12 Most Reliable Mental Health Assessment Tools
 Assessment tools remain a cornerstone of many professions centering around the human mind.
Assessment tools remain a cornerstone of many professions centering around the human mind.
Typically, these assessments invite clients to respond to questions about their mental state and subjective experiences.
Psychologists and therapists depend on these tools to make decisions about the best course of treatment for clients seeking support for their mental health. Therefore, it’s worth taking a little time to explore their variations and how to use them most effectively.
In this article, we’ll explore some of the most commonly used and reliable mental health assessments, as well as their applications at different stages of the therapeutic process. We’ll also walk through some ways you can automate and simplify the administration of these assessments.
Before you continue, we thought you might like to download our three Positive Psychology Exercises for free. These science-based exercises explore fundamental aspects of positive psychology, including strengths, values, and self-compassion, and will give you the tools to enhance the wellbeing of your clients, students, or employees.
This Article Contains:
- What Are Psychological Assessments? 3 Examples
- How to Use Therapy Assessment Tools
- 3 Reliable Psychological Tests & Assessments
- 13 Questions and Worksheets to Assess Clients
- Using Online Tools for Psychology Assessments
- Crafting Assessments in Quenza: 3 Templates
- Helpful Resources From PositivePsychology.com
- A Take-Home Message
- References
What Are Psychological Assessments? 3 Examples
Whether it’s a pop psychology quiz online or a validated assessment by a therapist, psychological assessments share one thing in common.
They all function as
“a systematic procedure for comparing the behavior of two or more persons.”
Cronbach, 1949, p. 21
In recent years, scientists have begun making distinctions between psychological tests versus assessments.
While tests are typically thought of as pen-and-paper or computer-based tools for considering differences between people, the term ‘assessment’ acknowledges the wide variety of other approaches a psychologist may use to evaluate these differences. Examples of such approaches include interviews, observations, and recording physiological functions (Goldstein, Allen, & DeLuca, 2019).
To begin, here are three examples of mental health tests commonly used among mental health practitioners.
1. Minnesota Multiphasic Personality Inventory (MMPI-2)
First published in 1989, the MMPI-2 is the world’s most widely used psychometric test for measuring mental health ailments that feature as forms of psychopathology (Rogers, Robinson, & Jackson, 2016).
The scale features 567 true–false statements, which assess 10 clinical sub-scales (Butcher, Dahlstrom, Graham, Tellegen, & Kaemmer, 1989):
- Hypochondriasis
- Depression
- Hysteria
- Psychopathic deviate
- Masculinity/Femininity
- Paranoia
- Psychasthenia
- Schizophrenia
- Hypomania
- Social introversion
In addition to these 10 primary clinical scales, the MMPI-2 also contains three sub-scales to detect lying, defensiveness, and inconsistent responses.
It also features many additional content scales assessing specific cognitions, behaviors, physical experiences, and motivations, such as self-doubt, competitive drive, and gastrointestinal issues.
If you’re interested in administering this assessment yourself, you can order a copy of the test from the Pearson Assessments website.
2. Beck Anxiety Inventory
Another commonly used mental health assessment is the Beck Anxiety Inventory. This inventory is a brief self-report test used to assess the severity of symptoms of anxiety. It includes detailed scoring to help practitioners identify whether clients’ presenting symptoms of anxiety are within a normal range or severe and debilitating.
The scale comprises 21 common symptoms of anxiety. Examples include:
- Hands trembling
- Fear of dying
- Hot/cold sweats
Respondents indicate the frequency with which each symptom has bothered them for the past month on a 4-point scale, where 0 is ‘not at all,’ and 3 is ‘severely – it bothered me a lot.’
You can access a copy of the test for free from the Great Plains Health website.
3. Beck Depression Inventory
Finally, a standard complement to the Beck Anxiety Inventory is the Beck Depression Inventory. Again, this inventory consists of 21 items and contains detailed scoring information to indicate whether symptoms are in a normal range or severe.
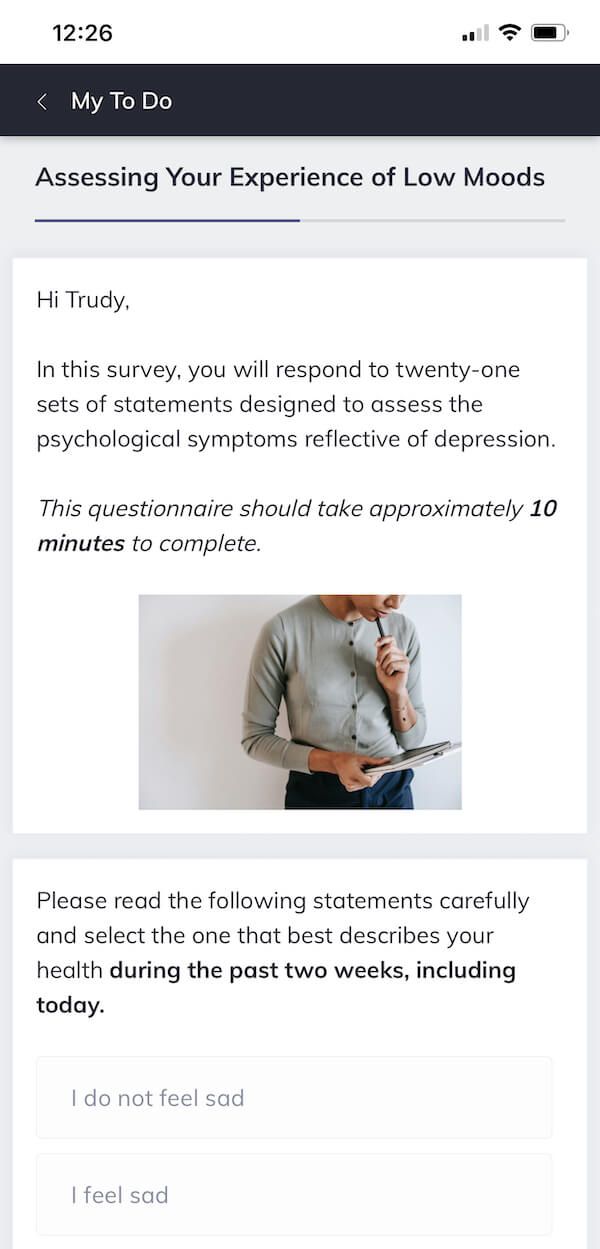
Respondents complete each item of the scale by selecting the statement that best reflects their current emotional state. For example, the first item and accompanying scoring are as follows:
- 0 – I do not feel sad.
- 1 – I feel sad.
- 2 – I am sad all the time, and I can’t snap out of it.
- 3 – I am so sad and unhappy that I can’t stand it.
If you’re interested, the Beck Depression Inventory with scoring information is freely available to download.
Beck’s depression inventory – Practical Psychology
Using tests for holistic mental health assessments
Regardless of which test you use, each can form part of a holistic mental assessment for clients that guides the design of subsequent therapeutic interventions.
To illustrate, consider this sample interpretive report following the administration of the MMPI-2 (Pearson Education, 2014).
The assessment results for this example patient, Karen, point toward a likely diagnosis of schizophrenia or major affective disorder as well as potential challenges in the therapeutic process. Namely, several of her responses suggest that she may possess little faith in her ability to improve her mental health and a lack of trust that may impact her relationship with a therapist.
It is subsequently suggested that she may benefit from minimal face-to-face contact and brief, periodic visits with a mental health professional.
Information such as this can form part of a holistic assessment, which monitors Karen’s ongoing engagement with therapeutic interventions (or lack thereof) and determines her likelihood of seeing positive improvements to her mental health.
It might even inform a therapist’s hypothesis that Karen could benefit from therapy of particular duration, such as solution-focused brief therapy, or specific modes of delivery, such as teletherapy or blended modes of treatment.
Next, we’ll consider some of these different delivery modes as well as blended technology’s uses for facilitating ongoing mental health assessment.
How to Use Therapy Assessment Tools
Therapists can use mental health assessments to achieve a range of goals at different stages of the therapeutic process, all of which can be streamlined using online tools.
Throughout this article, we’ll explore the applications of the online psychotherapy tool Quenza (pictured here), which is a powerful platform that helps practitioners automate and scale several aspects of the assessment process.
At the beginning of the therapeutic relationship, practitioners using the platform will send a digital invitation to their clients to sign up for a free account.
Following this initial step, most of the client’s engagement with the platform will occur when prompted via push notifications on their smartphone.
Once a client is registered, Quenza can help the practitioner carry out two key aspects of a mental health assessment. These include pre- and post-treatment assessments and ongoing assessment of intervention efficacy using repeated measurements across time.
Pre-treatment assessments can help practitioners determine which mode of treatment or intervention is most likely to have the greatest benefit based on presenting symptoms.
Likewise, the therapist may administer a post-treatment test to determine how effective an intervention has been at reducing symptoms or increasing signs of psychological flourishing.
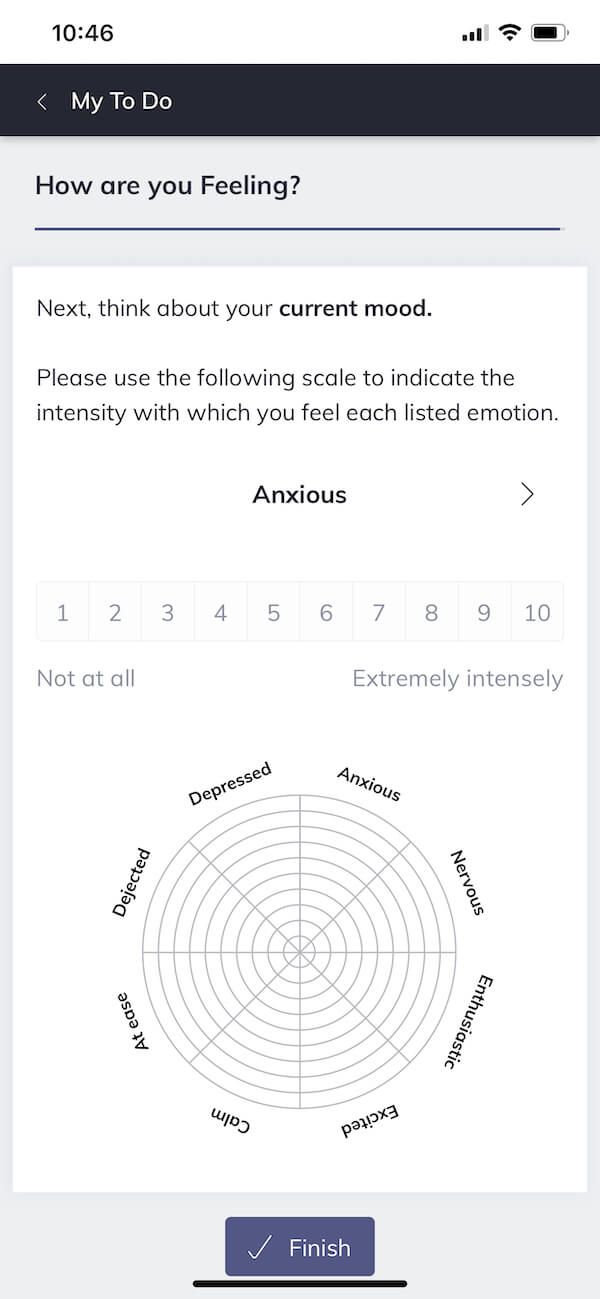
Regarding ongoing assessments, it can be helpful to encourage clients to provide regular feedback on aspects of their treatment. Using Quenza, this can be accomplished by assigning brief tests or reflections assessing factors like mood, cognitions, and behaviors, which clients can complete at regular intervals.
For instance, pictured here is a daily emotion reflection, which clients can complete each day on their smartphone to help track changes in their emotions. The practitioner can then review a client’s aggregate responses to these reflections via Quenza’s online dashboard to make inferences about the effectiveness of ongoing interventions.
A key advantage of using an online platform to conduct these one-off and ongoing assessments is that it allows the practitioner to monitor their clients’ progress with interventions between sessions.
It also gives practitioners the flexibility to design assessments that tap into the specific foci of interest to them and their clients, rather than being constrained by the questions included in standardized questionnaires and forms.
3 Reliable Psychological Tests & Assessments
So far, we’ve looked at the MMPI-2 and the Beck Inventories as examples of reliable and widely used psychological tests for assessing mental health. We’ve also considered how we might administer these tests efficiently as part of a one-off or ongoing assessment.
Let’s now consider three more freely available tests for assessing experiences reflective of one’s mental health.
But before we dive in, a quick note. These assessments are not designed to be self-administered. Rather, they should be administered by licensed practitioners and only within the bounds of your professional expertise.
Dissociation – Brief Dissociative Experiences Scale
Dissociation is a common characteristic of a range of mental health disorders, including post-traumatic stress disorder and bipolar disorder (Hariri et al., 2015). Therefore, when clients show signs of dissociation, it may be wise to administer an assessment.
One widely used test assessing dissociation is the Brief Dissociative Experiences Scale.
This measure consists of eight items assessing the frequency with which a client has experienced various dissociative symptoms over the past seven days.
Example items from the scale are:
- I find myself staring into space and thinking of nothing.
- People, objects, or the world around me seem strange or unreal.
- When I am alone, I talk out loud to myself.
All items are presented on 5-point scales, where 0 is ‘not at all,’ and 4 is ‘more than once a day.’
A full copy of the scale and scoring information can be downloaded from the American Psychiatric Association website.
Misophonia – Amsterdam Misophonia Scale
Misophonia is defined as
“a relatively unexplored chronic condition in which a person experiences autonomic arousal (analogous to an involuntary ‘fight-or-flight’ response) to certain innocuous or repetitive sounds such as chewing, pen clicking, and lip smacking.”
Edelstein, Brang, Rouw, & Ramachandran, 2013
The experience of misophonia can compel someone to avoid situations that may trigger this autonomic arousal, potentially making it difficult to work and socialize. Misophonic experiences have the potential to negatively impact mental health and quality of life.
One tool for assessing the experience of misophonia is the Amsterdam Misophonia Scale (Schröder, Vulink, & Denys, 2013).
This scale comprises six items assessing different features of misophonic experiences, including their frequency and the extent to which they disrupt a patient’s day-to-day functioning.
Example items from the scale are:
- How much of your time is occupied by misophonic sounds?
- How much distress do the misophonic sounds cause you?
- How much effort do you make to resist the (thoughts about the) misophonic sounds?
A free copy of the scale can be obtained from the Misophonia Treatment website.
Intolerance of Uncertainty – Intolerance of Uncertainty Scale Short Form
The inability to tolerate uncertainty can have direct deleterious effects on mental wellbeing (Satici, Saricali, Satici, & Griffiths, in press). Therefore, how a client tolerates uncertainty may sometimes be a relevant focus for assessment.
The Short Form Intolerance of Uncertainty Scale (Carleton, Norton, & Asmundson, 2007) is one of the most commonly used scales for assessing uncertainty intolerance and its effects on mental health.
This scale consists of 12 items asking respondents to indicate the extent to which they agree with a list of statements.
Example items from the scale are:
- Unforeseen events upset me greatly.
- I can’t stand being taken by surprise.
- The smallest doubt can stop me from acting.
All items are presented on 5-point scales, where 1 is ‘not at all characteristic of me,’ and 5 is ‘entirely characteristic of me.’
13 Questions and Worksheets to Assess Clients

However, there are also questions and exercises that may flag the potential need for these more specific diagnoses. This may require practitioners to ask a series of general therapy questions before diving in for a deeper analysis of specific symptoms.
To help, here are seven useful questions you might ask your clients early in the therapeutic process or session (adapted from Aidala, Havens, Peake, & Keane, 2002).
Note that these questions could invite a combination of open-ended responses and numerical responses on Likert scales.
- How have things been going for you in terms of your mood or feelings?
- Were there any periods when you were very sad or depressed?
- How about any times when you were very nervous, frightened, or worried about things?
- Were there times when you were so active or hyper that you couldn’t slow down?
Depending on when symptoms of ill mental health started presenting (or in cases where an event triggered them), you may find it helpful to anchor the mental health questions in specific timeframes, such as in the following examples:
- During the last month, was there a time when you had little interest or pleasure in doing things? If so, how often did you feel that way?
- Over the last week, how often have you had trouble falling or staying asleep? What about sleeping too much?
- In the last four weeks, have you had an anxiety attack (i.e., sudden feelings of fear or panic)?
In addition to the above questions, here are six worksheets that can support you in exploring your clients’ mental health. Several of these are preloaded activities on Quenza, which you can access and try for yourself via the platform’s no-risk 30-day trial.
1. Moving from Cognitive Fusion to Defusion
Central to the practice of Cognitive-Behavioral Therapy is the understanding that our thoughts have the potential to strengthen or weaken emotional states brought about by events in our environment. Therefore, we can change our emotional experiences by changing our thoughts.
The Cognitive Fusion to Defusion worksheet on Quenza is designed to help your clients take a step back when growing overwhelmed by self-critical thoughts. In particular, the worksheet invites the user to begin noticing their thoughts nonjudgmentally as opposed to getting caught up in them. Consequently, they can reduce their belief that intrusive thoughts are true or must dictate their behaviors.
2. S.O.B.E.R. Stress Interruption Technique
For some clients, difficulties managing stress can exacerbate problems with mental health. For these clients, try inviting them to apply the S.O.B.E.R. Stress Interruption Technique. This exercise and accompanying worksheet are available digitally through Quenza’s Expansion Library.
The acronym S.O.B.E.R. stands for Stop, Observe, Breathe, Expand awareness, and Respond with awareness. To apply the technique during stressful times, clients begin by listening to an eight-minute audio meditation that guides them through the five S.O.B.E.R. steps. The activity then concludes with a reflection, encouraging them to consider other situations in which they may benefit from applying the technique.
3. Brief Needs Check-In
The final worksheet we’ll look at from Quenza is the Brief Needs Check-In.
A core part of caring for our mental health involves recognizing and taking the time to meet our emotional needs. The Brief Needs Check-in is useful for helping clients anchor themselves in the present moment and stop to consider their needs. The activity then guides clients as they plan out how to satisfy any unmet emotional needs in an act of self-care.
4. Preventing Mental Health Relapse
When clients are undertaking therapy for mental health conditions, there are likely to be times when they fall back into old or unhelpful habits.
The Preventing Mental Health Relapse worksheet is designed to help your clients track the symptoms of mental illness, recognize early signs that they may be ‘relapsing’ (e.g., falling into a depressive spell), and plan adaptive strategies to help them cope.
5. Self-Care Checkup
Whether we have a mental illness or not, all of us need to take time out for ourselves to maintain good mental health.
The Self-Care Checkup worksheet lists a wide range of self-care activities and invites your clients to consider which ones they typically engage in. In doing so, the worksheet encourages clients to assess the frequency and quality of their self-care across the emotional, physical, social, professional, and spiritual domains of their life.
6. Understanding Mental Health Stigma
It is not uncommon for therapy clients to experience embarrassment or shame at needing support for their mental health. Likewise, others in their life may hold a stigmatizing view about mental illness or attending therapy.
The Understanding Mental Health Stigma worksheet explores some dangers of mental health stigma and makes recommendations for how we might reduce misunderstanding around mental illness. In particular, this worksheet may serve as a handy communication aid for clients looking to start a constructive conversation about mental health with others in their life.
Using Online Tools for Psychology Assessments
Let’s now delve into some practical applications of these assessment tools with an example designed in Quenza.
Quenza allows practitioners to draw on a growing library of tests and assessments or design their own.
These can focus on a broad range of themes, including wellbeing, interpersonal functioning, and emotional volatility.
Therapists can then administer these activities to their clients digitally to be completed via their own smartphone or tablet.
For instance, therapists can choose to administer a single test, such as the Beck Depression Inventory (pictured here) or administer a sequence of tests as part of an ongoing assessment. In Quenza, this sequence is referred to as a pathway.
For instance, a therapist might schedule a pathway of mental health activities assessing the intensity of emotions throughout a week. Using Quenza, the therapist can automatically send these according to a pre-programmed schedule and then facilitate a discussion regarding patterns in these responses during their next in-person session with the client.
Additionally, practitioners using Quenza are not limited to designing and administering assessments. Rather, they can create any number of activities, including audio meditations and lessons.
For example, as a part of a mental health intervention, a therapist might record one week’s worth of five-minute meditations and send a push notification to their client each morning, reminding them to meditate.
They might then follow up each meditation with a digital reflection that invites clients to consider their emotional health following the period of meditation.
For an entirely fresh approach, therapists may even wish to design toolkits of activities, meditations, and videos that clients can draw on as needed, rather than according to a schedule. That way, clients will have a bank of custom-made tools in their back pocket to help them cope during times of stress.
These are just a few examples of the different ways you can use this platform to administer your mental health assessments.
Crafting Assessments in Quenza: 3 Templates
Let’s now look at three useful activity templates in Quenza you can use to design a mental health assessment pathway of your own. You’ll find each of these in Quenza’s ever-growing Expansion Library.
Stress Diary Pathway
Among Quenza’s ready-to-use tools is its Stress Diary. This preloaded expansion is a complete pathway that invites your clients to reflect on their experience of stress for seven days.
Each day, your client will receive a push notification reminding them to complete their day’s diary entry. They will be prompted to rate the intensity of their stress reactions, note the day’s most stressful event, reflect on their emotional responses to stress, and consider their chosen coping strategies.
At the end of the week, clients will review their diary entries and analyze them for patterns.
The Stress Diary can serve as a valuable exercise to help clients practice noticing their emotional reactions, which is a behavior that in itself may take practice. Likewise, the diary can serve as a form of ongoing assessment during particularly stressful periods or as a way to capture improvements (e.g., the use of positive coping strategies) throughout the therapeutic process.
Life Domain Satisfaction Activity
Many clients who seek therapy do so because challenges with their mental health have hampered their ability to function across different domains of life.
Quenza’s Life Domain Satisfaction activity can serve as an enlightening activity to assess these impacts as part of a pre/post-assessment of change. In short, this activity invites clients to rate their satisfaction across 16 domains of life using 10-point rating scales.
Given that all of Quenza’s preloaded activities are fully customizable, practitioners can easily adapt this template to invite open-ended responses exploring the impact that the client’s mental health has had on their satisfaction with each of these domains.
These responses may then serve as useful signposts for whether mental health interventions are enabling clients to achieve their initial aims for seeking therapy and deriving greater satisfaction from life.
Outcome Rating Scale Activity
Finally, Quenza’s Outcome Rating Scale activity is a useful tool for assessing improvements to a client’s mental health. In particular, it quickly assesses four areas of functioning known to change as a result of therapeutic intervention relating to wellbeing and interpersonal functioning using 10-point rating scales.
Again, practitioners may choose to combine this single activity template with a range of other activities in a pathway as part of an ongoing mental health assessment.
For instance, if a client is practicing mindfulness as part of a mental health intervention, the practitioner may alternate sending weekly meditations via Quenza with the Outcome Rating Scale to assess trajectories in mental wellbeing flowing from the intervention.
Helpful Resources From PositivePsychology.com
Looking for more tools to help assess your clients’ mental health and wellbeing? Check out the following free assessment tools from our blog.
- Perfectionist Beliefs ‘Flexibility’ Self-Assessment
This short assessment presents a series of questions to help clients identify areas where their thinking is rigid and instances when they might benefit from relaxing perfectionist tendencies. - Self-Care Check-In
This self-assessment uses ratings and reflection questions to help clients determine how they can better meet their self-care needs. - Thoughts and Feelings: Struggle or Acceptance?
This 15-item questionnaire will help you quickly assess the extent to which a client adopts an attitude of acceptance when facing unavoidable discomfort and challenges. - Codependency Questionnaire
This questionnaire, adapted from research, presents 20 statements assessing a client’s tendency to display symptoms of codependency.
If you’re looking for more science-based ways to help others enhance their wellbeing, this signature collection contains 17 validated positive psychology tools for practitioners. Use them to help others flourish and thrive.
A Take-Home Message
It’s clear that assessment tools are critical for mental health professionals to do their work.
Thankfully, researchers and practitioners have designed a vast array of tools and tests to assess everything from the common experience of anxiety to the lesser known disturbances associated with misophonia.
Further, clinicians are becoming increasingly creative in their application of these tools. Rather than the standard pre/post-assessments that once dominated therapeutic practice, modern technologies are making it easier to conduct ongoing assessments involving repeated measurements across time.
If you’re a mental health practitioner, we hope this article has inspired you to consider how you might better use the tools at your disposal to assess your clients’ mental health.
And if it has, let us know what you’re planning to do differently in the comments. We’d love to hear from you.
We hope you enjoyed reading this article. Don’t forget to download our three Positive Psychology Exercises for free.
- Aidala, A., Havens, J., Peake, M., & Keane, T. (2002). Use of Client Diagnostic Questionnaire (CDQ): Training manual. Retrieved from https://targethiv.org/sites/default/files/file-upload/resources/Client_Diagnostic_Questionnaire.pdf
- Butcher, J. N., Dahlstrom, W. G., Graham, J. R., Tellegen, A., & Kaemmer, B. (1989). Manual for administration and scoring: MMPI-2. University of Minnesota Press.
- Carleton, R. N., Norton, M. P. J., & Asmundson, G. J. (2007). Fearing the unknown: A short version of the Intolerance of Uncertainty Scale. Journal of Anxiety Disorders, 21(1), 105–117.
- Cronbach, L. J. (1949). Essentials of psychological testing. Harper.
- Edelstein, M., Brang, D., Rouw, R., & Ramachandran, V. S. (2013). Misophonia: Physiological investigations and case descriptions. Frontiers in Human Neuroscience, 7, 296.
- Goldstein, G., Allen, D. N., & Deluca, J. (2019). Historical perspective. In G. Goldstein, D. N. Allen, D. N., & J. Deluca (Eds.), Handbook of psychological assessment (4th ed.). Elsevier.
- Hariri, A. G., Gulec, M. Y., Orengul, F. F. C., Sumbul, E. A., Elbay, R. Y., & Gulec, H. (2015). Dissociation in bipolar disorder: Relationships between clinical variables and childhood trauma. Journal of Affective Disorders, 184, 104–110.
- Park, C. L., Cohen, L. H., & Murch, R. L. (1996). Assessment and prediction of stress‐related growth. Journal of Personality, 64(1), 71–105.
- Pearson Education. (2014). Case description: Karen Z–Inpatient mental health interpretive report. Retrieved from https://images.pearsonclinical.com/images/Assets/MMPI-2Clinical/MMPI-2_AdultClinical_Inpatient-Mental-Health.pdf
- Prochaska, J. O., Norcross, J. C., & DiClemente, C. C. (1994). Changing for good: The revolutionary program that explains the six stages of change and teaches you how to free yourself from bad habits. Morrow.
- Rogers, R., Robinson, E. V., & Jackson, R. L. (2016). Forensic psychiatry and forensic psychology: Malingering and related response styles. In J. Payne-James & R. W. Byard (Eds.), Encyclopedia of forensic and legal medicine (2nd ed.) (pp. 627–633). Elsevier.
- Satici, B., Saricali, M., Satici, S. A., & Griffiths, M. D. (in press). Intolerance of uncertainty and mental wellbeing: Serial mediation by rumination and fear of COVID-19. International Journal of Mental Health and Addiction.
- Schröder, A., Vulink, N., & Denys, S. (2013). Misophonia: Diagnostic criteria for a new psychiatric disorder. PLoS ONE, 8(1).
Let us know your thoughts
Read other articles by their category
- Body & Brain (49)
- Coaching & Application (57)
- Compassion (26)
- Counseling (51)
- Emotional Intelligence (24)
- Gratitude (18)
- Grief & Bereavement (21)
- Happiness & SWB (40)
- Meaning & Values (26)
- Meditation (20)
- Mindfulness (45)
- Motivation & Goals (45)
- Optimism & Mindset (34)
- Positive CBT (28)
- Positive Communication (20)
- Positive Education (47)
- Positive Emotions (32)
- Positive Leadership (18)
- Positive Parenting (4)
- Positive Psychology (33)
- Positive Workplace (37)
- Productivity (17)
- Relationships (46)
- Resilience & Coping (36)
- Self Awareness (21)
- Self Esteem (38)
- Strengths & Virtues (32)
- Stress & Burnout Prevention (34)
- Theory & Books (46)
- Therapy Exercises (37)
- Types of Therapy (64)





What our readers think
Need a professional mental evaluation with MRI for my son who was born with mental disability.
Hi Gisela,
You can find a directory of licensed therapists here (and note that you can change the country setting in the top-right corner). You’ll also find there are a range of filters to help you drill down to the type of support you need: https://www.psychologytoday.com/us/therapists
I hope this helps.
– Nicole | Community Manager
Hi Nicole,
Thank you for sharing your experience and knowledge with us. Love your resources and they are definitely will be utalised to make a difference in many who are needing care and support in improving their mental health well-being. All the best with your ongoing research. Take care and stay safe.