Exploring the Mind–Body Connection Through Research
 The debate about the mind–body connection has been around for millennia.
The debate about the mind–body connection has been around for millennia.
From ancient philosophers and religions to modern science, there have been different views on whether the mind and the body are related, if they can affect each other, and how that interaction can be possible.
Although mainstream contemporary science and healthcare practices tend to study and treat the mind and the body as separate entities, increasing research and evidence-based practices support the notion of a bidirectional relationship between the two.
This suggests that we might benefit more from acknowledging these interactions and adopting a more holistic approach to our health and wellbeing.
Before you continue, we thought you might like to download our three Positive Psychology Exercises for free. These science-based exercises will explore fundamental aspects of positive psychology including strengths, values, and self-compassion and will give you the tools to enhance the wellbeing of your clients, students, or employees.
This Article Contains:
- Mind–Body Connection: A Philosophical Take
- Psychology Theories on Mind–Body Interaction
- 2 Examples of the Mind–Body Connection
- Can the Mind Heal the Body? 3 Research Areas
- 10 Empirical Ways to Heal Your Mind Through Your Body
- A Look at the Mechanisms of Mind–Body Therapy
- A Take-Home Message
- References
Mind–Body Connection: A Philosophical Take
Throughout centuries, philosophers and scientists have hypothesized about the mind–body connection. However, far from reaching a definite solution, we have been left with what many refer to as the mind–body problem.
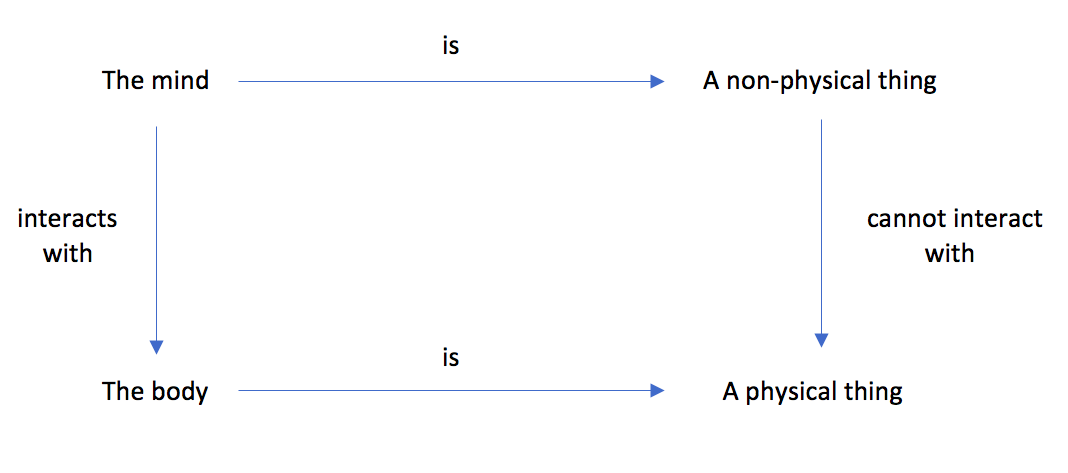
According to Westphal (2016), this is a logical problem with four statements about the nature and interaction of mind and body.
While considered to be true in isolation, they contradict each other when brought together, as illustrated below:
Figure 1. Illustration of the Mind–Body Problem. Adapted from “The Mind–Body Problem” by Westphal (2016). Copyright 2016 Massachusetts Institute of Technology.
Two main approaches within the philosophy of mind theorize about the mind–body connection by placing their attention in some of the statements above.
Monism
This approach posits that there is only one reality, composed only of either physical or non-physical substances (Kind, 2020).
Physicalism
This view assumes that everything existing is physical, including the mind. Here, the mind–body interaction is acknowledged only in the physical plane.
This is often related to traditional science, which tends to explain mental phenomena in terms of brain activities.
Idealism
Using a metaphysical perspective, this standpoint sustains that reality is non-physical, and everything is either a mind or depends on the mind to exist.
In other words, this view proposes that reality depends on how our minds perceive and make sense of the world.
Dualism
This philosophical standpoint theorizes that reality is composed of both physical and non-physical substances. Dualism posits that the body is physical, while the mind is not, treating mind and body as separate entities.
This worldview was developed by Rene Descartes during the 16th century, widely influencing modern science and compartmentalizing the study of body and mind (Descartes, 1960).
Dualism has evolved from views proposing that mind and body exist independently from one another without interaction, to ones that acknowledge a causal relationship between both.
According to Kind (2020), current views tend to be either interactionist property dualists or physicalists.
While physicalists would assert that the mind can be completely understood in terms of brain and neural networks, interactionist dualists would state that mental activities are rooted in the physical brain, yet are not reducible to these material properties (Westphal, 2016).
Non-dualism: Beyond the mind–body problem
This philosophical approach is often linked to several Eastern traditions and might provide further insight into the mind–body problem from a different angle.
Non-dualism proposes that the dualistic nature of things, such as mind/body, is an illusion.
Thus, there is no real separation between mind and body, as they are interdependent and need each other to exist (Loy, 1997).
Watch this short animated video by Embodied Philosophy to learn more about these approaches:
Interesting debate, but why and how is all this philosophical discussion relevant to mind–body research?
Although philosophy and empirical science may seem like independent silos, philosophy of mind is highly relevant to science and psychology in particular, as it informs the underlying assumptions and methods by which scientists conduct research and contribute to our understanding of mind–body interactions.
Psychology Theories on Mind–Body Interaction

Behaviorists may hold a physicalist view, conceiving of the mind in terms of observable behavior expressed in or with the body.
While cognitivism acknowledges the body’s role, it tends to focus more on mental phenomena, reflecting a tendency towards dualism.
Finally, embodied approaches in psychology place equal value on the role of each, acknowledging their mutual interaction and adopting a more holistic view (Leitan & Murray, 2014).
Theories on emotions
These theories have evolved from considering emotions purely as physiological reactions to subjective interpretations to which we assign a valence depending on how they feel.
Cognitive appraisal theories
Pioneered by Magda Arnold and Richard Lazarus in the 1940s and 1950s respectively, the cognitive appraisal approach proposes that emotions result from the cognitive evaluation of an event in terms of their consequence as being pleasant or unpleasant (Shields & Kappas, 2006).
This is the background behind the use of the terms positive and negative emotions. Until the late 1990s, research on negative emotions broadly outnumbered studies on positive emotions, in part due to the perceived impact and relevance of negative emotions.
Broaden-and-build theory
Barbara Fredrickson (2000) posits that positive and negative affect complement each other and have the purpose of promoting the survival of the human species.
While negative emotions narrow our thought–action repertoire to respond more effectively to a threat, positive emotions expand this repertoire to build personal resources and pro-social behavior.
Remarkably, the broaden-and-build theory also states that “positive emotions have an undoing effect on negative emotions” (Fredrickson, 2000, p. 1).
Recent research in neuroscience has further supported this theory, suggesting that mindfulness and loving-kindness meditation can foster positive emotions and buffer against negative affect in a clinical population (Garland et al., 2010).
Cognitive theories
Although cognitive theories acknowledge the relationship between the mind (thoughts and subjective experiences of emotions) and the body (physical responses and behavior), they tend to place greater emphasis on the mental realm (Leitan & Murray, 2014).
This can be reflected in the lack of integration of the body within psychological interventions and psychotherapy (Hefferon, 2013).
Cognitive theory of psychopathology
Aaron Beck developed this model in the 1960s, contending that negative cognitions elicit unpleasant emotions, physical symptoms, and dysfunctional behavior.
He argues that these types of thoughts are the leading cause of depression, and therefore, psychotherapy should be aimed at addressing these mental processes to create positive change (Leitan & Murray, 2014).
Growth mindset theory
People with a growth mindset see challenges as opportunities to learn and grow, using their effort as a pathway to achieve mastery (Nussbaum & Dweck, 2008).
This involves mental processes grounded in the brain, such as increased awareness, attention, and the ability to adapt behavior to attain goals related to intrinsic motivation.
This framework is consistent with neuroplasticity, arguing that brain structures can reorganize, develop, and change according to our learning experiences (Ng, 2018).
Embodiment theories
This group of theories puts forward that bodily states and processes affect our psychological sphere and vice versa, contrasting with the disembodied view of the mind proposed by Descartes and early cognitivists.
Embodiment posits that our bodies mediate our interaction with the world and that mental symbols must be grounded in forms, such as words (Glenberg, 2010).
Embodied emotions
Considering previous theories on emotions, Prinz (2004) argues that although emotions are physical, they are essentially semantic too.
In other words, emotions can be conscious or unconscious perceptions of the body’s variations, but they are always grounded in language to an equal extent.
Embodied cognition (EC)
EC approaches generally agree that the type of body an organism has (e.g., human body) determines and shapes their perceptual and motor processes.
This means that the mind is grounded in the sensorimotor system, and that mind and body are equally relevant.
So rather than seeing the body as a server of the mind, EC posits that the body is actively and subjectively engaged in cognition (Leitan & Murray, 2014).
Embodiment theories allow bringing mind and body together into neuroscientific research, considering both participants’ subjective and physical experiences (Borghi & Caruana, 2015).
For example, a recent review of Beck’s Cognitive Theory considers neural and cognitive pathways to explain the effectiveness of Cognitive Therapy.
Research findings support the relationship between Cognitive Therapy and brain areas involved in initiating negative emotions and their cognitive control (Clark & Beck, 2010).
2 Examples of the Mind–Body Connection
To support the psychology theories of mind-body interaction, we look at two examples.
The mind–body connection of trauma
The polyvagal theory describes and explains different mechanisms of neural regulation and their related behaviors when perceiving a threat, involving the brain cortex, immune response, hypothalamic-pituitary-adrenal, and gut-brain axes (Porges, 2001).
The chain reaction activated under these circumstances is called the defense cascade, comprising four different responses (Kozlowska, Walker, McLean, & Carrive, 2015):
- Arousal. Cardiac regulation response promotes either engagement or disengagement with the environment after perceiving a threat.
- Fight-or-flight response. The inhibition of the vagus nerve and the sympathetic nervous system’s activation lead to an increase in metabolic activity to mobilize the body to either escape or confront the threat.
- Freeze response. When facing an unavoidable threat, the vagus nerve is stimulated, the metabolic activity drops, and the body freezes.
- Quiescent immobility. After the threat is gone, the parasympathetic system overrides, and metabolic activity drops dramatically so the body can rest and heal.
Understanding the pattern of these responses can help us understand and heal trauma (Kozlowska et al., 2015).
Porges (2001) argues that the traumatic experience leaves an imprint in the body, getting stuck in a trauma-response mode.
Mind–body interventions can help people to release these imprints.
The mind–body connection of emotions and immunity
Research supports a strong relationship between affective states and immune system response.
Sustained negative emotional states such as stress, depression, and anxiety can worsen immunity functions and affect other bodily functions.
Recent studies show that positive emotions are associated with a range of health outcomes, such as reducing ill-health symptoms, reducing pain, and increasing longevity.
In terms of immunity and illness, positive emotions have been related to enhanced immunity outcomes in immune-depressive conditions, such as cancer and HIV, and also in the nonclinical population after being exposed to the flu virus (Pressman & Black, 2012).
But how is this possible? One possible pathway is that positive emotions buffer the stress response in the body and its consequences. This aligns with the undoing effect posited by the broaden-and-build theory.
Other pathways suggest that positive emotions promote social bonds and changes in lifestyle habits, such as clean eating, sleeping, and regular exercise, thus improving immunity (Pressman & Cohen, 2005).
Can the Mind Heal the Body? 3 Research Areas

Meditation
A study exploring the effects of meditation on the brain compared novices to experienced meditators.
Functional MRI showed that experienced meditators had more brain activity in areas related to attention and inhibition response and less activation in regions related to discursive emotions and cognitions, suggesting a correlation between hours of practice and brain plasticity (Brefczynski-Lewis, Lutz, Schaefer, Levinson, & Davidson, 2007).
Loving-kindness meditation (LKM) is a type of meditation derived from Buddhist traditions, aiming at cultivating unconditional love and kindness for yourself and others, as well as compassion, joy, and equanimity.
A systematic review suggests that LKM is an effective intervention for increasing positive emotions and reducing pain (Zeng, Chiu, Wang, Oei, and Leung, 2015).
Mindfulness-based psychotherapy
Mindfulness can be used as a therapeutic tool to develop awareness and acceptance of feelings, thoughts, and bodily sensations, aligning to psychotherapy goals such as reducing ruminating thoughts or developing self-acceptance.
Applications linking the mind and the body can include mindful breathing and body scan exercises (Leitan & Murray, 2014).
A systematic review with meta-analysis found that mindfulness can help with depression, pain, weight management, schizophrenia, smoking, and anxiety (Goldberg et al., 2018).
Another study showed that a mindfulness program positively affects immunity and brain functions (Davidson et al., 2003).
Hypnotherapy
The American Psychological Association (2020) defines hypnosis as a therapeutic method used in clinical settings, where the client is induced into a state of relaxation by following suggestions from their psychotherapist.
It is hypothesized that in a relaxed state, the subconscious mind can more readily accept suggestions to change involuntary responses.
Clinical research evidence suggests that hypnosis can be useful for physical ailments such as managing pain and improving anxiety and depression.
One type of hypnosis is Gut-Directed Hypnotherapy, which has shown to effectively reduce irritable bowel syndrome symptoms and increase wellbeing (Peter et al., 2018).
10 Empirical Ways to Heal Your Mind Through Your Body
Below are listed ten approaches believed to heal and improve the body and thereby heal and improve the mind.
1. Body psychotherapy
The body can be integrated as a central tool in psychotherapy by connecting bodily experiences to emotional and subjective experiences.
Body psychotherapy mainly uses body awareness of external and internal bodily sensations to accept and re-frame their meaning.
These mental health interventions can be beneficial not only for healing from trauma but also for wellbeing (Hefferon, 2013).
2. Exercise psychotherapy
Exercise can be used as a means to achieve psychotherapeutic goals, acknowledging that blending psychological and physical strategies can be more effective than using a standalone treatment.
This might include improving energy levels in clients with depression, reducing anxiety, or improving mastery and self-efficacy (Hefferon, 2013).
3. Somatic Experiencing (SE®)
SE® was developed by Dr. Peter Levine to regulate interrupted neuromuscular patterns due to trauma.
It consists of bringing awareness to physical sensations and reactions associated with a traumatic experience, helping clients describe physical patterns to integrate unconscious memories consciously.
Although there is limited empirical research, a systematic review including four studies on SE® suggests its effectiveness in improving post-traumatic stress disorder (PTSD) symptoms (Almeida, Gomez de Melo, & Cordeiro de Sousa, 2019).
4. Tension and trauma releasing exercises
Recently renamed as Self-induced Unclassified Therapeutic Tremor (SUTT), this method uses physical exercises to evoke natural tremor responses in the body to release tension associated with stress or trauma (Berceli, Salmon, Bonifas, & Ndefo, 2014).
Proposed by Dr. David Berceli, SUTT argues that although neuromuscular tremors are an innate response to events perceived as threatening, humans have learned to suppress them.
A pilot study (Berceli, et al. 2014) and a case study (Heath & Beattie, 2019) report that people experienced increased wellbeing and decreased stress at post-intervention measurements and follow-up.
5. Yoga
Yoga is considered an ancient Eastern discipline integrating mind, body, and spirit through practices, typically including physical postures, breathing techniques, and meditation.
Yoga Chikitsa, or Yoga Therapy, refers to the use of yoga for improving ill-health conditions.
From a Western perspective, yoga has been used as an add-on therapy for improving symptoms of depression (Cramer, Lauche, Langhorst, & Dobos, 2013), anxiety (Cramer et al., 2018), PTSD (Nguyen-Feng, Clark, & Butler 2019), cancer (Cramer, Lange, Klose, Paul, & Dobos, 2012), and schizophrenia (Vancampfort et al., 2012).
Yoga benefits also relate to health and wellbeing outcomes in the general population (Hendriks, de Jong, & Cramer, 2017).
6. Dance therapy
Dance Movement Therapy (DMT) refers to “the therapeutic use of movement aiming to further the emotional cognitive, physical, spiritual and social integration of the individual” (European Association of Dance Movement Therapy, 2020, paragraph 1).
DMT seeks to understand and create new meanings from patterns of behavior by recognizing and exploring sensations, emotions, and stories emerging from the movement.
It is facilitated by a registered therapist, and it can be done individually or in a group setting (European Association of Dance Movement Therapy, 2020).
Studies suggest dance therapy‘s effectiveness in improving ill health and trauma in clients with schizophrenia (Xia & Grant, 2009) and cancer (Bradt, Shim, & Goodill, 2015).
7. Progressive muscle relaxation (PMR)
Initially developed by Edmund Jacobson in the 1920s, PMR seeks to decrease anxiety levels by gradually contracting and relaxing muscle groups to reduce physical tension and physiological activation (Hefferon, 2013).
A systematic review with meta-analysis of relaxation intervention including 10 studies on PMR suggests this can be an efficacious treatment for anxiety in different clinical settings (Manzoni, Pagnini, Castelnuovo, & Molinari, 2008).
8. Deep breathing
Intentional breath regulation to increase pulmonary capacity while reducing the rate of breathing cycles has been acknowledged as an effective method to improve both physical and mental health.
By consciously engaging the diaphragm, the practice of slow-paced deep breathing activates the parasympathetic nervous system and inhibits the sympathetic nervous system, invoking a relaxation response and decreasing stress (Saoji, Raghavendra, & Manjunath, 2019).
Studies show that deep-breathing exercises can lower depressive and anxiety symptoms (Jerath, Crawford, Barnes, & Harden, 2015) and foster emotional wellbeing (Zaccaro et al., 2018).
9. Qigong and tai chi
Sharing the same philosophical roots, tai chi and qigong focus on the cultivation and enhancement of qi or life energy.
Along with yoga, they are considered meditative movement practices, and they include slow-paced and flow-like physical movements, as well as sitting, standing, or movement meditation; body shaking; and breathing techniques.
Underpinned by traditional Chinese medicine, they suggest that combining self-awareness with movement, meditation, and breath can promote mind–body balance and self-healing (Jahnke, Larkey, Rogers, Etnier, & Lin, 2010).
Several reviews have explored the effects of tai chi and qigong on different ill-health conditions such as cancer (Lee, Chen, Sancier, & Ernst, 2007), hypertension (Lee, Pittler, Guo, & Ernst, 2007), and cardiovascular disease (Lee, Pittler, Taylor-Piliae, & Ernst, 2007).
A Look at the Mechanisms of Mind–Body Therapy
Mind–body Therapy (MBT) is an umbrella term for therapeutic approaches combining physical and mental elements, such as those mentioned above.
MBT has been gradually recognized as an effective add-on treatment to traditional approaches for improving physical and mental health outcomes.
Research in the field of genomics has shed light on the relationship between gene expression and emotional states.
Similarly, studies in neuroimaging and neurophysiology have examined the connections and pathways between emotions and thoughts (Muehsam et al., 2017).
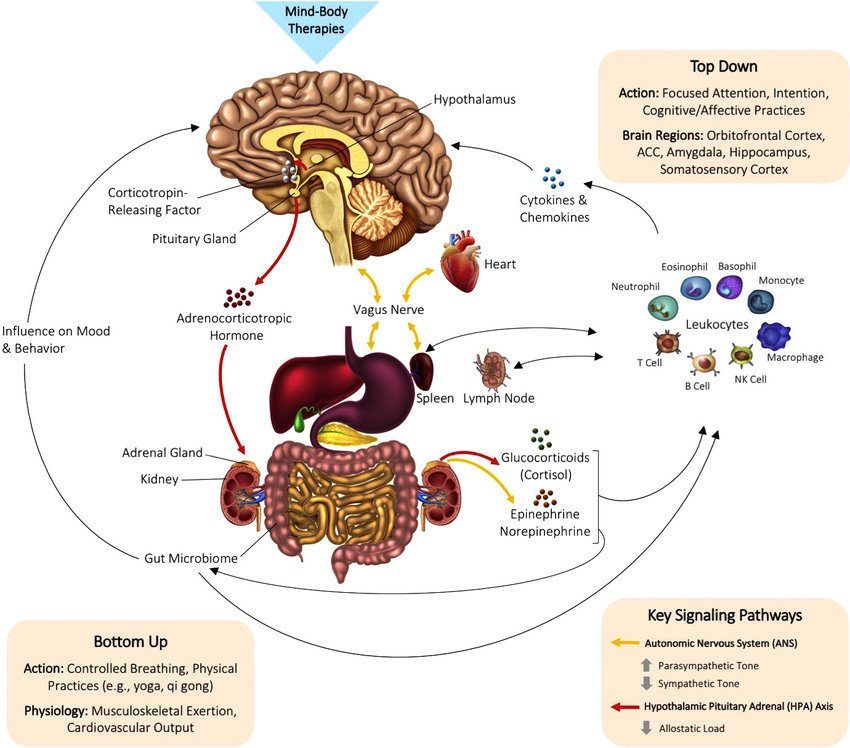
Figure 2. Biological Mechanisms of MBT. Extracted from “The embodied mind: a review on functional genomic and neurological correlates of mind-body therapies” by Muehsam, D., et al. (2017) Neuroscience & Biobehavioral Reviews, 73, p. 167. Copyright 2016 by Elsevier Ltd.
The diagram above illustrates how MBT works, including top-down and bottom-up pathways.
Top-down interventions like meditation or mindfulness focus on thoughts and emotions. Their neurological correlates in turn influence the endocrine and nervous system, with ulterior changes in the body.
Bottom-up interventions centered on breathing and physical movements such as yoga, tai chi, and qigong stimulate the nervous, immune, and endocrine systems, resulting in changes in psychological states.
A Take-Home Message
The mind–body connection is undeniable, yet our understanding of how they interact is still limited.
The dualistic view of modern science has provided many advances in the knowledge of each, though in an isolated way.
Contemporary research urges the need to take a holistic approach to explore the mind and body as an integrated entity and continue to explore the potential of MBT for alleviating disease and enhancing wellbeing.
We hope you enjoyed reading this article. Don’t forget to download our three Positive Psychology Exercises for free.
- Almeida, A. K., Gomez de Melo, S. C., & Cordeiro de Sousa, M. B. (2019). A systematic review of somatic intervention treatments in PTSD: Does Somatic Experiencing® (SE®) have the potential to be a suitable choice? Estudos de Psicologia, 24(3), 237–246.
- American Psychological Association. (2020). Hypnosis. Retrieved on August 2020 from https://www.apa.org/topics/hypnosis.
- Berceli, D., Salmon, M., Bonifas, R., & Ndefo, N. (2014). Effects of self-induced unclassified therapeutic tremors on quality of life among non-professional caregivers: A pilot study. Global Advances in Health and Medicine, 3(5), 45–48.
- Borghi, A.M., & Caruana, F. (2015). Embodiment theory. In: J.D. Wright (Ed.) International encyclopedia of the social & behavioral sciences, 2nd edition, Vol 6. (pp. 420–426). Oxford: Elsevier.
- Bradt, J., Shim, M., & Goodill, S. W. (2015). Dance/movement therapy for improving psychological and physical outcomes in cancer patients. Cochrane Database of Systematic Reviews, (1).
- Brefczynski-Lewis, J. A., Lutz, A., Schaefer, H. S., Levinson, D. B., & Davidson, R. J. (2007). Neural correlates of attentional expertise in long-term meditation practitioners. Proceedings of the National Academy of Sciences, 104(27), 11483–11488.
- Clark, D. A., & Beck, A. T. (2010). Cognitive theory and therapy for anxiety and depression: Convergence with neurobiological findings. International Journal of Psychophysiology, 14(9), 418–424.
- Cramer, H., Lauche, R., Anheyer, D., Pilkington, K., de Manincor, M., Dobos, G., & Ward, L. (2018). Yoga for anxiety: A systematic review and meta-analysis of randomized controlled trials. Depression and Anxiety, 35(9), 830–843.
- Cramer H., Lange, S., Klose, P., Paul, A., & Dobos, G. (2012). Yoga for breast cancer patients and survivors: A systematic review and meta-analysis. BMC Cancer, 12, 412–458.
- Cramer, H., Lauche, R., Langhorst, J., & Dobos, G. (2013). Yoga for depression: A systematic review and meta-analysis. Depression and Anxiety, 30, 1068–1983.
- Davidson, R. J., Kabat-Zinn, J., Schumacher, J., Rosenkranz, M., Muller, D., Santorelli, S. F., … & Sheridan, J. F. (2003). Alterations in brain and immune function produced by mindfulness meditation. Psychosomatic Medicine, 65(4), 564–570.
- Descartes, R. (1960). Meditations on First Philosophy 1st Edition.
- European Association of Dance Movement Therapy. (2020). What is dance movement therapy? Retrieved on August 2020 from https://www.eadmt.com/?action=article&id=22.
- Fredrickson, B. L. (2000). Cultivating positive emotions to optimize health and wellbeing. Prevention and Treatment, 3(0001a), 1–25.
- Garland, E. L., Fredrickson, B., Kring, A. M., Johnson, D. P., Meyer, P. S., & Penn, D. L. (2010). Upward spirals of positive emotions counter downward spirals of negativity: Insights from the broaden-and-build theory and affective neuroscience on the treatment of emotion dysfunctions and deficits in psychopathology. Clinical Psychology Review, 30(7), 849–864.
- Glenberg, A. M. (2010). Embodiment as a unifying perspective for psychology. Wiley Interdisciplinary Reviews: Cognitive Science, 1(4), 586–596.
- Goldberg, S. B., Tucker, R. P., Greene, P. A., Davidson, R. J., Wampold, B. E., Kearney, D. J., & Simpson, T. L. (2018). Mindfulness-based interventions for psychiatric disorders: A systematic review and meta-analysis. Clinical Psychology Review, 59, 52–60.
- Heath, R., & Beattie, J. (2019). Case report of a former soldier using TRE (tension/trauma releasing exercises) for post- traumatic stress disorder self-care. Journal of Military and Veterans’ Health, 27(3), 35–40.
- Hendriks, T., de Jong, J., & Cramer, H. (2017). The effects of yoga on positive mental health among healthy adults: A systematic review and meta-analysis. The Journal of Alternative and Complementary Medicine, 23(7), 505–517.
- Hefferon, K. (2013). Positive psychology and the body: The somatopsychic side to flourishing. London: McGraw-Hill Education.
- Jahnke, R., Larkey, L., Rogers, C. Etnier, J., & Lin, F. (2010). A comprehensive review of health benefits of qigong and tai chi. American Journal of Health Promotion, 24(6), 1–25.
- Jerath, R., Crawford, M. W., Barnes, V. A., & Harden, K. (2015). Self-regulation of breathing as a primary treatment for anxiety. Applications of Psychophysiological Feedback, 40, 107–115.
- Kind, A. (2020). Philosophy of mind: The basics. New York: Routledge.
- Kozlowska, K., Walker, P., McLean, L., & Carrive, P. (2015). Fear and the defense cascade: Clinical implications and management. Harvard Review of Psychiatry, 23(4), 263–287.
- Lee, M. S., Chen, K. W., Sancier, K. M., & Ernst, E. (2007) Qigong for cancer treatment: A systematic review of controlled clinical trials. Acta Oncologica, 46, 717–722.
- Lee, M. S., Pittler, M. H., Guo, R., & Ernst, E. (2007). Qigong for hypertension: A systematic review of randomized clinical trials. Journal of Hypertension, 25, 1525–32.
- Lee, M. S., Pittler, M. H., Taylor-Piliae, R. E., & Ernst, E. (2007). Tai chi for cardiovascular disease and its risk factors: A systematic review. Journal of Hypertension, 25, 1974–1975.
- Leitan, N.D., & Murray, G. (2014). The mind-body relationship in psychotherapy: Grounded cognition as an explanatory framework. Frontiers In Psychology, 5(472), 69–76.
- Loy, D. (1997). Nonduality: A study in comparative philosophy. New Jersey: Humanities Press.
- Manzoni, G. M., Pagnini, F., Castelnuovo, G., & Molinari, E. (2008). Relaxation training for anxiety: A ten-years systematic review with meta-analysis. BioMed Central Psychiatry, 8(41), 1–12.
- Muehsam, D., Lutgendorf, S., Mills, P. J., Rickhi, B., Chevalier, G., Bat, N., … & Gurfein, B. (2017). The embodied mind: A review on functional genomic and neurological correlates of mind-body therapies. Neuroscience and Biobehavioral Reviews, 73, 165–181.
- Nguyen-Feng, V. N., Clark, C. J., & Butler, M. E. (2019). Yoga as an intervention for psychological symptoms following trauma: A systematic review and quantitative synthesis. Psychological Services, 16(3), 513–524.
- Ng, B. (2018). The neuroscience of growth mindset and intrinsic motivation. Brain Sciences, 8(2), 20.
- Nussbaum, A. D., & Dweck, C. S. (2008). Defensiveness versus remediation: Self-theories and modes of self-esteem maintenance. Personality and Social Psychology Bulletin, 34(5), 599–612.
- Peter, J., Fournier, C., Keip, B., Rittershaus, N., Stephanou-Rieser, N., Durdevic, M., … & Moser, G. (2018). Intestinal microbiome in irritable bowel syndrome: Before and after gut-directed hypnotherapy. International Journal of Molecular Sciences, 19, 3619.
- Porges, S. W. (2001). The polyvagal theory: Phylogenetic substrates of a social nervous system. International Journal of Psychophysiology, 42(2), 123–146.
- Pressman, S. D., & Black, L. L. (2012). Positive emotions and immunity. In S. C. Segerstrom (Ed.), The Oxford handbook of psychoneuroimmunology (pp. 92–104). New York: Oxford University Press.
- Pressman, S. D., & Cohen, S. (2005). Does positive affect influence health? Psychological Bulletin, 131(6), 925–971.
- Prinz, J. (2004). Embodied emotions. In R. C. Solomon (Ed.), Thinking about feeling: Contemporary philosophers on emotions. Series in affective science. New York: Oxford University Press.
- Saoji, A. A., Raghavendra, B. R., & Manjunath, N. K. (2019). Effects of yogic breath regulation: A narrative review. Journal of Ayurveda and Integrative Medicine, 10(1), 50–58.
- Shields, S. A., & Kappas, A. (2006). Magda B. Arnold’s contributions to emotions research. Cognition and Emotion, 20(7), 898–901.
- Vancampfort, D., Vansteelandt, K., Scheewe, T., Probst, M., Knapen, J., De Herdt, A., & De Hert, M. (2012). Yoga in schizophrenia: A systematic review of randomized controlled trials. Acta Psychiatrica Scandinavica, 126(1), 12–20.
- Westphal, J. (2016). The mind-body problem. Massachusetts Institute of Technology. Massachussets: MIT Press Books.
- Xia, J., & Grant, T. J. (2009). Dance therapy for schizophrenia. Cochrane Database of Systematic Reviews, 1, 1–9.
- Zaccaro, A., Piarulli, A., Laurino, M., Garbella, E., Menicucci, D., Neri, B., & Gemignani, A. (2018). How breath control can change your life: A systematic review of psycho-physiological correlates of slow breathing. Frontiers of Human Neuroscience, 12, 353, 1–16.
- Zeng, X., Chiu, C. P., Wang, R., Oei, T. P., & Leung, F. Y. (2015). The effect of loving-kindness meditation on positive emotions: A meta-analytic review. Frontiers in Psychology, 6, 1693, 1–14.
Let us know your thoughts
Read other articles by their category
- Body & Brain (49)
- Coaching & Application (57)
- Compassion (26)
- Counseling (51)
- Emotional Intelligence (24)
- Gratitude (18)
- Grief & Bereavement (21)
- Happiness & SWB (40)
- Meaning & Values (26)
- Meditation (20)
- Mindfulness (45)
- Motivation & Goals (45)
- Optimism & Mindset (34)
- Positive CBT (28)
- Positive Communication (20)
- Positive Education (47)
- Positive Emotions (32)
- Positive Leadership (18)
- Positive Parenting (4)
- Positive Psychology (33)
- Positive Workplace (37)
- Productivity (16)
- Relationships (46)
- Resilience & Coping (36)
- Self Awareness (21)
- Self Esteem (38)
- Strengths & Virtues (31)
- Stress & Burnout Prevention (34)
- Theory & Books (46)
- Therapy Exercises (37)
- Types of Therapy (64)





What our readers think
Broad and concise amongs all the other sources. Thank you
Thanks for this very valuable research and proven work on the mind-body connection.
Thankyou for this wonderful article and your indepth research on recent studies. I’ll use this for my further research
Is an excellent article, the content is easy to read and very informative. It can be used as teaching resourcr