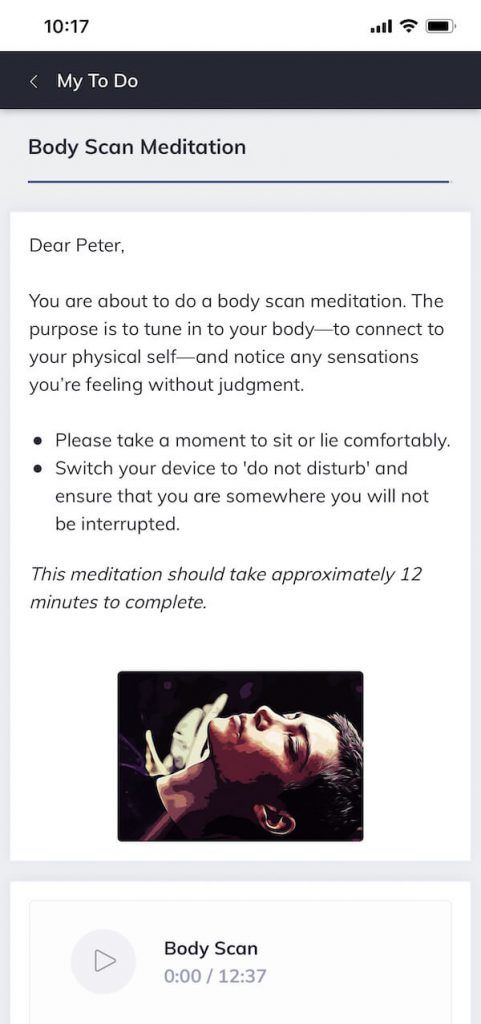
1. Mindfulness meditation
Mindfulness can have a wide range of positive impacts, including helping with depression, anxiety, addiction, and many other mental illnesses or difficulties.
The practice can help those suffering from harmful automatic thoughts to disengage from rumination and obsession by helping them stay firmly grounded in the present (Jain et al., 2007).
Mindfulness meditations, in particular, can function as helpful tools for your clients in between therapy sessions, such as to help ground them in the present moment during times of stress.
If you are a therapist who uses mindfulness-based approaches, consider finding or pre-recording some short mindfulness meditation exercises for your clients.
You might then share these with your clients as part of a toolkit they can draw on at their convenience, such as using the blended care platform Quenza (pictured here), which allows clients to access meditations or other psychoeducational activities on-the-go via their portable devices.
2. Successive approximation
This is a fancy name for a simple idea that you have likely already heard of: breaking up large tasks into small steps.
It can be overwhelming to be faced with a huge goal, like opening a business or remodeling a house. This is true in mental health treatment as well, since the goal to overcome depression or anxiety and achieve mental wellness can seem like a monumental task.
By breaking the large goal into small, easy-to-accomplish steps, we can map out the path to success and make the journey seem a little less overwhelming (e.g., Emmelkamp & Ultee, 1974).
3. Writing self-statements to counteract negative thoughts
This technique can be difficult for someone who’s new to CBT treatment or suffering from severe symptoms, but it can also be extremely effective (Anderson, 2014).
When you (or your client) are being plagued by negative thoughts, it can be hard to confront them, especially if your belief in these thoughts is strong. To counteract these negative thoughts, it can be helpful to write down a positive, opposite thought.
For example, if the thought “I am worthless” keeps popping into your head, try writing down a statement like “I am a person with worth,” or “I am a person with potential.” In the beginning, it can be difficult to accept these replacement thoughts, but the more you bring out these positive thoughts to counteract the negative ones, the stronger the association will be.
4. Visualize the best parts of your day
When you are feeling depressed or negative, it is difficult to recognize that there are positive aspects of life. This simple technique of bringing to mind the good parts of your day can be a small step in the direction of recognizing the positive (Anderson, 2014).
All you need to do is write down the things in your life that you are thankful for or the most positive events that happen in a given day. The simple act of writing down these good things can forge new associations in your brain that make it easier to see the positive, even when you are experiencing negative emotions.
5. Reframe your negative thoughts
It can be easy to succumb to negative thoughts as a default setting. If you find yourself immediately thinking a negative thought when you see something new, such as entering an unfamiliar room and thinking “I hate the color of that wall,” give reframing a try (Anderson, 2014).
Reframing involves countering the negative thought(s) by noticing things you feel positive about as quickly as possible. For instance, in the example where you immediately think of how much you hate the color of that wall, you would push yourself to notice five things in the room that you feel positively about (e.g., the carpet looks comfortable, the lampshade is pretty, the windows let in a lot of sunshine).
You can set your phone to remind you throughout the day to stop what you are doing and think of the positive things around you. This can help you to push your thoughts back into the realm of the positive instead of the negative.
A Take-Home Message
In this post, we offered many techniques, tools, and resources that can be effective in the battle against depression, anxiety, OCD, and a host of other problems or difficulties.
However, as is the case with many treatments, they depend on you (or your client) putting in a lot of effort. We encourage you to give these techniques a real try and allow yourself the luxury of thinking that they could actually work.
When we approach a potential solution with the assumption that it will not work, that assumption often becomes a self-fulfilling prophecy. When we approach a potential solution with an open mind and the belief that it just might work, it has a much better chance of succeeding.
So if you are struggling with negative automatic thoughts, please consider these tips and techniques and give them a shot. Likewise, if your client is struggling, encourage them to make the effort, because the payoff can be better than they can imagine.
If you are struggling with severe symptoms of depression or suicidal thoughts, please call the following number in your respective country:
- USA: National Suicide Prevention Hotline at 988;
- UK: Samaritans hotline at 116 123;
- The Netherlands: Netherlands Suicide Hotline at 09000767;
- France: Suicide écoute at 01 45 39 40 00;
- Germany: Telefonseelsorge at 0800 111 0 111 or 0800 111 0 222
For a list of other suicide prevention websites, phone numbers, and resources, see this website.
Please know that there are people out there who care and that there are treatments that can help.
Please let us know about your experiences with CBT in the comments section. If you’ve tried it, how did it work for you? Are there any other helpful exercises or techniques that we did not touch on in this piece? We’d love to know your thoughts.
We hope you enjoyed this article. For more information, don’t forget to download our three Positive CBT Exercises for free.
- Abramowitz, J. S. (1996). Variants of exposure and response prevention in the treatment of obsessive-compulsive disorder: A meta-analysis. Behavior Therapy, 27(4), 583-600.
- Anderson, J. (2014, June 12). 5 Get-positive techniques from cognitive behavioral therapy. Retrieved from http://www.everydayhealth.com/hs/major-depression-living-well/cognitive-behavioral-therapy-techniques/
- Arntz, A. (2002). Cognitive therapy versus interoceptive exposure as treatment of panic disorder without agoraphobia. Behaviour Research and Therapy, 40(3), 325-341.
- Bannink, F. (2012). Practicing positive CBT: From reducing distress to building success. John Wiley & Sons.
- Beck, A. T. (1967). Depression. Hoeber-Harper.
- Boyes, A. (2012, December 6). Cognitive behavioral therapy techniques that work: Mix and match cognitive behavioral therapy techniques to fit your preferences. Retrieved from https://www.psychologytoday.com/blog/in-practice/201212/cognitive-behavioral-therapy-techniques-work
- Chankapa, N. P. (2018). Effectiveness of cognitive behavioral therapy on depression and self-efficacy among out-patient female depressants in Sikkim (Masters dissertation). Retrieved from http://14.139.206.50:8080/jspui/bitstream/1/6059/1/nancy%20chankpa.pdf
- Davis, R. (2019, March 6). The complete list of cognitive behavioral therapy (CBT) techniques. Retrieved from https://www.infocounselling.com/list-of-cbt-techniques/
- Emmelkamp, P. M., & Ultee, K. A. (1974). A comparison of “successive approximation” and “self-observation” in the treatment of agoraphobia. Behavior Therapy, 5(5), 606–613.
- Geschwind, N., Arntz, A., Bannink, F., & Peeters, F. (2019). Positive cognitive behavior therapy in the treatment of depression: A randomized order within-subject comparison with traditional cognitive behavior therapy. Behaviour research and therapy, 116, 119-130.
- Grohol, J. (2016). 15 Common cognitive distortions. Retrieved from https://psychcentral.com/lib/15-common-cognitive-distortions/
- Hamamci, Z. (2002). The effect of integrating psychodrama and cognitive behavioral therapy on reducing cognitive distortions in interpersonal relationships. Journal of Group Psychotherapy, Psychodrama & Sociometry, 55(1), 3–14.
- Jain, S., Shapiro, S. L., Swanick, S., Roesch, S. C., Mills, P. J., Bell, I., & Schwartz, G. E. (2007). A randomized controlled trial of mindfulness meditation versus relaxation training: effects on distress, positive states of mind, rumination, and distraction. Annals of Behavioral Medicine, 33(1), 11-21.
- Larsson, A., Hooper, N., Osborne, L. A., Bennett, P., & McHugh, L. (2016). Using brief cognitive restructuring and cognitive defusion techniques to cope with negative thoughts. Behavior Modification, 40(3), 452-482.
- Martin, B. (2016). In-depth: Cognitive behavioral therapy. Retrieved from https://psychcentral.com/lib/in-depth-cognitive-behavioral-therapy/
- McCallie, M. S., Blum, C. M., & Hood, C. J. (2006). Progressive muscle relaxation. Journal of Human Behavior in the Social Environment, 13(3), 51-66.
- Pathak, N. (Ed.). (2018). Does cognitive behavioral therapy treat depression? Retrieved from https://www.webmd.com/g00/depression/guide/cognitive-behavioral-therapy-for-depression/
- Pruiksma, K. E., Cranston, C. C., Rhudy, J. L., Micol, R. L., & Davis, J. L. (2018). Randomized controlled trial to dismantle exposure, relaxation, and rescripting therapy (ERRT) for trauma-related nightmares. Psychological trauma: theory, research, practice, and policy, 10(1), 67-75.
- Psychology Tools. (n.d.). Retrieved from https://www.psychologytools.com/
- Therapist Aid. (n.d.). Retrieved from https://www.therapistaid.com/
- Utley, A., & Garza, Y. (2011). The therapeutic use of journaling with adolescents. Journal of Creativity in Mental Health, 6(1), 29-41.
Let us know your thoughts
Read other articles by their category
- Body & Brain (49)
- Coaching & Application (57)
- Compassion (26)
- Counseling (51)
- Emotional Intelligence (24)
- Gratitude (18)
- Grief & Bereavement (21)
- Happiness & SWB (40)
- Meaning & Values (26)
- Meditation (20)
- Mindfulness (45)
- Motivation & Goals (45)
- Optimism & Mindset (34)
- Positive CBT (29)
- Positive Communication (20)
- Positive Education (47)
- Positive Emotions (32)
- Positive Leadership (18)
- Positive Parenting (4)
- Positive Psychology (33)
- Positive Workplace (37)
- Productivity (17)
- Relationships (46)
- Resilience & Coping (36)
- Self Awareness (21)
- Self Esteem (38)
- Strengths & Virtues (32)
- Stress & Burnout Prevention (34)
- Theory & Books (46)
- Therapy Exercises (37)
- Types of Therapy (64)






What our readers think
Thanks for providing in-depth information on cognitive behavioral therapy techniques.
Loved the article. This was very useful, and very much appreciate all the free resources you included. Mahalo!
I am a nurse and a holistic life coach and these resources were very helpful to revise and improve my practice!
This is ridiculous. More ad than content. Misleading title.It is not a free website that you flood the viewers with so many ads. And if you are making so much money through ads then make the entire content free , since it is for the betterment of patients with mental health
Dear Prasun,
We agree, and we are currently looking for another solution as the site experience is suffering too much from this try-out.
Kind regards,
Julia | Community Manager
Thank you for the work put into this amazing article! It encompasses every bit of CBT that is so useful for clients increasing their understanding of how “this” works in a very well-written tone. Well done!
Thank you for the useful material that is free of charge. It will come in handy especially the providers guidebook “activities and your mood” for my client who has been diagnosed with depression.
It is very informative, keep up the good work