Anxiety Therapy: Types, Techniques, and Worksheets
 Suffering from anxiety generally involves worry, fear, and rumination about the future.
Suffering from anxiety generally involves worry, fear, and rumination about the future.
Such anticipatory anxiety makes enjoying each moment a difficult endeavor. Unfortunately, anxiety disorders represent a serious and prevalent problem for children and adults worldwide.
The lifetime prevalence rate for anxiety disorders is estimated at 33.7% of the population—an estimate that has remained quite stable over the years (Bandelow & Michaelis, 2015).
Overall, anxiety disorders represent the most common psychiatric disorders within the general population (Öst, 2008), and the number one mental disorder among women (Chambala, 2008).
While anxiety may serve a useful purpose (e.g., alerting us to dangers), too much anxiety impairs functioning and performance in certain activities (Yerkes & Dodson, 1908).
If you are depressed you are living in the past. If you are anxious you are living in the future. If you are at peace you are living in the present.
Lao Tzu
When anxiety reaches the clinical level, it interferes with the ability to live life to the fullest, often causing significant social and occupational impairment. Anxiety disorders cover a lot of territories:
- Generalized anxiety disorder
- Panic disorders
- Post-traumatic stress disorder (PTSD)
- Specific phobias
- Social anxiety disorder
- Obsessive-compulsive disorder
Anxiety disorders may be terrifying for their victims, causing physiological, cognitive, and emotional symptoms (Hart, 1999). Those experiencing panic attacks often end up in the emergency room, believing they are dying. It is also common for anxiety disorders to occur concomitantly with other disorders such as depression.
On the positive side, there are several effective therapeutic approaches for anxiety disorders, as well as a variety of techniques and worksheets individuals may apply themselves.
This article will describe these approaches while also addressing the specific issues of social and childhood anxiety disorders. By shedding light on anxiety disorders and their treatment, the goal is to provide useful suggestions, tools, and above all, hope for individuals negatively impacted by these conditions.
Before you continue, we thought you might like to download our three Positive Psychology Exercises for free. These science-based exercises will explore fundamental aspects of positive psychology including strengths, values, and self-compassion, and will give you the tools to enhance the wellbeing of your clients, students, or employees.
This Article Contains:
- Can Anxiety Be Cured With Therapy?
- 6+ Popular Anxiety Therapy Options
- Exposure Treatment for Anxiety
- 14+ Techniques for Treating Anxiety
- 9 Useful Worksheets for Your Sessions
- Helpful Exercises
- A Look at Anxiety Group Therapy + Ideas
- A Note on Art Therapy for Anxiety
- 17 Creative Art and Music Therapy Ideas
- Treating Child Anxiety
- A Note on E-Therapy for Anxiety
- A Take-Home Message
- References
Can Anxiety Be Cured With Therapy?
While anxiety covers a range of areas and may be debilitating, it is highly treatable.
Despite the enormous stressors of modern society, there are ways to respond without succumbing to serious anxiety problems. Anxiety has been described as “the absence of the happy messengers that keep us tranquil” (Hart, 1999, p. 5).
Rebuilding such tranquility is possible thanks to a number of psychological treatment approaches. This article will focus on the non-pharmaceutical approaches that have been found effective for reducing and even curing individuals of anxiety disorders and associated symptomatology.
6+ Popular Anxiety Therapy Options
Man is not worried by real problems so much as by his imagined anxieties about real problems.
Epictetus
Severe anxiety is generally more a reflection of worry about anxiety itself as opposed to the problem underneath.
For example, an individual with a public speaking phobia is typically terrified of looking like a fool in front of an audience because of their anxiety symptoms (e.g., hyperventilating, throwing up, passing out, sweating, stuttering, etc.).
It is not fear of public speaking per se that is the real problem, but rather, the anticipation of associated anxiety that causes distress. It is by confronting such anxiety that individuals often experience relief.
Although the nature of intervention needs to be individualized based on the particular type of anxiety disorder, the following anxiety treatments can be effective for many people.
1. Cognitive therapy
Cognitive therapy is the most common psychological treatment for anxiety disorders.
This approach involves working with therapists to identify the feelings, thoughts, and beliefs that impact an individual’s ability to modify behaviors. For example, a person with a phobia of dogs would work to uncover the irrational beliefs that surround this phobia, such as the inherent danger in approaching all dogs.
Cognitive therapy is typically combined with behavior therapy to address beliefs and cognitions in conjunction with working toward ways of changing behaviors.
For example, the patient with the dog phobia might try approaching docile dogs while also working with a therapist on their irrational fears. This is an approach known as exposure therapy.
2. Cognitive-Behavioral Therapy
Cognitive-Behavioral Therapy (CBT) is widely used for anxiety disorders because it encompasses each of the underlying tenets that are related to clinical anxiety.
CBT is grounded in the following ideas:
- Mental health disorders involve key learning and information processing mechanisms (e.g., irrational beliefs about perceived dangers).
- Behaviors are better understood by exposing their true functions (e.g., examining the belief that sweating and heart palpitations will result in death).
- New adaptive learning experiences can be used to substitute prior nonadaptive learning processes (e.g., developing new beliefs about a feared object after increasing exposure).
- Clinicians take on a scientific approach to therapy by creating hypotheses about patients’ cognitive and behavioral patterns, intervening and observing outcomes, and reframing original hypotheses as needed (Hazlett-Stevens & Craske, 2004).
In this way, the CBT approach is tailored to the individual needs of the client and modified based on their progress (Hazlett-Stevens & Craske, 2004). CBT is grounded in the assumption that “emotional [i.e., anxiety] disorders are maintained by cognitive factors, and that psychological treatment leads to changes in these factors through cognitive and behavioral techniques” (Hofmann & Smits, 2008, p. 621).
CBT contains a variety of potential components:
- Exposure
- Social skills training
- Cognitive restructuring
- Problem-solving training
- Self-monitoring or journaling of symptoms
- Homework
- Relaxation training
Also, it may be implemented via brief therapy or over a longer duration depending upon the client and their presenting problems.
Meta-analyses have determined that CBT is an effective approach for the treatment of anxiety disorders (Butler, Chapman, Forman, & Beck, 2006; Deacon & Abramowitz, 2004; Hofmann & Smits, 2008; Stewart & Chambless, 2009).
In addition, CBT implemented by primary physicians with minimal mental health training (i.e., ‘The Calm Program’) has been reported as an acceptable and encouraging way for primary doctors to help anxious patients who might otherwise remain untreated (Craske et al., 2009).
3. Attention bias modification
Attention bias modification is a newly emerging approach that involves the use of computer-based attention training with patients with anxiety to affect hyper-attention to perceived threats in the environment (Bar-Haim, 2010).
In this way, problematic attentional biases can be modified to reduce anxiety.
Attention bias modification is similar to CBT because it involves exposure to feared objects or situations, but it is also unique because of its focus on specific attentional bias targets (Hakamata et al., 2010).
Although studies investigating this approach are minimal, attention bias modification represents a promising new approach for the treatment of anxiety disorders (Hakamata et al., 2010).
4. Hypnosis
Hypnosis has also been found to benefit individuals dealing with anxiety.
Hypnosis is “a state of consciousness involving focused attention and reduced peripheral awareness characterized by an enhanced capacity for response to suggestion” (Elkins, Barabasz, Council, & Spiegel, 2014, p. 6).
Hypnosis is like meditation, but with added objectives based on the needs of the individual. It may involve varying states of consciousness during which attention is focused and distractions are tuned out (McNeal, 2019).
Importantly, hypnosis is not an out-of-control experience, as the patient has power over and awareness of what’s going on. Additionally, its goals are achievable within a minimal time commitment (Straub & Bowman, 2016).
Hypnosis (including self-hypnosis) has been widely used within the mental health field (Valentine, Milling, Clark, & Moriarty, 2019). It has also been reported as a useful tool for patients dealing with the following:
- Dental anxiety (Potter, 2013)
- Surgical anxiety (Capafons & Mendoza, 2009)
- Anxiety related to sports competitions (Mendoza, 2010)
- Social phobia (Capafons & Mendoza, 2013)
- Anxiety disorders in general (Hammond, 2010)
5. Psychodynamic therapy
Psychodynamic therapy as a therapeutic approach often conjures up antiquated images of psychiatrist couches and patients reliving early childhood experiences. Psychodynamic therapy, which is rooted in Freudian theory, involves building strong therapist–patient alliances in which patients may develop the psychological tools needed to deal with fears and anxieties.
Although treatment may be lengthy, short-term psychodynamic therapy also has been reported as an effective approach for anxiety.
For example, one study reported that a 30-session psychodynamic treatment was helpful for the treatment of generalized anxiety – although this approach was less successful than CBT (Leichsenring et al., 2009).
Additionally, in a study examining long-term follow-up after psychodynamic therapy, significant reductions were reported for anxiety symptoms, with short-term approaches producing quicker improvements and long-term approaches providing longer lasting improvements (Knekt et al., 2008).
Finally, in a study comparing psychodynamic therapy with CBT, both approaches produced significant positive effects for social anxiety (Bögels, Wijts, Oort, & Sallaerts, 2014).
In contrast, a comparison of CBT and short-term psychodynamic therapy for patients with excessive health-related anxiety indicated significant improvements only for those who received CBT (Sørensen, Birket-Smith, Wattar, Buemann, & Salkovskis, 2010).
6. Vagus nerve stimulation
In this unique treatment approach, an anticonvulsant device sends electrical stimulation to the vagus nerve. The vagus nerve is targeted because of its ability to modulate anxiety.
Although this approach is typically used for epilepsy and treatment-resistant depression, studies have also demonstrated its effectiveness for treatment-resistant anxiety disorders (George et al., 2008).
Additionally, studies in which vagus nerve stimulation was used to treat epilepsy or depression have reported significant reductions in anxiety symptoms (Chavel, Westerveld, & Spencer, 2003; Rush et al., 2000).
Importantly, vagus nerve stimulation is an invasive approach that is used as an add-on treatment for patients who have not achieved success with CBT and other forms of therapy.
Exposure Treatment for Anxiety

With exposure therapy, the patient is exposed to their feared object or situation, such as flying.
Such exposure is typically gradual, with the exposure beginning with less threatening stimuli and gradually working its way toward increasingly feared stimuli (Wolpe, 1958).
This graduated exposure therapy is grounded in behavioral psychology, with the goal of desensitizing the patient to their feared trigger.
An example of graduated exposure therapy is that of an individual with arachnophobia. In this case, the patient might work with a therapist as follows:
- The patient first watches a film with giant spiders.
- The patient then views a large but harmless spider in a glass case across the room.
- The patient approaches and looks directly into the glass case.
- The patient works toward actually handling the spider.
Of course, the nature and duration of the arachnophobia exposure therapy will depend upon the patient’s individual symptoms and needs.
If systematic desensitization is used, gradual exposure will also involve relaxation techniques as a way of pairing the feared stimulus with a state that is not compatible with anxiety. Therefore, the patient might experience relaxation training while viewing spider images.
Like CBT, there are different ways in which exposure therapy may be implemented depending upon the client and diagnosis. For example, exposure therapy may be in vivo, as is the case with the live spider. Simulated exposure is a similar technique in which the patient experiences a proxy of the feared stimuli. For example, viewing a film of spiders is a simulated exposure.
Recent technology has provided therapists with the tools to implement more realistic simulations via virtual reality exposure therapy.
In such cases, patients wear headsets in which they experience a highly realistic virtual space. This technique is useful for several anxiety disorders and phobias; for example, military patients with PTSD can use virtual reality to simulate battlefield experiences.
Research studies have shown support for virtual reality exposure therapy in the treatment of anxiety disorders. For example, in a comprehensive meta-analysis, researchers found significant positive effects for virtual reality exposure therapy across outcomes (Powers & Emmelkamp, 2008).
Another type of exposure therapy is flooding.’ With this technique, patients confront their fears via simulated or in vivo exposure that is not gradual. Instead, patients are rapidly exposed to fear-provoking stimuli until they feel less anxious. For example, a patient with a bridge phobia is taken to a bridge and asked to stand on it until their anxiety wanes.
Flooding is based on the idea that without engaging in avoidance, the patient’s fear will become extinguished (Abramowitz, Deacon, & Whiteside, 2019). Therapists generally prefer gradual exposure over flooding because the latter is intense and may have negative repercussions for patients not prepared for such direct and immediate exposure to feared stimuli.
Other forms of exposure therapy include prolonged exposure, which was designed for the treatment of PTSD. With prolonged exposure, both repeated in vivo and imaginal exposure are combined to enable the patient to experience trauma without the feared outcomes.
This technique has been widely used for the treatment of PTSD and is considered by many clinicians as the best option for this disorder (Van Minnen, Harned, Zoellner, & Mills, 2012).
In a meta-analysis examining prolonged exposure among PTSD patients, individuals in the prolonged exposure group experienced better results than 86% of those in control condition (Powers, Halpern, Ferenschak, Gillihan, & Foa, 2010).
Acceptance-based therapy is another CBT approach sometimes used together with in vivo or simulated exposure therapy. The goal of this relatively new approach is to help patients increase their willingness to experience anxiety as part of their exposure to feared situations (England et al., 2012).
For example, in a study examining the use of acceptance-based exposure therapy for individuals with public speaking phobias, participants received group-based therapy in which they experienced public speaking exposure combined with acceptance-based treatment aimed at promoting acceptance of distressing emotions and sensations associated with public speaking (England et al., 2012).
Participants who received acceptance-based exposure therapy, which seeks to promote ‘psychological flexibility,’ experienced significant improvements in public speaking confidence, skills, and associated emotions (England et al., 2012).
14+ Techniques for Treating Anxiety
If you want to conquer the anxiety of life, live in the moment, live in the breath.
Amit Ray
Along with CBT and other therapist-implemented approaches for anxiety, various additional techniques may help to ease symptoms. Here is a list of ideas:
Mindfulness approaches involve a type of awareness in which a person pays attention to their feelings and thoughts in the moment and without judgment. It is an open-minded and totally accepting way of responding to thoughts (Kabat-Zinn, 2005).
Mindfulness techniques may be beneficial to patients with anxiety by helping to increase relaxation while removing negative or stressful judgments. Mindfulness may be enhanced by using various approaches, such as meditation, yoga, or deep-breathing exercises.
While mindfulness activities are often add-ons with CBT and other forms of therapy, there is recent evidence supporting their unique benefit for the reduction of anxiety (Blanck et al., 2018).
Engaging in aerobic exercise also represents a useful way to reduce physiological stress responses and improve mood (Sharma, Madaan, & Petty, 2006). While it may be difficult for an anxious person to find the motivation to exercise, its potential benefits make it worth the effort.
Physical activity is linked to reduced anxiety symptomatology, as well as improved cognitive functioning, life satisfaction, and psychological wellbeing (Carek, Laibstain, & Carek, 2011).
Exercise is beneficial for anxiety disorders, including obsessive-compulsive disorder, generalized anxiety disorder, and social anxiety disorder (Baldwin et al., 2014).
Exercise has also been associated with reduced anxiety symptoms among sedentary patients with medical conditions (Baldwin et al., 2014).
Exercise is especially attractive because it’s cost-effective and may be performed in a variety of ways. While exercise may not reap the same benefits for patients with anxiety as CBT or other psychological approaches, it may enhance the impact of such treatment.
Along with mindfulness techniques and aerobic exercise, here are a variety of things that individuals can do to reduce anxiety:
- Get involved in a hobby you love (e.g., baking, gardening, reading, painting, etc.).
- Listen to your favorite music.
- Journal your feelings.
- Take a warm bath.
- Make sure to eat healthy, as junk food can have adverse effects on physical and psychological health.
- Get enough sleep.
- Go out in nature.
- Avoid emotional triggers (e.g., people and places that consistently increase your anxiety).
- Spend time with animals.
- Organize your home or workspace, as clutter may exacerbate anxiety.
- Watch caffeine and alcohol intake.
- Spend time with family and friends whom you enjoy.
Techniques for treating social anxiety
Social anxiety is a prevalent problem, with over 7% of Americans diagnosed with social anxiety disorder (Norton, 2012).
Social anxiety may take several forms, such as a fear of public speaking, social situations, or meeting new people.
Social anxiety stems from an individual’s fear of adverse judgments or scrutiny from others and the humiliation that follows. As such, social phobia may lead to significant problems within occupational, educational, and social domains, which often result in low self-esteem and loneliness.
The best treatment for social anxiety is CBT, with exposure therapy often recommended.
For example, an individual with public speaking anxiety might work on speaking in front of a few people and gradually work their way up to larger groups.
Socially anxious people may also benefit from social skills and relaxation training.
For example, in an in-depth meta-analysis, including 30 studies and 1,628 respondents, Acarturk, Cuijpers, van Straten, and de Graaf (2008) investigated various social anxiety treatments.
Therapy intervention methods included CBT, cognitive restructuring, exposure therapy, social skills training, and applied relaxation training.
The authors found the psychological treatments to be highly effective for social anxiety disorder, with no differences between treatment types (likely because so many studies used combined treatments). Lower effectiveness was noted for patients with more severe social anxiety disorder (Acarturk et al., 2008).
In another study, which was randomized with a one-year follow-up, Anderson et al. (2013) compared in vivo exposure with virtual reality exposure for the treatment of social anxiety.
Anderson et al. (2013) reported significant improvements at 12-month follow-up, with virtual reality therapy functioning equally well as in vivo exposure. Research also has indicated that attentional bias training for social anxiety is related to significant reductions in social anxiety symptoms (Schmidt, Richey, Buckner, & Timpano, 2009).
In sum, while social anxiety disorder often results in severe impairment, there are psychological treatments that have been found to diminish significantly associated symptomatology and enhance the quality of life for many individuals.
9 Useful Worksheets for Your Sessions
There are numerous worksheets that may be useful for reducing anxiety. Here are several examples:
- The Anxiety Workbook: A 7-Week Plan to Overcome Anxiety, Stop Worrying, and End Panic (Cuncic, 2017)
- Jane’s Worry Elephant: A Self-Help Guide for Kids with Anxiety (Miller, 2019)
- The Worry Workbook for Kids: Helping Children to Overcome Anxiety and the Fear of Uncertainty (Khanna & Ledley, 2018)
- Conquer Anxiety Workbook for Teens: Find Peace From Worry, Panic, Fear, and Phobias (Chansard, 2019)
- The 5-Minute Anxiety Relief Journal: A Creative Way to Stop Freaking Out (Peterson, 2019)
- The Anxiety and Worry Workbook: The Cognitive Behavioral Solution (Clark & Beck, 2011)
- The Generalized Anxiety Disorder Workbook: A Comprehensive CBT Guide for Coping with Uncertainty, Worry, and Fear (Robichaud & Dugas, 2015)
- The Anxiety and Phobia Workbook (Bourne, 2015)
- Let That Sh*t Go: A Journal for Leaving Your Bullsh*t Behind and Creating a Happy Life (Sweeney, 2018)
Helpful Exercises
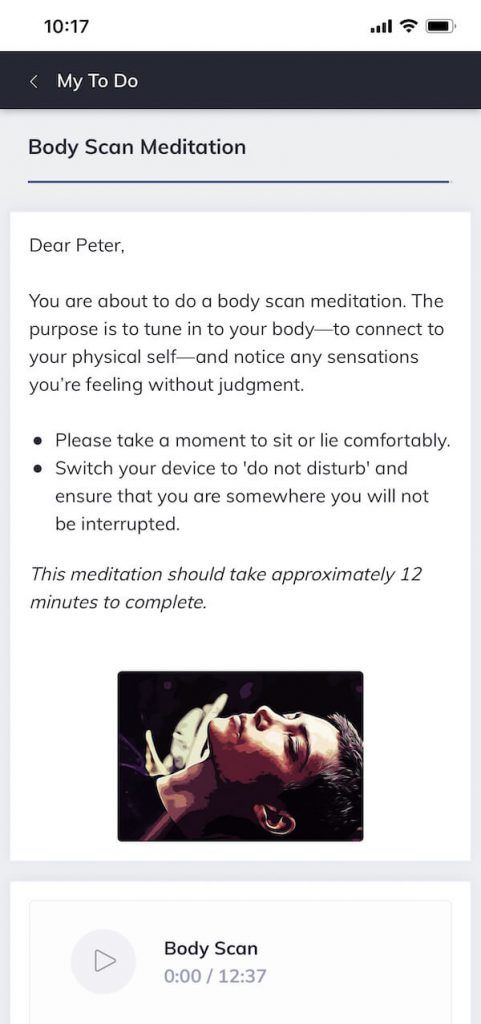
Because such activities may be conducted as needed and for free, they represent highly feasible ways to deal with anxiety issues.
Many therapists will prescribe self-guided mindfulness and meditation exercises for clients to complete between in-person therapy sessions or as a tool to help during moments of intense anxiety.
With the rise in digital technologies, such as smartphones and blended care e-therapy platforms like Quenza (pictured here), the prescription of take-home interventions such as these is becoming increasingly more common and convenient.
While the potential value of self-guided exercise has face validity, standalone exercises performed outside of treatment intervention have rarely been researched.
However, in a meta-analysis of 18 studies, standalone exercises were found to be beneficial for the reduction of anxiety (Blanck et al., 2018).
The standalone mindfulness exercises included breathing meditation, sitting meditation, body scan (gradually attending to different parts of the body) and sound scan (mindfulness that adjusts responses to sounds so their aversive impact is reduced).
Blanck et al.’s (2018) study shows that there are positive ways for individuals to deal with their anxiety on their own, outside of a structured intervention.
If you are feeling anxious or stressed, you can search and apply various exercises based on your unique interests and needs. Here are some examples:
- Deep-breathing meditation
- Sitting meditation
- Body scan meditation
- Loving-kindness meditation
- Spiritual meditation
- Vipassana meditation
- Transcendental meditation
- Mantra meditation
- Walking meditation
- Buddhist meditation
- Yoga
Quick-start guide to anxiety treatment – Therapy in a Nutshell
A Look at Anxiety Group Therapy + Ideas
Psychological treatment options for anxiety include both individual and group-based therapies.
Norton (2012) describes effective evidence-based approaches designed to help CBT therapists implement group-based interventions for patients with anxiety disorders.
Such group treatment approaches (e.g., exposure, cognitive restructuring, mindfulness, etc.) are useful for all anxiety disorders; there is no need to apply separate strategies for specific anxiety disorders (Norton, 2012).
For CBT group therapy to be effective, the group needs to be both cohesive and task focused. Other key group therapy factors include altruism, imitative behaviors, interpersonal learning, and installation of hope (Yalom, 1995).
While there is more research examining one-on-one CBT therapy for anxiety than for group therapy (Whitefield, 2010), the latter approach has some advantages:
- Cost-effectiveness
- The ability to reach more people
- May facilitate the normalization of behaviors (e.g., by seeing that others have the same problems)
- The acceptance of challenges that are elicited by peers versus the therapist
- Positive reinforcement by multiple people
- Exposure situations that are more easily recreated within a group setting
- The ability to exercise problem-solving skills by making suggestions to other group members (Whitefield, 2010)
While many individuals with anxiety disorders may benefit from group CBT, there are some people for whom group therapy is likely to be less effective, such as those with co-morbid psychological disorders, more severe and chronic presentation of problems, negative core beliefs, communication problems, interpersonal issues, active suicidal ideation, fear of group environments, extreme stress, or poor relationships (Moorey, 1996).
Additionally, individuals who lack the motivation to change or fail to comply with treatment are less likely to be a good match for group CBT (Moorey, 1996).
Group-based CBT as useful for the treatment of social anxiety disorders (Butler et al., 2018; Hedman et al., 2011).
In addition, preliminary research suggests that large-group CBT classes represent highly feasible and useful approaches for individuals with anxiety disorders (Palay et al., 2018).
In terms of key ingredients for group CBT as a treatment for social anxiety, researchers examined mechanisms for change for two group-based approaches: CBT, and mindfulness and acceptance-based therapy.
Results indicated that mindfulness and acceptance were fundamental mechanisms of change for both group approaches, whereas cognitive reappraisal was more important for CBT (Kocovski, Fleming, Hawley, Ho, & Antony, 2015).
Finally, a qualitative study examined perceptions among individuals with anxiety disorders who achieved benefits following group CBT (Abrahamsson, Nordling, & Michelsen et al., 2018).
Respondents described their anxiety as a lack of security and noted that creating a securing group environment involved the following themes:
- Sharing with others (e.g., getting to know others with similar problems)
- Knowledge given to participants (e.g., as related to the link between anxiety and thoughts, behaviors, health, and lifestyle)
- Structure (e.g., how instructors responded to participants’ needs and provided acceptable structures for group members to practice on their own; Abrahamsson et al., 2018)
Overall, if you are dealing with anxiety and feel that group therapy is a good fit for you, there is likely a group that will meet your needs. Once you do some research and find groups that interest you, it is also a good idea to try out several until you find the best fit.
A Note on Art Therapy for Anxiety

There is a certain magic in the act of creating; young children expressing themselves through art appear not to have a care in the world.
Indeed, the therapeutic benefit in the creation of art transcends age and talent. There are two important reasons that art therapy is a viable approach for anxious individuals:
- It enables a type of self-expression that goes beyond words.
- Visual representations of anxiety aid in the application of certain types of therapy (Chambala, 2008).
Art therapy has also been described as creating a cathartic release of positive feelings (Curl, 2008). Research supports this idea, as art therapy has been found effective for the reduction of anxiety and other psychological symptoms across multiple populations.
Here are some noteworthy examples:
- Engaging in art such as coloring mandalas, making collages, and modeling with clay is associated with reduced anxiety among college students (Sandmire, Gorham, Rankin, & Grimm, 2012).
- Creating art such as ‘healthy image posters,’ greeting cards, and silk wall hangings is related to reduced anxiety among family caregivers of cancer patients (Walsh, Martin, & Schmidt, 2004).
- Participation in group art therapy is related to the reduction of symptomatology among adult psychiatric outpatients primarily diagnosed with depressive, anxiety, and adjustment disorders (Chandraiah, Anand, & Avent, 2012).
- Engaging in art therapy is related to the reduction of overall state anxiety among adult cancer patients (Nainis et al., 2006).
- Creating art is related to reduced levels of perceived stress among Canadian college students (Abbott, Shanahan, & Neufeld, 2013).
- Making pottery is related to reduced anxiety among elderly nursing home residents (Doric-Henry, 1997).
- Engaging in art-therapy-based supervision among end-of-life care workers is associated with reduced anxiety and enhancement of emotional awareness and regulation (Potash, Ho, Chan, Wang, & Cheng, 2014).
- Art therapy incorporated into brief CBT among individuals with anxiety disorders is associated with reduced frequency of panic attacks (Morris, 2014).
- Simply being exposed to visual art has been shown to reduce anxiety symptoms among psychiatric inpatients (Nanda, Eisen, Zadeh, & Owen, 2010), a finding that attests to the powerful healing power of art.
17 Creative Art and Music Therapy Ideas
The function of music is to liberate in the soul those feelings which normally we keep locked up in the heart.
Sebastian Faulks
Music does have a way of changing moods, whether this means sinking into the angst of the blues or experiencing the upbeat feelings of disco. Because of its ability to affect mood, music therapy has been used to help patients deal with a variety of psychological problems.
Music therapy basically consists of “the monitored use of music to promote clinical change” (Bulfone, Quattrin, Zanotti, Regattin, & Brusaferro, 2009, p. 238). Music therapy can be used in multiple ways, such as in combination with CBT or other types of therapy.
Performing music may also foster positive feelings that promote healing. The efficacy of music therapy for the reduction of anxiety is also supported by scientific literature.
For example, music has been found to reduce anxiety among cancer patients receiving chemotherapy (Bulfone et al., 2009; Karagozoglu, Tekyasar, & Yilmaz, 2012), physiological signs of anxiety among patients receiving mechanical ventilatory support (Korhan, Khorshid, & Uyar, 2011), and anxiety among patients with Alzheimer’s disease (Guétin et al., 2009).
Additionally, music therapy is associated with reduced anxiety among individuals with psychiatric disorders (de l’Etoile, 2002; Bibb, Castle, & Newton, 2015; Shiranibidabadi & Mehryar, 2015).
There are many ways we can enhance our moods with the use of music; here are some ideas:
- Pick music that fits your mood or activity, such as upbeat music for exercise and classical music for relaxation.
- Try meditative music before sleeping.
- Take dance lessons.
- If you are anxious or angry while driving, pick music that will calm your nerves.
- Do not expose yourself to others’ music if it causes stress.
- Use music while creating art as a way of adding inspiration.
Similarly, there are several ways you might engage in creative art as a way of promoting positive wellbeing.
Here are a few ideas:
- Pottery
- Origami
- Collage making
- Painting or drawing
- Building with Legos or Lincoln Logs
- Beading
- Making paper airplanes
- Scrapbooking
- Knitting
- Stained glass making
- Sewing or quilting
Treating Child Anxiety

As with adults, childhood anxiety disorders cause significant impairment and are often unrecognized (Walkup et al., 2008).
Rapee et al. (2009) note that childhood anxiety has a negative impact on peer relationships, school functioning, and family processes. Childhood anxiety disorders also commonly occur in conjunction with other psychological diagnoses and have been linked to inhibited temperament (Rapee et al., 2009).
The most common childhood anxiety disorders include separation anxiety, phobias, social anxiety disorder, generalized anxiety disorder, obsessive-compulsive disorder, and PTSD.
As with adults, childhood anxiety disorders are often successfully treated using CBT or skill-focused treatment, both of which are sometimes combined with pharmacological treatment.
In a randomized, controlled study of 488 children with anxiety disorders, CBT, both alone and in combination with antidepressant therapy, was related to significant reductions in anxiety severity as compared to a no-treatment comparison group (Walkup et al., 2008).
Similarly, among children with anxiety disorders, responsiveness to CBT during childhood has been associated with reductions in anxiety during adulthood (Benjamin, Harrison, Settipani, Brodman, & Kendall, 2013).
In a study examining the long-term effects of CBT combined with parental anxiety management, children who received the combined treatment were significantly less likely to be diagnosed with an anxiety disorder three years later (Cobham, Dadds, Spence, & McDermott, 2010).
Interestingly, the combined therapy was significantly more effective than the CBT treatment alone, which makes sense given that psychological symptoms in parents are related to treatment outcomes among children with anxiety (Berman, Weems, Silverman, & Kurtines, 2000).
Along with parental influences, the quality of peer friendships has also been found to predict better CBT treatment responses among kids with anxiety disorders (Baker & Hudson, 2013).
While there is some evidence that children with particular anxiety disorders (e.g., obsessive-compulsive disorder) may benefit from pharmacological treatment (especially selective serotonin re-uptake inhibitors), quality studies examining the effects of psychotropic medication for the treatment of pediatric anxiety are scarce (Reinblatt & Riddle, 2007).
There is, however, evidence that CBT is an effective treatment for children with anxiety disorders, with long-term benefits often noted (Muris, Meesters, & van Melick, 2002). Moreover, CBT is particularly effective for treating childhood anxiety disorders when combined with family training (Muris et al., 2002).
A Note on E-Therapy for Anxiety
With the large numbers of individuals with anxiety disorders who remain undiagnosed and untreated, psychologists have attempted to find more effective ways to provide treatment.
This point is particularly salient concerning anxiety disorders, as the inability to engage in treatment outside the home is often inherent in the disorder itself.
Fortunately, technology has created an avenue in which individuals with anxiety disorders may be reached. By delivering therapist-guided CBT via the computer (
For example, in a study examining a 10-week dose of iCBT among participants with generalized anxiety, iCBT was associated with significant positive treatment effects comparable to those found for in-person treatment (Robinson et al., 2010). Similarly, CBT e-therapy has been reported as effective for the treatment of obsessive-compulsive disorder, PTSD, social anxiety, and generalized anxiety (Klein, Meyer, Austin, & Kyrios, 2011).
Finally, in a comprehensive review of 26 randomized controlled studies of internet therapy, 23 studies reported positive results for the treatment of depression or anxiety symptoms (Griffiths, Farrer, & Christensen, 2010). Preliminary findings for the efficacy of internet-based treatment provides promise for adults and children experiencing the often debilitating effects of anxiety disorders.
A Take-Home Message
Anxiety symptoms and clinical anxiety disorders are highly prevalent and often debilitating.
Fortunately, these conditions are absolutely treatable. Effective treatment options include CBT, attention bias modification, hypnosis, psychodynamic therapy, and vagus nerve stimulation.
The psychological treatment approach with the most scientific support for anxiety disorders is CBT. Consequently, CBT is often the treatment of choice among therapists specializing in anxiety issues.
CBT may take many forms, with exposure therapy often reported as highly successful for the reduction of anxiety. Exposure therapy may be enhanced with other therapeutic approaches, such as relaxation training and acceptance-based therapy. There is also support for the efficacy of group CBT for the treatment of anxiety, especially when groups are both cohesive and task focused.
Anxiety disorders are common among children, with the most frequent diagnoses including separation anxiety, phobias, social anxiety, generalized anxiety, obsessive-compulsive disorder, and PTSD. Research similarly indicates that CBT has long-term benefits for kids, especially when combined with family therapy. Along with CBT, art and music therapy also represent research-based approaches found to soothe an anxious mind.
In addition, there are various things individuals can do on their own to relieve anxiety, such as deep breathing, aerobic exercise, meditation, yoga, enjoying a hobby, listening to music, etc.
Finally, anxiety treatment has been dramatically advanced by technology, with e-therapy (especially iCBT) reaching larger audiences than possible with face-to-face therapy. Overall, given the preponderance of evidence supporting anxiety-focused treatment, those with anxiety disorders or symptoms have much reason to be hopeful about the promise of a tomorrow without suffering.
We hope you enjoyed reading this article. Don’t forget to download our three Positive Psychology Exercises for free.
- Abbott, K. A., Shanahan, M. J., & Neufeld, R. W. J. (2013). Artistic tasks outperform non-artistic tasks for stress reduction. Art Therapy, 30, 71–78.
- Abrahamsson, C., Nordling, B., Michelsen, C. S., & Norlander, T. (2018). Patients’ experiences after cognitive behavior group therapy: From anxiety to feelings of perceived security. Psychology, 9, 1176–1193.
- Abramowitz, J., Deacon, B., & Whiteside, S. (2019). Exposure therapy for anxiety, second edition: Principles and practice. Guilford Press.
- Acarturk, C., Cuijpers, P., van Straten, A., & de Graaf, R. (2008). Psychological treatment of social anxiety disorder: A meta-analysis. Psychological Medicine, 39(2), 241–254.
- Anderson, P. L., Price, M., Edwards, S. M., Obasaju, M. A., Schmertz, S. K., Zimand, E., & Calamaras, M. R. (2013). Virtual reality exposure therapy for social anxiety disorder: A randomized controlled trial. Journal of Consulting and Clinical Psychology, 81, 751–760.
- Baker, J. R., & Hudson, J. L. (2013). Friendship quality predicts treatment outcome in children with anxiety disorders. Behaviour Research and Therapy, 51, 31–36.
- Baldwin, D. S., Anderson, I. M., Nutt, D. J., Allgulander, C., Bandelow, B., den Boer, J., … Wittchen, H.U. (2014). Evidence-based pharmacological treatment of anxiety disorders, post-traumatic stress disorder and obsessive-compulsive disorder: A revision of the 2005 guidelines from the British Association for Psychopharmacology. Journal of Psychopharmacology, 28, 403–439.
- Bandelow, B., & Michaelis, S. (2015). Epidemiology of anxiety disorders in the 21st century. Dialogues in Clinical Neuroscience, 17, 327–335.
- Bar-Haim, Y. (2010). Research review: Attention bias modification (ABM): A novel treatment for anxiety disorders. Journal of Child Psychology and Psychiatry, 51, 859–870.
- Benjamin, C. L., Harrison, J. P., Settipani, C. A., Brodman, D. M., & Kendall, P. C. (2013). Anxiety and related outcomes in young adults 7 to 19 years after receiving treatment for child anxiety. Journal of Consulting and Clinical Psychology, 81(5), 865–876.
- Berman, S. L., Weems, C. F., Silverman, W. K., & Kurtines, W. M. (2000). Predictors of outcome in exposure-based cognitive and behavioral treatments for phobic and anxiety disorders in children. Behavior Therapy, 31, 713–731.
- Bibb, J., Castle, D., & Newton, R. (2015). The role of music therapy in reducing post-meal related anxiety for patients with anorexia nervosa. Journal of Eating Disorders, 3, 50.
- Blanck, P., Perleth, S., Heidenreich, T., Kröger, P., Ditzen, B., Bents, H., & Mander, J. (2018). Effects of mindfulness exercises as stand-alone intervention on symptoms of anxiety and depression: Systematic review and meta-analysis. Behaviour Research and Therapy, 102, 25–35.
- Bögels, S. M., Wijts, P., Oort, F. J., & Sallaerts, S. J. M. (2014). Psychodynamic psychotherapy versus cognitive behavior therapy for social anxiety disorder: An efficacy and partial effectiveness trial. Depression and Anxiety, 31, 363–373.
- Bourne, E. (2015). The anxiety and phobia workbook. New Harbinger.
- Bulfone, T., Quattrin, R., Zanotti, R., Regattin, L., & Brusaferro, S. (2009). Effectiveness of music therapy for anxiety reduction in women with breast cancer in chemotherapy treatment. Holistic Nursing Practice, 23, 238–242.
- Butler, A., Chapman, J., Forman, E., & Beck, A. (2006). The empirical status of cognitive-behavioral therapy: A review of meta-analyses. Clinical Psychology Review, 26, 17–31.
- Butler, R. M., Boden, M. T., Olino, T. M., Morrison, A. S., Goldin, P. R., Gross, J. J., & Heimberg, R. G. (2018). Emotional clarity and attention to emotions in cognitive-behavioral group therapy and mindfulness-based stress reduction for social anxiety disorder. Journal of Anxiety Disorders, 55, 31–38.
- Capafons, A., & Mendoza, M. (2009). The Valencia model of waking hypnosis and its clinical applications. In G. Koester and P. Delisle (Eds.), Hypnosis: Theories, research, and applications. Nova Science.
- Capafons, A., & Mendoza, M. (2013). Waking hypnosis. In M. V. Costa Ferreira (Ed.), Manual Brasileiro de hipnose clínica. Atheneu.
- Carek, P. J., Laibstain, S. E., & Carek, S. M. (2011). Exercise for the treatment of depression and anxiety. The International Journal of Psychiatry in Medicine, 41, 15–28.
- Chambala, A. (2008). Anxiety and art therapy: Treatment in the public eye. Art Therapy, 25, 187–189.
- Chandraiah, S., Anand, S. A., & Avent, L. C. (2012). Efficacy of group art therapy on depressive symptoms in adult heterogeneous psychiatric outpatients. Art Therapy, 29(2), 80–86.
- Chansard, T. (2019). Conquer anxiety workbook for teens: Find peace from worry, panic, fear, and phobias. Althea Press.
- Chavel, S. M., Westerveld, M., & Spencer, S. (2003). Long-term outcome of vagus nerve stimulation for refractory partial epilepsy. Epilepsy and Behavior, 4, 302–309.
- Clark, D., & Beck, A. (2011). The anxiety and worry workbook: The cognitive-behavioral solution. Guilford Press.
- Cobham, V. E., Dadds, M. R., Spence, S. H., & McDermott, B. (2010). Parental anxiety in the treatment of childhood anxiety: A different story three years later. Journal of Clinical Child and Adolescent Psychology, 39(3), 410–420.
- Craske, M. G., Roy-Byrne, P. P., Stein, M. B., Sullivan, G., Sherbourne, C., & Bystritsky, A. (2009). Treatment for anxiety disorders: Efficacy to effectiveness to implementation. Behaviour Research and Therapy, 47, 931–937.
- Cuncic, A. (2017). The anxiety workbook: A 7-week plan to overcome anxiety, stop worrying, and end panic. Althea Press.
- Curl, K. (2008). Assessing stress reduction as a function of artistic creation and cognitive focus. Art Therapy, 25, 164–169.
- de l’Etoile, S. K. (2002). The effectiveness of music therapy in group psychotherapy for adults with mental illness. The Arts in Psychotherapy, 29, 69–78.
- Deacon, B. J., & Abramowitz, J. S. (2004). Cognitive and behavioral treatments for anxiety disorders: A review of meta-analytic findings. Journal of Clinical Psychology, 60(4), 429–441.
- Doric-Henry, L. (1997). Pottery as art therapy with elderly nursing home residents. Art Therapy, 14, 163–171.
- Elkins, G. R., Barabasz, A. F., Council, J. R., & Spiegel, D. (2014). Advancing research and practice: The revised APA Division 30 definition of hypnosis. International Journal of Clinical and Experimental Hypnosis, 63, 1–9.
- England, E. L., Herbert, J. D., Forman, E. M., Rabin, S. J., Juarascio, A., & Goldstein, S. P. (2012). Acceptance-based exposure therapy for public speaking anxiety. Journal of Contextual Behavioral Science, 1, 66–72.
- George, M. S., Ward, H. E., Ninan, P. T., Pollack, M., Nahas, Z., Anderson, B., … Ballenger, J. C. (2008). A pilot study of vagus nerve stimulation (VNS) for treatment-resistant anxiety disorders. Brain Stimulation, 1, 112–121.
- Griffiths, K., Farrer, L., & Christensen, H. (2010). The efficacy of internet interventions for depression and anxiety disorders: A review of randomised controlled trials. The Medical Journal of Australia, 192, S4–S11.
- Guétin, S., Portet, F., Picot, M. C., Pommié, C., Messaoudi, M., Djabelkir, L., … Touchon, J. (2009). Effect of music therapy on anxiety and depression in patients with Alzheimer’s type dementia: Randomised, controlled study. Dementia and Geriatric Cognitive Disorders, 28, 36–46.
- Hakamata, Y., Lissek, S., Bar-Haim, Y., Britton, J. C., Fox, N. A., Leibenluft, E., … Pine, D. S. (2010). Attention bias modification treatment: A meta-analysis toward the establishment of novel treatment for anxiety. Biological Psychiatry, 68, 982–990.
- Hammond, D. C. (2010). Hypnosis in the treatment of anxiety- and stress-related disorders. Expert Review of Neurotherapeutics, 10, 263–273.
- Hart, A. (1999). The anxiety cure. Thomas Nelson.
- Hazlett-Stevens, H., & Craske, M. (2004). Chapter 1 brief cognitive-behavioral therapy: Definition and scientific foundations. Retrieved from http://citeseerx.ist.psu.edu/viewdoc/summary?doi=10.1.1.529.3790
- Hedman, E., Andersson, G., Ljótsson, B., Andersson, E., Rück, C., Mörtberg, E., & Lindefors, N. (2011). Internet-based cognitive behavior therapy vs. cognitive-behavioral group therapy for social anxiety disorder: A randomized controlled non-inferiority trial. PLoS ONE, 6.
- Hofmann, S. G., & Smits, J. A. (2008). Cognitive-behavioral therapy for adult anxiety disorders: A meta-analysis of randomized placebo-controlled trials. The Journal of Clinical Psychiatry, 69, 621–632.
- Kabat-Zinn, J. (2005). Coming to our senses. Hyperion.
- Karagozoglu, S., Tekyasar, F., & Yilmaz, F. A. (2012). Effects of music therapy and guided visual imagery on chemotherapy-induced anxiety and nausea-vomiting. Journal of Clinical Nursing, 22, 39–50.
- Khanna, M., & Ledley, D. (2018). The worry workbook for kids: Helping children to overcome anxiety and the fear of uncertainty. New Harbinger.
- Klein, B., Meyer, D., Austin, D., & Kyrios, M. (2011). Anxiety online—A virtual clinic: Preliminary outcomes following completion of five fully automated treatment programs for anxiety disorders and symptoms. Journal of Medical Internet Research, 13, e89.
- Knekt, P., Lindfors, O., Härkänen, T., Välikoski, M., Virtala, E., Laaksonen, M. A., … the Helsinki Psychotherapy Study Group (2008). Randomized trial on the effectiveness of long-and short-term psychodynamic psychotherapy and solution-focused therapy on psychiatric symptoms during a 3-year follow-up. Psychological Medicine, 38, 689–703.
- Kocovski, N. L., Fleming, J. E., Hawley, L. L., Ho, M. H. R., & Antony, M. M. (2015). Mindfulness and acceptance-based group therapy and traditional cognitive-behavioral group therapy for social anxiety disorder: Mechanisms of change. Behaviour Research and Therapy, 70, 11–22.
- Korhan, E. A., Khorshid, L., & Uyar, M. (2011). The effect of music therapy on physiological signs of anxiety in patients receiving mechanical ventilatory support. Journal of Clinical Nursing, 20, 1026–1034.
- Leichsenring, F., Salzer, S., Jaeger, U., Kächele, H., Kreische, R., Leweke, F., … Leibing, E. (2009). Short-term psychodynamic psychotherapy and cognitive-behavioral therapy in generalized anxiety disorder: A randomized, controlled trial. American Journal of Psychiatry, 166, 875–81.
- McNiff, S. (2005). Art heals: How creativity cures the soul. Shambhala.
- Mendoza, M. (2010). Application and results of the Valencia model of waking hypnosis in four clinical cases. In A. Capafons, Advances in Experimental and Applied Hypnosis. Symposium conducted at the VII Iberoamerican Congress of Psychology, Oviedo, Spain.
- Moorey, S. (1996). Cognitive behaviour therapy for whom? Advances in Psychiatric Treatment, 2, 17–23.
- Morris, F. J. (2014). Should art be integrated into cognitive behavioral therapy for anxiety disorders? The Arts in Psychotherapy, 41, 343–352.
- Muris, P., Meesters, C., & van Melick, M. (2002). Treatment of childhood anxiety disorders: A preliminary comparison between cognitive-behavioral group therapy and a psychological placebo intervention. Journal of Behavior Therapy and Experimental Psychiatry, 33, 143–158.
- Nainis, N., Paice, J. A., Ratner, J., Wirth, J. H., Lai, J., & Shott, S. (2006). Relieving symptoms in cancer: Innovative use of art therapy. Journal of Pain and Symptom Management, 31, 162–169.
- Nanda, U., Eisen, S., Zadeh, R., & Owen, D. (2010). Effect of visual art on patient anxiety and agitation in a mental health facility and implications for the business case. Journal of Psychiatric and Mental Health Nursing, 18, 386–393.
- Norton, P. (2012). Group cognitive-behavioral therapy of anxiety: A transdiagnostic treatment manual. Guilford Press.
- Öst, L. G. (2008). Cognitive behavior therapy for anxiety disorders: 40 years of progress. Nordic Journal of Psychiatry, 62, 5–10.
- Palay, J., Wong, J. Y., Randall, J. R., Sala, T., Bolton, J. M., Furer, P., … Sareen, J. (2018). Feasibility of large group cognitive behavioural therapy education classes for anxiety disorders. European Journal for Person Centered Healthcare, 6, 274–278.
- Peterson, T. (2019). The 5-minute anxiety relief journal: A creative way to stop freaking out. Rockridge Press.
- Potash, J. S., Ho, A. H., Chan, F., Wang, X. L., & Cheng, C. (2014). Can art therapy reduce death anxiety and burnout in end-of-life care workers? A quasi-experimental study. International Journal of Palliative Nursing, 20, 233–240.
- Potter, C. (2013). Using hypnosis in dentistry. Dental Nursing, 3, 522–526.
- Powers, M. B., & Emmelkamp, P. M. G. (2008). Virtual reality exposure therapy for anxiety disorders: A meta-analysis. Journal of Anxiety Disorders, 22, 561–569.
- Powers, M. B., Halpern, J. M., Ferenschak, M. P., Gillihan, S. J., & Foa, E. B. (2010). A meta-analytic review of prolonged exposure for posttraumatic stress disorder. Clinical
Psychology Review, 30, 635–641. - Rapee, R. M., Schniering, C. A., & Hudson, J. L. (2009). Anxiety disorders during childhood and adolescence: Origins and treatment. Annual Review of Clinical Psychology, 5, 311–341.
- Reinblatt, S. P., & Riddle, M. A. (2007). The pharmacological management of childhood anxiety disorders: A review. Psychopharmacology 191, 67–86.
- Robichaud, M., & Dugas, M. (2015). The generalized anxiety disorder workbook: A comprehensive CBT guide for coping with uncertainty, worry, and fear. New Harbinger.
- Robinson, E., Titov, N., Andrews, G., McIntyre, K., Schwencke, G., & Solley, K. (2010). Internet treatment for generalized anxiety disorder: A randomized controlled trial comparing clinician vs. technician assistance. PLoS ONE, 5.
- Rush, A., George, M., Sackeim, H., Marangell, L., Husain, N., Giller, C., … Goodman, R. (2000). Vagus nerve stimulation (VNS) for treatment-resistant depressions: A multicenter study. Biological Psychiatry, 47, 276–286.
- Sandmire, D. A., Gorham, S. R., Rankin, N. E., & Grimm, D. R. (2012). The influence of art-making on anxiety: A pilot study. Art Therapy, 29, 68–73.
- Schmidt, N. B., Richey, J. A., Buckner, J. D., & Timpano, K. R. (2009). Attention training for generalized social anxiety disorder. Journal of Abnormal Psychology, 118, 5–14.
- Sharma, A., Madaan, V., & Petty, F. (2006). Exercise for mental health. Primary Care Companion to the Journal of Clinical Psychiatry, 8, 106.
- Shiranibidabadi, S., & Mehryar, A. (2015). Music therapy as an adjunct to standard treatment for obsessive-compulsive disorder and co-morbid anxiety and depression: A randomized clinical trial. Journal of Affective Disorders, 184, 13–17.
- Sørensen, P., Birket-Smith, M., Wattar, U., Buemann, I., & Salkovskis, P. (2010). A randomized clinical trial of cognitive behavioural therapy versus short-term psychodynamic psychotherapy versus no intervention for patients with hypochondriasis. Psychological Medicine, 41, 431–441.
- Stewart, R. E., & Chambless, D. L. (2009). Cognitive-behavioral therapy for adult anxiety disorders in clinical practice: A meta-analysis of effectiveness studies. Journal of Consulting and Clinical Psychology, 77, 595–606.
- Straub, W. F., & Bowman J. J. (2016). A review of the development of sport hypnosis as a performance enhancement method for athletes. Journal of Psychology and Clinical Psychology, 6(6). Retrieved from https://medcraveonline.com/JPCPY/JPCPY-06-00378.pdf
- Sweeney, M. (2018). Let that sh*t go: A journal for leaving your bullsh*t behind and creating a happy life. St. Martin’s Press.
- Valentine, K., Milling, L., Clark, L., & Moriarty, C. (2019). The efficacy of hypnosis as a treatment for anxiety: A meta-analysis. International Journal of Clinical and Experimental Hypnosis, 67, 336–363.
- Van Minnen, A., Harned, M. S., Zoellner, L., & Mills, K. (2012). Examining potential contraindications for prolonged exposure therapy for PTSD. European Journal of Psychotraumatology, 3.
- Walkup, J. T., Albano, A. M., Piacentini, J., Birmaher, B., Compton, S. N., Sherrill, J. T., … Kendall, P. C. (2008). Cognitive-behavioral therapy, Sertraline, or a combination in childhood anxiety. New England Journal of Medicine, 359, 2753–2766.
- Walsh, S. M., Martin, S. C., & Schmidt, L. A. (2004). Testing the efficacy of a creative-arts intervention with family caregivers of patients with cancer. Journal of Nursing Scholarship, 36, 214–219.
- Whitefield, G. (2010). Group cognitive–behavioural therapy for anxiety and depression. Advances in Psychiatric Treatment, 16, 219–227.
- Wolpe, J. (1958). Psychotherapy by reciprocal inhibition. Stanford University Press.
- Yalom, I. (1995). The theory and practice of group psychotherapy. Basic Books.
- Yerkes, R. M., & Dodson, J. D. (1908). The relation of strength of stimulus to rapidity of habit-formation. Journal of Comparative Neurology and Psychology, 18, 459–482.
Let us know your thoughts
Read other articles by their category
- Body & Brain (49)
- Coaching & Application (57)
- Compassion (26)
- Counseling (51)
- Emotional Intelligence (24)
- Gratitude (18)
- Grief & Bereavement (21)
- Happiness & SWB (40)
- Meaning & Values (26)
- Meditation (20)
- Mindfulness (45)
- Motivation & Goals (45)
- Optimism & Mindset (34)
- Positive CBT (28)
- Positive Communication (20)
- Positive Education (47)
- Positive Emotions (32)
- Positive Leadership (18)
- Positive Parenting (4)
- Positive Psychology (33)
- Positive Workplace (37)
- Productivity (16)
- Relationships (46)
- Resilience & Coping (36)
- Self Awareness (21)
- Self Esteem (37)
- Strengths & Virtues (31)
- Stress & Burnout Prevention (34)
- Theory & Books (46)
- Therapy Exercises (37)
- Types of Therapy (64)






What our readers think
Exploring the nuances of anxiety therapy in your blog was incredibly insightful. From outlining various types and techniques to providing practical worksheets, it’s a comprehensive guide for anyone seeking support. Your clarity and depth make navigating anxiety management feel less daunting. Thank you for this valuable resource!
Thanks for always sharing your insights, being selfless, and spreading kindness. I personally can’t thank you enough for all of the amazing content you share. You change lives! WE APPRECIATE YOU. Stay safe!
How do you find a good iCBT for children?
Hi Jill,
Good question. While I’m not sure what the prevalence of iCBT services for children is (and it will depend somewhat on your country of residence), I’m aware that many face-to-face CBTs are switching to teletherapy as a result of COVID-19. So, a general suggestion I’d make is that if you have trouble finding online child CBT specialists, try doing a more general search for child CBTs and sending out some inquiries about whether they’ve moved online. Hope his helps!
– Nicole | Community Manager