20 Best Anxiety Tools for Helping Your Clients Cope
 Anxiety is part of our brain’s hardwired threat response, which has helped humans survive for thousands of years.
Anxiety is part of our brain’s hardwired threat response, which has helped humans survive for thousands of years.
We have all experienced anxiety at some point, whether it’s hearing a bump in the night or preparing for an exam.
However, over-activation of the anxiety response can have a debilitating impact, and anxiety difficulties are one of the most commonly presented mental health problems (Stansfeld et al., 2016). Thankfully, there are many evidence-based anxiety management tools available.
This article provides key information for practitioners, with over 20 helpful anxiety tools to help clients cope with and overcome anxiety difficulties.
Before you continue, we thought you might like to download our three Resilience Exercises for free. These engaging, science-based exercises will help you effectively deal with difficult circumstances and give you the tools to improve the resilience of your clients, students, or employees.
This Article Contains:
- What Is Anxiety According to Psychology?
- How to Cope With Anxiety and Worries
- 10 Effective Anxiety Management Tools
- 5 Helpful Grounding Tools for Adults
- A Look at Calming Breathing Techniques
- 5 Anxiety Tools for Supporting Youth
- How to Measure Anxiety in Therapy
- 6 Screening and Assessment Tools
- Resources From PositivePsychology.com
- A Take-Home Message
- References
What Is Anxiety According to Psychology?
Anxiety is a normal and adaptive emotional response, defined as feelings of distress, worry, and physiological symptoms in the context of apprehensively anticipating future danger or misfortune (American Psychological Association, 2013).
Anxiety is the activation of the body’s fight, flight, or freeze response, which is often experienced as restlessness, trembling, poor concentration, sweating, heart palpitations, shortness of breath, and irritability (Clark & Beck, 2011).
Although anxiety is a normal experience, it can become a problem when it exceeds the reality of potential danger. This can lead to excessive fear, hypersensitivity to threat, and unhelpful behavior change that impacts daily functioning (Clark & Beck, 2011).
Medical professionals can categorize these difficulties as anxiety disorders, such as panic disorder and generalized anxiety disorder (American Psychological Association, 2013).
Beck, Emery, and Greenberg’s (2005) cognitive theory suggests that anxiety difficulties stem from an overestimation of danger and underestimation of coping ability. In this theory, negative cognitions (e.g., predictions and appraisals) start the vicious cycle of anxiety, triggering associated physiological responses and safety behaviors (e.g., avoiding or escaping feared situations).
Although safety behaviors alleviate anxiety in the short term, they can lead to anxious predictions never being challenged, which maintains or worsens anxiety in the long term (Wells, 1997).
This brief TED Talk video introduces anxiety and the fight, flight, or freeze response.
How to Cope with Anxiety and Worries
Here are four steps for helping your clients cope with anxiety.
1. Psychoeducation
It is important to normalize anxiety initially and provide information about the brain’s threat response (Donker, Griffiths, Cuijpers, & Christensen, 2009).
Normalizing anxiety helps to reduce a client’s sense of shame or feeling that there’s something wrong with them (Welford, 2010). Here’s an example of an anxiety psychoeducation video.
For further reading about psychoeducation, this article explains how to provide Psychoeducation in Groups, while our article Coaching for Anxiety offers podcasts and techniques that you can use with your clients.
2. Anxiety monitoring
Keeping track of experiences of anxiety can help clients identify patterns of thoughts, feelings, and behaviors. They can write down triggers or keep an anxiety diary as a way to gain a deeper understanding of these patterns (Leahy, Holland, & McGinn, 2011).
3. Understanding maintenance cycles
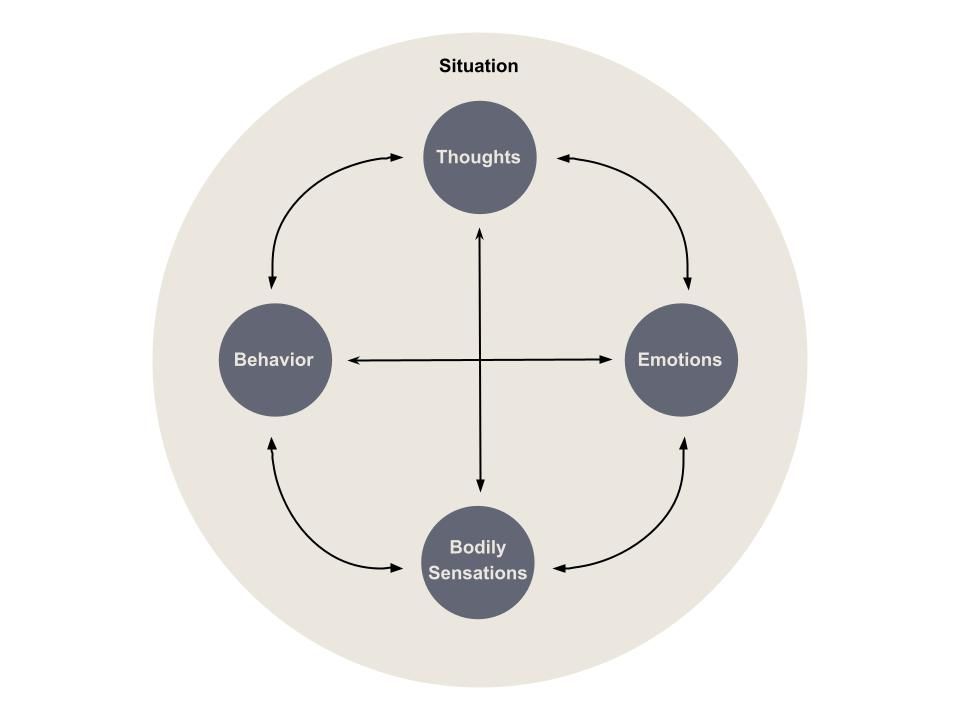
Psychological formulation (Johnstone & Dallos, 2014) can help clients understand maintenance cycles of anxiety (i.e., how their anxious thoughts, feelings, and behaviors interlink to keep anxiety going). For example, the Cognitive-Behavioral Therapy situational formulation cycle can be used as part of psychoeducation.
4. Building a toolkit of strategies
There are different types of tools that target different areas of the anxiety cycle.
Relaxation strategies calm bodily sensations, cognitive skills aim to shift anxious thinking, and behavioral strategies help to reduce safety behaviors.
Different tools work for different people in different situations. It can be helpful for clients to develop a written list or toolkit of strategies that work for them.
10 Effective Anxiety Management Tools
Here are 10 evidence-based anxiety management tools (adapted from Leahy et al., 2011; Westbrook, Kennerley, & Kirk, 2011; Kennerley, 2014).
1. Controlled breathing
Controlled breathing aims to reduce physiological symptoms of anxiety by regulating breathing. Controlled breathing involves breathing deeply into your lower abdomen for four counts and out for six counts, repeating for at least a few minutes.
2. Progressive muscle relaxation
Progressive muscle relaxation aims to relax the muscles to ease the bodily sensations of anxiety, such as muscle tension. You tense and relax each muscle group in turn, working progressively throughout the body.
3. Calming imagery
Visualization is the idea of building an image in your mind of a calm, safe place (e.g., beach, forest, familiar place). This soothes the anxiety response and distracts from anxious thinking (Hart, 2008; Welford, 2010).
4. Distraction
You can distract your brain from anxious thoughts by refocusing on another activity. This strategy can also help clients feel empowered to use their existing strengths and interests as helpful anxiety tools, for example, doing an enjoyable hobby.
5. Thought challenging
Thought challenging involves identifying evidence for and against anxious thoughts. The aim is to weigh up this evidence and then reframe the thought as a more balanced view of the situation, moving away from anxious predictions. Use this Questions for Thought Challenging worksheet to get a balanced view on a situation.
6. Compassionate self-talk
Anxiety partly stems from self-criticism, such as believing that you do not have the skills to cope (Welford, 2010).
Compassionate self-talk can help reduce anxiety and self-criticism. For example, “I’ve coped before, I can get through this.”
7. Worry time
This involves allocating specific worry time (e.g., 5–10 minutes per day). If worries pop up, these can be written down and saved until worry time. This reduces the amount of worrying and rumination. Use our Worry Bank worksheet for further practical guidance on this tool.
8. Behavioral experiments and graded exposure
These involve facing your fears by reducing safety behaviors. Behavioral experiments involve writing down the initial anxious prediction, facing the feared situation, and then reflecting on what actually happened.
This often provides evidence against the initial anxious belief. Use this Behavioral Experiment to Test Beliefs worksheet to plan out experiments. Build up to facing fears through graded exposure by breaking down the task into small steps.
This video animation explains how to build a graded exposure ladder.
9. Exercise
Physical activity can be an effective way to reduce anxiety levels. It helps burn off the adrenaline caused by the fight, flight, or freeze response and serves as a distraction (Kennerley, 2014) and also helps with sleep (Kredlow, Capozzoli, Hearon, Calkins, & Otto, 2015).
10. Sleep
Feeling anxious can negatively impact sleep, and lack of sleep can mean a lower threshold for feeling anxious. It is important to strive for a good night’s sleep, through a relaxing bedtime routine, regular sleep pattern, and using other sleep hygiene strategies.
5 Helpful Grounding Tools for Adults

The following grounding strategies are drawn from Mindfulness-Based Cognitive Therapy (Hofmann & Gómez, 2017) and trauma-focused interventions (Peckham, 2021).
- Mindful breathing
This involves bringing your attention to your breathing, which refocuses your brain away from anxious thoughts to solely attending to the present moment and the physical sensations of the breath. - 5-4-3-2-1
This strategy helps you to connect to your environment using all senses. It involves naming five things you can see, four things you can touch, three things you can hear, two things you can smell, and one thing you can taste. - Grounding object
It can be helpful to carry a grounding object, such as a stone or fidget toy. When anxious, you can hold the object and focus your attention on it, such as the textures and colors, to bring your attention back to the present. - Ground through the feet
Place your feet on the ground and focus on the sensations this connection brings. This simple tool aims to foster a sense of feeling centered, present, and grounded to the earth. - Body scan
Bring your awareness to each part of your body in turn. The aim is to notice different sensations in your body, either internally or how the body feels when in contact with the external environment (e.g., touching a chair).
How to practice grounding for anxiety relief
Tip 1: Start with mindful breathing
Focusing on the breath can help to anchor you initially and lay the foundations for other grounding skills.
Tip 2: Create a grounding box
Also called a self-soothe box, this pre-made collection of grounding objects and reminders can make it easier to use grounding strategies when you’re very anxious. It helps to have multi-sensory tools, for example, a grounding object or something pleasant to smell/taste. You can also have written reminders of other grounding skills.
Tip 3: Be kind to yourself
It is normal for your mind to wander during mindfulness and grounding techniques, and it is important not to fall into self-critical thinking.
We can use the mindfulness concepts of nonjudgmentally noticing when our mind wanders and refocusing back to the grounding exercise. It may help to use a cognitive defusion tool (Harris, 2009), such as seeing thoughts as leaves on a stream floating by while doing mindful grounding. You can access the Leaves on a Stream exercise as part of this free Mindfulness Tools pack.
A Look at Calming Breathing Techniques
Now that we’ve introduced how to do breathing techniques, let us explain why they work from a biological and psychological perspective.
Biological changes
Fast, shallow breathing (associated with anxiety) can result in hyperventilation, which disrupts the blood’s oxygen and carbon dioxide levels, leading to feeling faint and dizzy.
Self-regulation of breathing helps to calm these fight, flight, or freeze physiological anxiety symptoms (Jerath, Crawford, Barnes, & Harden, 2015), by allowing oxygen levels to return to normal (Hazlett-Stevens & Craske, 2004).
Cognitive distraction and grounding
Mindful breathing helps with the cognitive effects of anxiety. Instead of focusing on anxious thoughts, the mind focuses on the breath, helping to ground in the present and shift focus away from anxious thoughts about the past or future.
Self-soothing and self-compassion
Focusing on the breath is core to compassion-focused strategies, such as soothing rhythm breathing (Gilbert, 2009). This involves finding a breath rhythm that helps to self-soothe when feeling anxious (Welford, 2010), with a focus on using self-compassion if your mind wanders from the task. This helps to foster skills in both self-soothing and self-compassion.
5 Anxiety Tools for Supporting Youth
The anxiety tools above are also effective for children. The key is to ensure that they are adapted for age and developmental stage, such as by using different creative formats like worksheets, videos, and apps.
Example ideas include our Deep Breathing for Kids worksheet, as well as this anxiety psychoeducation video for kids.
When supporting children with anxiety, parents and carers play a vital role. Here are five additional anxiety management tools for parents/carers to implement (Creswell & Willetts, 2019):
1. Manage parents’ role in safety behaviors
Sometimes parents can unintentionally feed into children’s safety behaviors. It is understandable that parents don’t want to see a child in distress; however, it is important not to fall into the traps of safety behaviors such as avoidance, which can make a child’s anxiety worse in the long term (Wells, 1997).
Parents can use tools such as graded exposure and set goals with their children to reduce safety behaviors.
2. Manage reassurance-seeking behavior
Children often seek reassurance from adults when feeling anxious. Although parents will naturally want to ensure the child is okay, too much reassurance can actually make anxiety worse in the long term (Creswell & Willetts, 2019).
Instead of giving reassurance, it can help to empower the child to manage their anxiety by using strategies from their toolbox.
3. Model positive anxiety management
Children observe adults’ behavior to learn what to be afraid of and how to cope. Parents can try to model to children how they positively manage day-to-day anxiety themselves.
4. Talk time
Parents can allocate a specific time to discuss worries with children. This helps to reduce the amount of focus on worries and reassurance seeking, making them less dominant in day-to-day life.
5. Encourage independence
Parents can help children overcome anxiety by empowering them to manage and problem-solve anxiety-provoking situations themselves, to help build independent coping skills.
It is also important to reinforce positive and brave behaviors using praise and rewards.
How to Measure Anxiety in Therapy
- Creating a 0–10 anxiety scale can help the client measure and log anxiety intensity between therapy sessions, as well as categorize anxiety levels in different situations (Westbrook et al., 2011).
- Anxiety diaries can be a helpful way for clients to keep a record of anxious thoughts, feelings, and behavior, and to monitor change over time (Kennerley, 2014; Westbrook et al., 2011).
- Goal-based outcomes (Law & Jacob, 2013) are therapeutic measures where clients set goals around anxiety and then rate themselves weekly on a scale from 1 to 10 on how close they are to reaching those goals.
- Validated questionnaires for anxiety (see below).
6 Screening and Assessment Tools

Adults:
- General Anxiety Disorder questionnaire (Spitzer, Kroenke, Williams, & Löwe, 2006). This seven-item questionnaire can be found at PHQ Screeners.
- The Hospital Anxiety and Depression Scale (HADS) is commonly used by doctors and therapists to measure a client’s level of anxiety. Here is an online version.
- DASS, the Depression and Anxiety Stress Scale is a self-report instrument and also measures stress and tension, in addition to depression and anxiety. You can access the free version here, but have to purchase the manual.
Adults with intellectual disability:
- Glasgow Anxiety Scale for People with an Intellectual Disability (Mindham & Espie, 2003). This 27-item tool is included in Mindham and Espie’s (2003) original article.
Children:
- Revised Children’s Anxiety and Depression Scale (Chorpita, Yim, Moffitt, Umemoto, & Francis, 2000). Both child and parent versions can be downloaded from CORC.
- Spence Children’s Anxiety Scale (SCAS; Spence, 1997). This 45-item scale can be located on the SCAS website.
Resources From PositivePsychology.com
Here are some additional helpful anxiety worksheets for children:
- When I’m Scared
This worksheet helps parents speak to their children about their anxiety in a structured, age-appropriate way, exploring triggers, thoughts, and bodily sensations of anxiety. - Draw Your Fears
This worksheet allows a child space to explore their anxieties by drawing their worries. This is helpful, as some children experience anxious images, rather than words, in their mind. - My Body and My Worries
This worksheet explores bodily sensations associated with the fight, flight, or freeze response, helping children learn about normal anxiety signs.
17 Resilience & Coping Exercises
If you’re looking for more science-based ways to help others overcome adversity, this collection contains 17 validated resilience and coping exercises. Use them to help others recover from personal challenges and turn setbacks into opportunities for growth.
A Take-Home Message
Anxiety is a normal hard-wired threat response that our brain uses when it perceives danger. However, our brain can sometimes take a “better safe than sorry” approach by overestimating danger, which results in our fight, flight, or freeze response being triggered too often. This is when anxiety can become problematic and when therapeutic intervention may be recommended.
There is a range of evidence-based therapies and anxiety management strategies that therapists can use to support clients. The key message is not to strive for the impossible task of getting rid of anxiety, but rather to build strategies to manage it successfully.
The aim of this article was to give practitioners a summary of the key advice and strategies available for anxiety management. The hope is that this can be used to foster clients’ confidence to use their inherent strengths and build new skills in order to overcome anxiety difficulties and live the life they choose.
We hope you enjoyed reading this article. Don’t forget to download our three Resilience Exercises for free.
- American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders (5th ed.). Author.
- Baldwin, D. S., Anderson, I. M., Nutt, D. J., Allgulander, C., Bandelow, B., den Boer, J., … Wittchen, H.U. (2014). Evidence-based pharmacological treatment of anxiety disorders, post-traumatic stress disorder and obsessive-compulsive disorder: A revision of the 2005 guidelines from the British Association for Psychopharmacology. Journal of Psychopharmacology, 28, 403–439.
- Beck, A. T., Emery, G., & Greenberg, R. L. (2005). Anxiety disorders and phobias: a cognitive perspective. Basic Books.
- Beidas, R. S., Stewart, R. E., Walsh, L., Lucas, S., Downey, M. M., Jackson, K., … Mandell, D. S. (2015). Free, brief, and validated: Standardized instruments for low-resource mental health settings. Cognitive and Behavioral Practice, 22(1), 5–19.
- Clark, D. A., & Beck, A. T. (2011). Cognitive therapy of anxiety disorders: Science and practice. Guilford Press.
- Creswell, C., & Willetts, L. (2019). Helping your child with fears and worries: A self-help guide for parents (2nd ed.). Robinson.
- Chorpita, B. F., Yim, L. M., Moffitt, C. E., Umemoto, L. A., & Francis, S. E. (2000). Assessment of symptoms of DSM-IV anxiety and depression in children: A revised child anxiety and depression scale. Behaviour Research and Therapy, 38, 835–855.
- Donker, T., Griffiths, K. M., Cuijpers, P., & Christensen, H. (2009). Psychoeducation for depression, anxiety and psychological distress: A meta-analysis. BMC Medicine, 7(1), 1–9.
- Gilbert, P. (2009). The compassionate mind. Robinson.
- Harris, R. (2009). ACT made simple. New Harbinger.
- Hart, J. (2008). Guided imagery. Alternative and Complementary Therapies, 14(6), 295–299.
- Hazlett-Stevens, H., & Craske, M. G. (2004). Breathing retraining and diaphragmatic breathing techniques. In W. T. O’Donohue, J. E. Fisher, & S. C. Hayes (Eds.), Cognitive behavior therapy: Applying empirically supported techniques in your practice (pp. 59–64). John Wiley & Sons.
- Hofmann, S. G., & Gómez, A. F. (2017). Mindfulness-based interventions for anxiety and depression. Psychiatric Clinics, 40(4), 739–749.
- Jerath, R., Crawford, M. W., Barnes, V. A., & Harden, K. (2015). Self-regulation of breathing as a primary treatment for anxiety. Applied Psychophysiology and Biofeedback, 40(2), 107–115.
- Johnstone, L., & Dallos, R. (2014). Formulation in psychology and psychotherapy: Making sense of people’s problems (2nd ed.). Routledge.
- Kennerley, H. (2014). Overcoming childhood trauma: A self-help guide using cognitive behavioral techniques. Hachette.
- Kredlow, M. A., Capozzoli, M. C., Hearon, B. A., Calkins, A. W., & Otto, M. W. (2015). The effects of physical activity on sleep: A meta-analytic review. Journal of Behavioral Medicine, 38(3), 427–449.
- Law, D., & Jacob, J. (2013). Goals and goal based outcomes (GBOs). CAMHS Press.
- Leahy, R. L., Holland, S. J., & McGinn, L. K. (2011). Treatment plans and interventions for depression and anxiety disorders. Guilford Press.
- Mindham, J., & Espie, C. A. (2003). Glasgow Anxiety Scale for People with an Intellectual Disability (GASID): Development and psychometric properties of a new measure for use with people with mild intellectual disability. Journal of Intellectual Disability Research, 47(1), 22–30.
- Peckham, M. (2021). Self-care and grounding. In A. Hershler, L. Hughes, P. Nguyen, & S. Wall (Eds.), Looking at trauma: A tool kit for clinicians (Vol. 23) (pp. 13–20). Penn State University Press.
- Spence, S. H. (1997). Structure of anxiety symptoms among children: A confirmatory factor-analytic study. Journal of Abnormal Psychology, 106(2), 280–297.
- Spitzer, R. L., Kroenke, K., Williams, J. B., & Löwe, B. (2006). A brief measure for assessing generalized anxiety disorder: The GAD-7. Archives of Internal Medicine, 166(10), 1092–1097.
- Stansfeld, S., Clark, C., Bebbington, P. E., King, M., Jenkins, R., & Hinchliffe, S. (2016). Common mental disorders. In S. McManus, P. E. Bebbington, R. Jenkins, & T. Brugha (Eds.), Mental health and wellbeing in England: Adult psychiatric morbidity survey 2014 (pp. 37–68). NHS Digital.
- Welford, M. (2010). A compassion focused approach to anxiety disorders. International Journal of Cognitive Therapy, 3(2), 124–140.
- Wells, A. (1997). Cognitive therapy of anxiety disorders: A practice manual and conceptual guide. John Wiley & Sons.
- Westbrook, D., Kennerley, H., & Kirk, J. (2011). An introduction to cognitive behaviour therapy: Skills and applications. SAGE.
Let us know your thoughts
Read other articles by their category
- Body & Brain (49)
- Coaching & Application (57)
- Compassion (26)
- Counseling (51)
- Emotional Intelligence (24)
- Gratitude (18)
- Grief & Bereavement (21)
- Happiness & SWB (40)
- Meaning & Values (26)
- Meditation (20)
- Mindfulness (45)
- Motivation & Goals (45)
- Optimism & Mindset (34)
- Positive CBT (29)
- Positive Communication (20)
- Positive Education (47)
- Positive Emotions (32)
- Positive Leadership (18)
- Positive Parenting (4)
- Positive Psychology (33)
- Positive Workplace (37)
- Productivity (17)
- Relationships (46)
- Resilience & Coping (36)
- Self Awareness (21)
- Self Esteem (38)
- Strengths & Virtues (32)
- Stress & Burnout Prevention (34)
- Theory & Books (46)
- Therapy Exercises (37)
- Types of Therapy (64)





What our readers think
Thanks for sharing this post.
Very useful article, many thanks
hi
I started feeling anxiety and worries as my retirement is due is year.
Kindly help me to lessen anxiety and manage stress. I am 62.
thanks
WAHID HASHMI
Hi Wahid,
I’m sorry to read you’re feeling anxiety about your approaching retirement. I’m sure it’s a time of significant change for you. I’ll note that this comment section is no substitute for the support of a professional therapist or counsellor who is trained in the appropriate methods to support you. You can find a directory of licensed therapists here (and note that you can change the country setting in the top-right corner).
For some reading you can look through on your own (or with support), I’d suggest some of the following posts in our blog, which include downloadable worksheets and reflections you can use:
Workplace Stress Management: 11 Best Strategies & Worksheets – https://positivepsychology.com/workplace-stress-management/
16 Stress-Management Activities and Worksheets to Help Clients Beat Stress – https://positivepsychology.com/stress-management-activities-worksheets/
I hope this helps a little, and I wish you all the best.
– Nicole | Community Manager