Benefits of CBT: 8+ Results of Cognitive Behavioral Therapy
 Cognitive-Behavioral Therapy (CBT) is considered to be one of the most rapid therapies there is when it comes to getting quick results.
Cognitive-Behavioral Therapy (CBT) is considered to be one of the most rapid therapies there is when it comes to getting quick results.
CBT is both brief and time-limited in comparison to other types of therapy. Cognitive-Behavioral Therapy is based upon the idea that our thoughts, not external events like people or situations, are actually the cause of our feelings and behaviors.
What this tells us is that we have a lot more control than we think and we can change things by changing our thoughts. In light of this, we have to ask ourselves what the research says about this groundbreaking therapy.
In this article, we will examine the scientific benefits as well as the research of Cognitive-Behavioral Therapy.
Before you continue, we thought you might like to download our three Positive CBT Exercises for free. These science-based exercises will provide you with detailed insight into Positive CBT and give you the tools to apply it in your therapy or coaching.
This Article Contains:
What are the Benefits of Cognitive-Behavioral Therapy?
According to the National Association of Cognitive-Behavioral Therapists (2021), CBT is based on the cognitive model of emotional response. This model tells us that our feelings and behaviors stem from our thoughts, as opposed to external stimuli. CBT is a goal-oriented and problem-focused therapy, unlike its psychoanalytical predecessors.
As a result of this, CBT focuses on the present and on the here and now, rather than on a lengthy analysis of the subject’s developmental history.
Cognitive-Behavioral Therapy is known for its quick results. Both therapists and psychologists use CBT in the treatment of certain mental disorders.
While the ideal number of CBT sessions a client should undertake will vary depending on their situation, treatments tend to range from between five to 20 sessions (Mayo Clinic, 2019). In comparison, other kinds of therapy may take months or even years of regular sessions in order to see results.
Other advantages of CBT include the fact that it:
- Is highly engaging.
- Holds the patient accountable for the therapeutic outcome.
- Is centered on the idea that one’s emotions and thoughts are responsible for how they behave and feel.
While CBT may not work for those with severe mental disorders or those with learning difficulties, it is a great form of therapy for helping people accept and understand that they can change things by simply changing their thoughts.
This is a major advantage because it helps people understand that altering their thought processes can lead to a positive outcome. This is a much different type of therapy in comparison to more traditional therapy, which typically focuses on trying to change or re-evaluate past actions or fears.
A Look at the Research

As such, it is used to ease the symptoms of a wide range of conditions, including (Hofmann, Asnaani, Vonk, Sawyer, & Fang, 2012):
- Substance use disorders
- Schizophrenia and other psychotic disorders
- Depression and Bipolar disorder
- Anxiety Disorders
- Somatoform disorders
- Eating disorders
- Insomnia
- Personality Disorders
- Aggression, anger and criminal behaviors
- Stress in general
- Distress due to medical conditions
- Chronic pain and fatigue
- Female hormonal conditions as well as pregnancy-related distress
In 2012, Hofmann and colleagues conducted a review of 106 meta-analyzes assessing CBT’s efficacy in treating these listed conditions.
Their findings revealed overwhelming support for CBT as an effective psychotherapeutic treatment option for all these conditions. In particular, the strongest support for the use of CBT was shown for anxiety disorders, somatoform disorders, bulimia, anger control problems, and general stress (Hofmann et al., 2012).
Additionally, of the eleven studies reviewed which compared the effects between CBT and other treatments or control conditions, patients undergoing CBT exhibited greater improvements than the comparison conditions in seven of the studies reviewed. Indeed, only one review identified CBT as being less effective than comparison treatments.
While not explored in Hofmann’s study, CBT is also widely used to help people with Obsessive-Compulsive Disorder (OCD). Commonly used components of CBT used in the treatment of OCD include exposure and response prevention as well as a range of cognitive interventions.
Evidencing CBT’s effectiveness for treating OCD, one study of fifty young people aged 12-17 years found that undergoing up to 14 sessions of CBT significantly reduced the sample’s symptoms of OCD and anxiety. Even more promising is that these improvements in OCD symptoms were shown to have been maintained in a six-month follow-up (Reynolds et al., 2013).
Overall, given the apparent effectiveness of CBT for easing the symptoms of such a wide range of conditions, the practice is now widely recognized as the current ‘gold standard’ of psychotherapy (David, Cristea, & Hofmann, 2018).
Different Types of CBT
Given CBT’s efficacy, many offshoots of this popular therapy have evolved, including:
- Positive CBT
- Behavioral Activation
- Trauma-focused CBT
- Acceptance and Commitment Therapy (ACT)
- Mindfulness-based CBT (MBCT)
According to research by Turner and Swearer Napolitano (2010), there is also a range of different therapeutic approaches that share the same theoretical underpinnings as CBT. These approaches include:
- Rational Emotive Behavior Therapy (REBT)
- Cognitive Therapy
- Rational Behavior Therapy
- Rational Living Therapy
- Schema-Focused Therapy
- Dialectical Behavior Therapy (DBT)
The Benefits of CBT for Anxiety

Therefore, we will now consider the evidence for the approach’s efficacy in the treatment of these conditions in turn.
To begin, CBT for the treatment of anxiety has been shown to be highly effective in both rigorous randomized placebo-controlled trials and natural field studies (Otte, 2011).
In randomized controlled trials, a treatment is compared against a placebo condition, where study participants have regular contact with a therapist and talk generally about their psychological issues, but the therapist does not apply a CBT approach to treatment. Therefore, all conditions surrounding the therapies remain the same, with the exception of the CBT paradigm, making it a strong test of CBT’s efficacy.
Promisingly, one review of 27 such trials found that CBT was significantly more effective than the control condition in treating a range of anxiety-related conditions, including social anxiety disorder, panic disorder, and generalized anxiety disorder (Hofmann & Smits, 2008).
In naturalistic settings, CBT has been shown to be similarly effective in the treatment of anxiety. In a review of 56 studies exploring real-world applications of CBT for anxiety, Stewart and Chambless (2009) again found strong evidence for the effectiveness of these treatments for anxiety comparable to that shown in well-controlled experimental conditions.
Overall, these findings point to CBT as a reliable and efficacious treatment option for a range of psychological conditions characterized by anxiety.
3 Instantly calming CBT techniques for anxiety – Mark Tyrrell
Can CBT Help with Depression?
Next, let’s review CBT for the treatment of depression.
Findings again indicate the effectiveness of CBT for the easing of depressive symptoms. However, the evidence suggesting that CBT is superior to other methods of treatment is not as strong.
Indeed, in a point of view colloquially known as the ‘Dodo bird verdict,’ some scholars and clinicians argue that all forms of psychotherapy are equally effective and that CBT is by no means superior.
In an effort to refute this claim, Honyashiki and colleagues (2014) conducted a review of 18 randomized placebo-controlled trials. The results found that CBT in the treatment of depression was significantly more likely to yield improvements than no-treatment conditions but that CBT was not necessarily more effective than psychological placebos (e.g., general talk therapy).
This result regarding the lack of difference between CBT and placebos appeared at least partially attributable to the length of the treatment. As participants underwent more CBT sessions, the improvements to their psychological states became more substantial.
In another review of 82 studies that examined CBT interventions in the treatment of depression, Lepping and colleagues (2017) found that CBT produced greater improvements among participants than other psychological or pharmacological treatments.
However, findings revealed that CBT applied in combination with a second active therapy, such as behavioral activation, produced even greater improvements for participants.
Therefore, results suggest that when using CBT to treat depression, clinicians can feel confident about the treatment’s efficacy. Nonetheless, careful consideration should be given to the number of sessions a client should undergo as well as whether any additional forms of treatment may help.
9 Ways to Implement These Beneficial CBT Practices
CBT is a firmly established method of treatment for many mental health conditions. The research also shows that the skills people learn through CBT last long after the treatment ends (Hawton, Salkovskis, Kirk, & Clark, 1989).
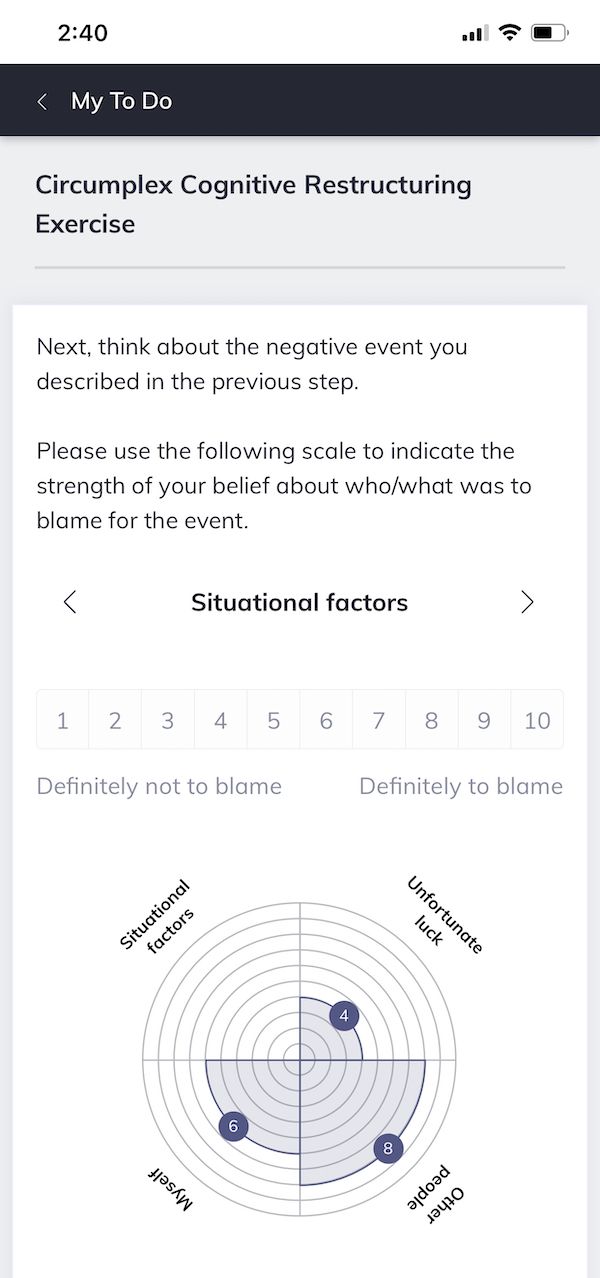
A key reason for CBT’s effectiveness lies in its applicability to real-life situations. To this end, CBT therapists are increasingly adopting a blended care approach to conducting CBT that encourages clients to practice interventions in their daily lives with the aid of portable technologies.
For example, using the e-therapy platform Quenza (pictured here), a CBT therapist can assign their client meditations, reflection exercises, and a range of other activities which clients can complete on the go via their smartphone or tablet.
The advantage of this convenience is that patients undergoing CBT can test their learned skills and techniques in response to real stressors in the environment.
For instance, while the practice of cognitive defusion—a technique that helps clients to reframe negative thoughts—is excellent in theory, being able to apply the technique independently upon receiving difficult feedback or finding oneself in conflict with a friend is likely to have myriad benefits for easing negative emotions and preventing negative thought-cycles in the moment.
6 Common CBT Interventions
Six common CBT interventions include things like:
- Learning how to set goals that are realistic and problem-solving.
- Learning how to better manage things like stress and anxiety.
- Learning how to identify situations that you might avoid and gradually approaching feared situations.
- Doing more enjoyable activities like hobbies, social activities, and exercise.
- Learning to identify and challenge automatic negative thoughts (ANTS).
- Journaling and keeping track of your feelings, thoughts, and behaviors (Patterson, 2009).
Setting realistic goals and learning how to solve problems might involve engaging in more social activities or learning how to be more assertive.
In order to better manage stress and anxiety, you can learn relaxation techniques and deep breathing techniques. You can also use positive self-talk or use a distraction technique like taking a deep breath to calm your energy in stressful situations.
Learning to be more comfortable in situations you might normally avoid is another good technique. This might involve networking more often or simply getting comfortable walking up to and greeting strangers at a party.
There is nothing more enjoyable than doing something you love, so engaging in hobbies and social activities can go a long way to helping you heal.
Because CBT involves changing how you think, it can also be helpful to identify and challenge those automatic negative thoughts. Instead of telling yourself things never work for you, try telling yourself that life supports you in every moment.
Keeping track of those negative thoughts, feelings and behaviors might also be helpful so it’s a good reason to journal or simply record your thoughts on a regular basis.
Other CBT Common Practices include:
- Mindfulness-based cognitive therapy
- Cognitive restructuring or reframing
- Cognitive journaling
The UK National Institute of Clinical Excellence has recently endorsed Mindfulness-Based Cognitive Therapy as an effective treatment for prevention and relapse for those who are clinically depressed (Crane & Kuyken, 2013). However, these same techniques can also help those who aren’t clinically depressed.
Mindfulness-Based Cognitive Therapy (MBCT) combines Cognitive-Behavioral techniques with mindfulness activities and strategies to help you better understand and manage your thoughts and emotions.
MBCT was originally developed to help give patients the necessary tools to combat depressive symptoms as they arise, but it can also be helpful for those who are merely looking for ways to combat stress.
Practicing mindfulness can also help you improve your mental and physical health. Mindfulness is all about turning off the endless chatter in your mind.
You can practice mindfulness by simply living in the present moment or by breathing in and out and observing the breath.
Mindfulness involves being aware of your thoughts, but not judging them. By observing your thoughts in a detached manner, you can let go of all cares and concerns.
Mindfulness practices are also a great way to combat those automatic negative thoughts.
Cognitive restructuring or reframing is another great technique. This technique allows you to identify the filter through which you see the world and change how you view things.
When you discover a belief that is destructive or harmful, you can then begin to challenge it and reframe it. When you reframe something, you learn to look at it differently.
When properly and consistently utilized, cognitive reframing can help you eliminate unproductive thoughts and challenging limiting beliefs.
Cognitive Reframing
Cognitive reframing involves:
- Learning about basic cognitive errors.
- Developing mental awareness.
- Challenging your conclusions.
- Replacing faulty beliefs.
The truth is, we all see the world a little differently. Because we see things differently, we form different conclusions about things. Learning about common mental errors, like blaming or emotional reasoning, can help us develop more mental awareness.
Challenging your conclusions allows you to reframe them and see things in a new light. Once you do all of this, you can then replace those faulty beliefs.
For example, just because you believe something to be true, doesn’t necessarily mean it is so.
Let’s say you believe life is hard and friends are hard to come by. You can begin by asking yourself a series of questions like:
- Why do I believe this is true?
- Where did these “beliefs” come from?
- What is it that is holding me back or keeping me from achieving success?
- What can I do to change it?
Try listing all of those negative beliefs or unproductive thoughts and then challenging yourself to think about them in a more productive way.
Instead of saying “I am not a people person,” you can turn the statement around and say “I have some great people in my life” instead.
Rewriting your thoughts is also a great way to start thinking differently.
Cognitive Journaling
Cognitive journaling is another great technique. Cognitive journaling uses something known as the “ABC Model” where you also include the letter D for Disputing.
ABC stands for:
- Activating Event – The actual event and your immediate interpretations of the event.
- Beliefs about the event – Which can be rational or irrational.
- Consequences – How you feel, what you do or other thoughts.
- Disputing – Identifying alternative beliefs that would lead to healthier consequences.
Let’s look at an activating event involving someone who constantly interrupts you or talks over you.
As a result of this, you may believe this person doesn’t like you. You may deem them rude. You may even think your thoughts aren’t important to them. These are your beliefs.
The consequences are that you feel bad. You may get anxious or nervous or even annoyed.
To dispute this, you have to look at things differently. Maybe this person is just excited to tell you something. Maybe they didn’t do it on purpose. Maybe you could simply mention the fact that this bothers you, and let it go. It’s not about YOU.
A Take-Home Message
Cognitive-Behavioral Therapy is a technique that is highly engaging and a technique that offers quick results when compared to standard psychotherapy.
CBT helps us understand that we have the power to change things. CBT tells us that external situations, interactions with others’ and negative events are not actually responsible for our poor moods and problems.
The truth is that our own reactions to events and the things we tell ourselves about those events are most likely the cause.
With Cognitive-Behavioral Therapy, you can learn to change the way you think, which in turn changes the way you feel. All of that then changes the way you view the world and how you handle difficult situations when they do arise.
The better you become at disrupting those unproductive thoughts, the happier you will be.
We hope you enjoyed reading this article. For more information, don’t forget to download our three Positive CBT Exercises for free.
- Crane, R. S., & Kuyken, W. (2013). The implementation of mindfulness-based cognitive therapy: Learning from the UK health service experience. Mindfulness, 4(3), 246-254.
- David, D., Cristea, I., & Hofmann, S. G. (2018). Why cognitive behavioral therapy is the current gold standard of psychotherapy. Frontiers in Psychiatry, 9.
- Hawton, K. E., Salkovskis, P. M., Kirk, J. E., & Clark, D. M. (1989). Cognitive behaviour therapy for psychiatric problems: A practical guide. New York, NY: Oxford University Press.
- Hofmann, S. G., Asnaani, A., Vonk, I. J., Sawyer, A. T., & Fang, A. (2012). The efficacy of cognitive behavioral therapy: A review of meta-analyses. Cognitive Therapy and Research, 36(5), 427-440.
- Hofmann, S. G., & Smits, J. A. (2008). Cognitive-behavioral therapy for adult anxiety disorders: a meta-analysis of randomized placebo-controlled trials. The Journal of Clinical Psychiatry, 69(4), 621-632.
- Honyashiki, M., Furukawa, T. A., Noma, H., Tanaka, S., Chen, P., Ichikawa, K., … & Caldwell, D. M. (2014). Specificity of CBT for depression: A contribution from multiple treatments meta-analyses. Cognitive Therapy and Research, 38(3), 249-260.
- Lepping, P., Whittington, R., Sambhi, R. S., Lane, S., Poole, R., Leucht, S., … & Waheed, W. (2017). Clinical relevance of findings in trials of CBT for depression. European Psychiatry, 45, 207-211.
- Mayo Clinic. (2019). Cognitive behavioral therapy. Retrieved from https://www.mayoclinic.org/tests-procedures/cognitive-behavioral-therapy/about/pac-20384610#
- National Association of Cognitive-Behavioral Therapists. (2021). What is cognitive-behavioral therapy? Retrieved from https://www.nacbt.org/whatiscbt-htm/
- Otte C. (2011). Cognitive-behavioral therapy in anxiety disorders: Current state of the evidence. Dialogues in Clinical Neuroscience, 13(4), 413–421.
- Patterson, M. (2009). CBT in practice: Part science, part art. Visions Journal, 6(1).
- Reynolds, S. A., Clark, S., Smith, H., Langdon, P. E., Payne, R., Bowers, G., … & McIlwham, H. (2013). Randomized controlled trial of parent-enhanced CBT compared with individual CBT for obsessive-compulsive disorder in young people. Journal of Consulting and Clinical Psychology, 81(6), 1021-1026.
- Stewart, R. E., & Chambless, D. L. (2009). Cognitive–behavioral therapy for adult anxiety disorders in clinical practice: A meta-analysis of effectiveness studies. Journal of Consulting and Clinical Psychology, 77(4), 595–606.
- Turner, R., & Swearer Napolitano, S. (2010). Cognitive Behavioral Therapy (CBT). In C. Clauss-Ehlers (Ed.), Encyclopedia of cross-cultural school psychology (pp. 226-229). New York, NY: Springer.
Let us know your thoughts
Read other articles by their category
- Body & Brain (49)
- Coaching & Application (57)
- Compassion (26)
- Counseling (51)
- Emotional Intelligence (24)
- Gratitude (18)
- Grief & Bereavement (21)
- Happiness & SWB (40)
- Meaning & Values (26)
- Meditation (20)
- Mindfulness (45)
- Motivation & Goals (45)
- Optimism & Mindset (34)
- Positive CBT (29)
- Positive Communication (20)
- Positive Education (47)
- Positive Emotions (32)
- Positive Leadership (18)
- Positive Parenting (4)
- Positive Psychology (33)
- Positive Workplace (37)
- Productivity (17)
- Relationships (46)
- Resilience & Coping (36)
- Self Awareness (21)
- Self Esteem (38)
- Strengths & Virtues (32)
- Stress & Burnout Prevention (34)
- Theory & Books (46)
- Therapy Exercises (37)
- Types of Therapy (64)





What our readers think
I read your whole paid and I’m starting cbt soon and a lot you talk about scares me very much i just hope it can really help me as i find myself unfixed at times so I’m going to give it all i got and hope for the best thank you for all your knowledge now g just have to get my feet wet take care
I am currently writing a paper for school about cognitive behavioral therapy. How might I use the information from the article to site as a reference?
Hi Z Jones,
You can cite the article using APA 7th formatting as follows:
Riopel, L. (2020). 8 Benefits of Cognitive Behavioral Therapy (CBT) according to science. PositivePsychology.com. Retrieved from https://positivepsychology.com/benefits-of-cbt/
Good luck with your paper!
– Nicole | Community Manager
Pls help on CBT therapy for depression
Hi Guna,
You can find more information about CBT for depression at this link.
– Nicole | Community Manager
Hi Guna,
You can read more about CBT for depression here. If you search your local area, you should be able to find a CBT therapist who can work with you on depression within a CBT framework.
Hope this helps.
– Nicole | Community Manager
it’s benefit for our daily life
Dear Leslie, this article is extremely informative and helpful. With your permission and agreement I would like to use this info and quotes for a book I am working on. Please email me at supersailorshine@gmail.com
Thank you!
Lauren
Hi Lauren
Glad to hear you found it informative. You are welcome to share it by clicking on the big green YES option at the bottom of the post, which will give you sharing options.
All the best,
Annelé